Crohn's disease is a chronic inflammatory process that can affect any part of the digestive tract and its most frequent location is the terminal ileum.1
Oropharyngeal and esophageal involvement is rare (0.2-11%) and 80% of these cases are associated with synchronous lesions in the terminal ileum that develop up to 3 months after upper tract symptom onset.2 It is considered a poor outcome marker due to its aggressiveness, diagnostic delay, and the delay in and poor response to treatment. It presents in younger patients and has greater complications.3
Taking into account the low prevalence of upper gastrointestinal involvement, its greater aggressiveness, and the difficulty in making accurate diagnosis, which can result in greater morbidity and mortality, we present herein a clinical case of oropharyngeal and esophageal Crohn's disease, diagnosed after the presentation of acute abdomen due to intestinal perforation.
A 60-year-old man was seen in the otorhinolaryngology department for dysphagia and odynophagia associated with the presence of aphthous lesions in the labial mucosa, the floor of the mouth, and the amygdala. He had anorexia, asthenia, a 20kg weight loss, no abdominal symptoms, and poor response to symptomatic treatment. Lesion biopsies were taken and left amygdalectomy was performed. The findings in the histopathologic study were consistent only with chronic inflammation.
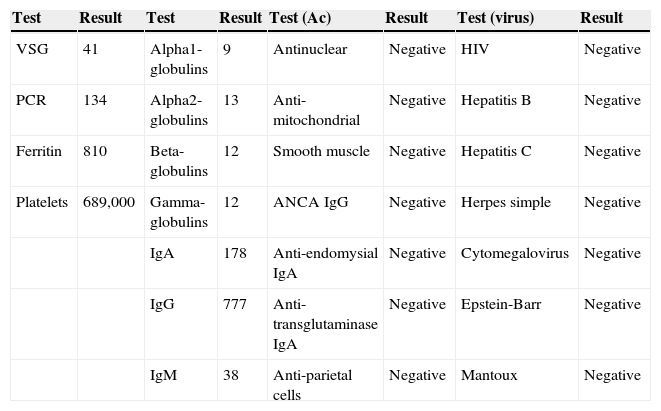
The patient was studied in the dermatology and internal medicine departments and infectious pathology and sexually transmitted disease were ruled out. He was referred to the gastroenterology department due to the suspicion of inflammatory bowel disease (Table 1).
Acute-phase immunologic and reagent tests performed on the patients as outpatients.
| Test | Result | Test | Result | Test (Ac) | Result | Test (virus) | Result |
|---|---|---|---|---|---|---|---|
| VSG | 41 | Alpha1-globulins | 9 | Antinuclear | Negative | HIV | Negative |
| PCR | 134 | Alpha2-globulins | 13 | Anti-mitochondrial | Negative | Hepatitis B | Negative |
| Ferritin | 810 | Beta-globulins | 12 | Smooth muscle | Negative | Hepatitis C | Negative |
| Platelets | 689,000 | Gamma-globulins | 12 | ANCA IgG | Negative | Herpes simple | Negative |
| IgA | 178 | Anti-endomysial IgA | Negative | Cytomegalovirus | Negative | ||
| IgG | 777 | Anti-transglutaminase IgA | Negative | Epstein-Barr | Negative | ||
| IgM | 38 | Anti-parietal cells | Negative | Mantoux | Negative |
Results of the outpatient analytic tests. Biochemistry and immunology.
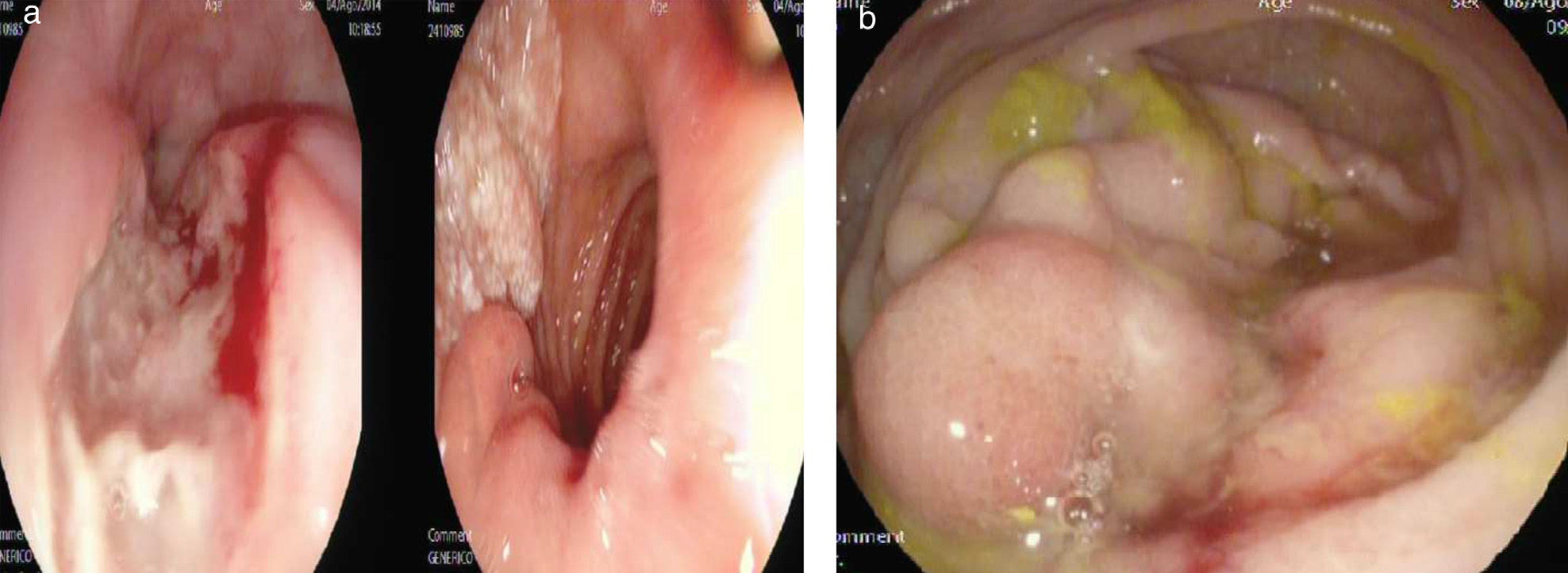
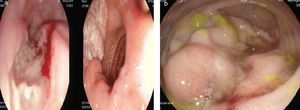
Upper gastrointestinal endoscopy was performed that revealed several large, deep, ulcerated lesions in the proximal esophagus, with raised edges and a fibrinous base (fig. 1a). The digestive study was completed with lower gastrointestinal endoscopy that showed the presence of a stricturing, friable, non-ulcerated cecal lesion that impeded the passage of the endoscope (fig. 1b).
The patient came to the emergency department 24h after colonoscopy due to intense, colicky pain in the hypogastrium. Physical examination revealed dehydration, pallor and sweating, fever (38.5°C), and low blood pressure (BP 90/55mmHg). The abdomen was peritonitic (diffuse pain with abdominal guarding and rebound tenderness).
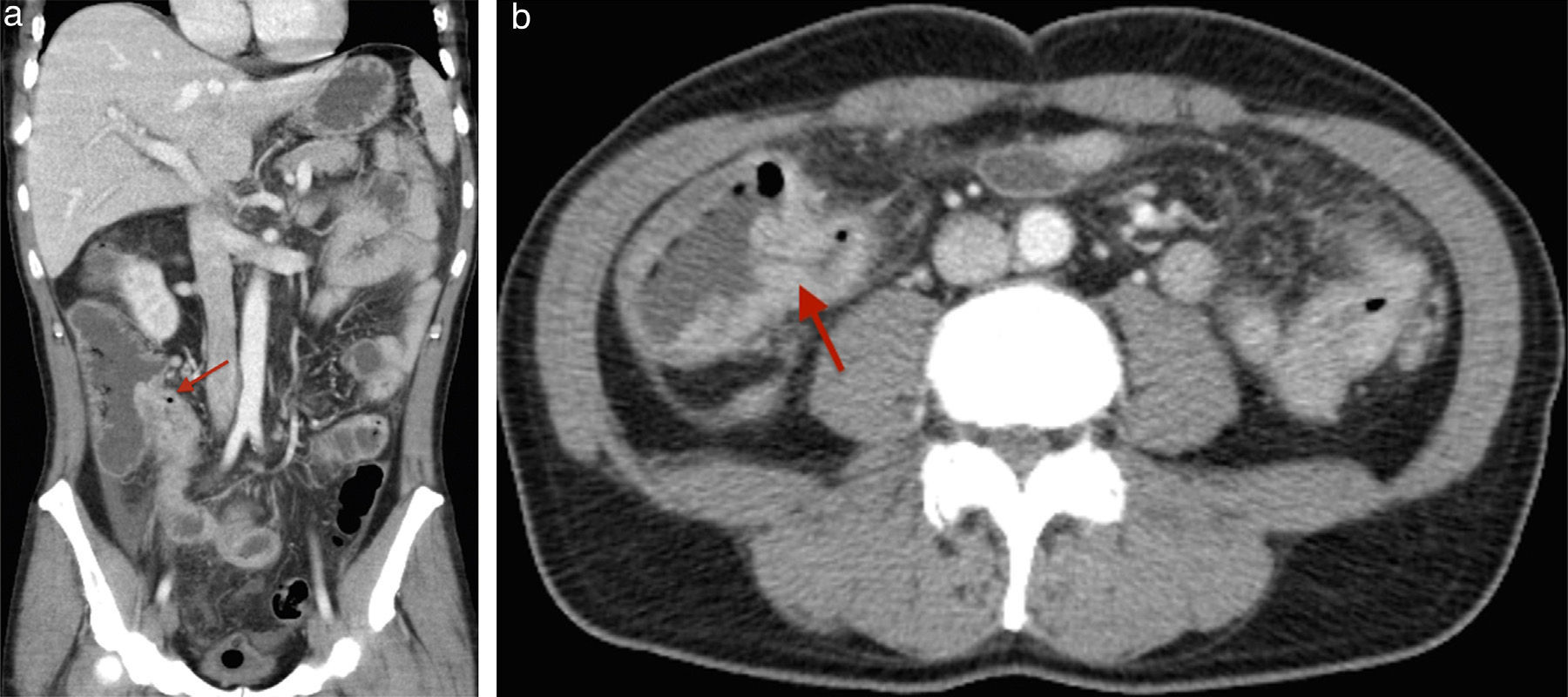
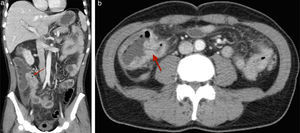
Emergency hemogram showed a left shift with no leukocytosis. With the suspicion of an eventual post-endoscopic complication, an abdominal CT scan was done that identified pneumoperitoneum, free fluid, and thickening of the terminal ileum and Bauhin's valve (a finding in concordance with the endoscopy) (figs. 2a and 2b). Emergency surgery was performed that revealed peritonitis secondary to a punctiform perforation in the terminal ileum 5cm from the ileocecal valve associated with the presence of multiple small ulcerous lesions and a stricturing cecal lesion. Right colectomy with ileocolic anastomosis was performed.
In the early postoperative period the patient presented with rectorrhagia without hemodynamic instability and had analytic parameters suggestive of sepsis: leukopenia, coagulopathy, and thrombocytopenia. The patient underwent blood product transfusion and wide-spectrum antibiotic treatment, reversing the sepsis and stopping the hemorrhagic complication.
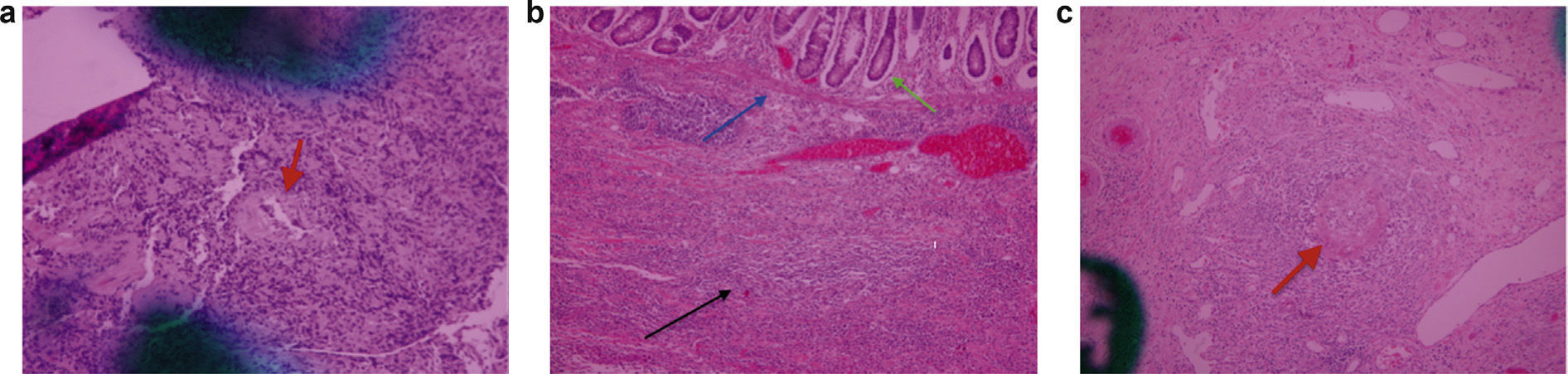
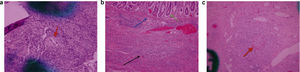
The anatomopathologic study of the endoscopic esophageal biopsy (fig. 3a) and the surgical specimen showed a transmural colitis and inflammatory bowel disease consistent with Crohn's disease, with reactive lymphadenitis and tubular adenoma with low-grade dysplasia in hyperplastic sessile polyps 2cm from the ileocecal valve (figs. 3b and 3c).
a) Microscopic study with hematoxylin-eosin stain, x100: endoscopic esophageal biopsy with non-caseating granuloma in the submucosa (indicated by the red arrow). b) Microscopic study with hematoxylin-eosin stain, x100: chronic leukocyte infiltration with transmural involvement: mucosa (green arrow), submucosa (blue arrow), and muscle layer (black arrow) in the surgical specimen (right colon and terminal ileum). c) Microscopic study with hematoxylin-eosin, x100: non-caseating granuloma in the small bowel (red arrow).
The patient was released from the hospital 14 days after surgery, receiving medical treatment with deflazacort and prednisone (60mg) on a tapering schedule. He was re-admitted 10 days later due to inability to eat that improved with azathioprine and continued after his release. Progressive thrombocytopenia was observed during follow-up that was associated with azathioprine and the therapeutic regimen was modified; the corticoid therapy continued and infliximab treatment was begun, with good clinical response. The oral and esophageal lesions disappeared, along with the associated symptoms (odynophagia and dysphagia). There was adequate digestive tolerance with nutritional status recovery and weight gain (13kg). No anastomotic complications were seen in the barium swallow study and colonoscopy.
The lapse of time from symptom onset to final diagnosis and instauration of adequate medical treatment was 26 months.
Crohn's disease is a chronic, segmental, transmural inflammation with the formation of non-caseating granulomas of the digestive tract that can affect any part of it, from the mouth to the anus, and its most frequent location is the terminal ileum (80%). It can present at any age and peaks between the ages of 15-25 years. It presents in outbreaks and its etiology is still unknown.
In its typical form, patients present with colicky abdominal pain, diarrhea, weight loss, and anemia. Diagnosis is established through endoscopic procedures and biopsy. Oropharyngeal and esophageal involvement at the onset of Crohn's disease is rare (0.5-20% and 0.2-3%, respectively).1 In fact, the esophagus is the least frequent location and is almost always associated with ileal involvement. It is characterized by the appearance of ulcerous lesions in up to 60% of cases, accompanied with dysphagia and odynophagia.3,4 Diagnosis is established when endoscopy and biopsy of the ulcerous lesions show a chronic, transmural, lymphocytic infiltrate and the characteristic granulomas.
Nevertheless, early diagnosis at this location is a significant challenge. The scant prevalence of involvement of the first portions of the digestive tract makes a rule-out diagnosis of other diseases with oral and esophageal ulcerations essential, such as: infectious esophagitis (tuberculosis, toxoplasmosis, syphilis, cytomegalovirus, herpes simple), sarcoidosis, Behçet disease, chemical burns, and neoplasias.5
On the other hand, studies that usually enable diagnosis of ileal Crohn's disease (endoscopy and biopsy) frequently have a lower performance in this location. Endoscopic lesions that include erythema, aphthae, and linear erosions and ulcerations at a distance from the gastroesophageal junction are identified through gastroscopy in less than 50% of the cases due to limited oropharyngeal examination during upper gastrointestinal endoscopy.
Esophageal disease has a higher predisposition to stricturing complications, greater aggressiveness with the formation of fistulas at the trachea, bronchial tubes, lungs, and stomach, and clinical onset in younger patients with a mean age of 35 years, a lower body mass index, and higher platelet count, indicative of a systemic inflammatory response. They are a poor outcome marker and therefore early treatment should be started, stepping up the therapy if there is no symptomatic or endoscopic improvement.1,5–7
Diagnosis is made through histologic study when typical non-caseating granulomas are observed. In the oropharyngeal location, this finding is quite variable (10-75%) and it is found in less than 25% of the cases in esophageal lesion biopsy, perhaps because they tend to settle in the deepest layers of the esophageal wall (submucosa and muscle), requiring thicker biopsies. Thus it is often that only a nonspecific chronic inflammatory infiltrate is observed that does not enable diagnosis.4
In our case, diagnosis was made 26 months after the appearance of the first manifestations (buccopharyngeal ulcers) and the first symptoms (dysphagia and odynophagia). The patient even underwent an amygdalectomy in which the histopathologic study could not establish the diagnosis.
The inability to make an early diagnosis in many of these cases means that once these patients are diagnosed, their disease will be more advanced (esophageal strictures and even fistulas have been described) or they will present with complications that can only be resolved through surgical treatment (esophageal perforations), without a doubt adding greater morbidity and even a possibly life-threatening situation.4,8
Our patient was diagnosed after presenting with peritonitis secondary to the perforation of an ileal lesion. There were severe complications in the postoperative period related to sepsis, which, even though they were satisfactorily resolved, there is little doubt that the progression of any of the untreated esophageal ulcers to perforation and the development of mediastinitis would have had a very negative impact on outcome.
The treatment of oral and esophageal Crohn's disease does not differ from that used in the most frequent forms of the disease. Basically, it employs glucocorticoids, acetylsalicylic acid derivatives (mesalazine and sulfasalazine), immunosuppressants (azathioprine), and biologic treatments (infliximab), reserving surgical operations for complicated cases or those with null response to drugs.4,9
Upper gastrointestinal lesions secondary to Crohn's disease become resistant to treatment in up to 21% of the cases, have complete clinical and endoscopic remission in 57%, and present at least one relapse of symptoms and lesions in 21%.10 In our case, medical treatment was established after the procedure, resulting in lesion and symptom remission.
And finally, we can conclude that oropharyngeal and esophageal involvement in Crohn's disease is rare and represents a diagnostic challenge due to the scant specificity of the clinical manifestations (aphthous ulcers), as well as the histologic findings (absence of granulomas), and also to the limited value of endoscopy and biopsy in that location, leading to late diagnosis with the consequent therapeutic and prognostic implications.
In cases such as ours, with oral lesions that do not respond to symptomatic treatment, with no accurate diagnosis, and with a biopsy excluding malignancy, the possibility of inflammatory bowel disease should be considered. Endoscopic and colonoscopic studies directed at discovering associated lesions primarily in the terminal ileum should be performed to make a correct diagnosis and begin early medical treatment. In this manner, remission is achieved and the progression into more advanced forms of the disease or the appearance of complications that require surgical treatment in a clinical situation of greater morbidity and mortality for the patient are prevented.
Financial disclosureNo financial support was received in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Loreto-Brand M, Fernández-Pérez A, Celeiro-Muñoz C, Álvarez-Castro A, Bustamante-Montalvo M. Enfermedad de Crohn: afectación gastrointestinal alta. Revista de Gastroenterología de México. 2015;80:282–285.