Intussusception is rare in adults and can occur in the small bowel and colon. Its atypical presentation makes the diagnosis difficult. The aim of the present study was to evaluate the causes, clinical characteristics, and treatment outcomes of adult intussusception and to determine whether there was an association between etiology and clinical presentation.
Materials and methodsA retrospective study was carried out on patients above 18 years of age that were treated for intussusception at a tertiary care hospital, between 2000 and 2020. The findings were summarized utilizing descriptive and inferential statistics.
ResultsTwenty-eight cases were identified. Median patient age was 46 years (18-80) and median symptom duration was 18 days. Abdominal pain was the most frequent symptom (96.42%). The intussusceptions registered were enteroenteric (14), ileocecal (4), ileocolonic (4), colocolonic (5), and colorrectal (1). Intussusception etiology was benign in 15 cases, 9 were associated with malignancy, and 4 were idiopathic. Surgery was performed on 11 patients with enteroenteric intussusception and on all the cases of ileocecal, ileocolonic, colocolonic, and colorectal intussusception. There were 2 events of perioperative mortality (8%) and 8 of postoperative morbidity (32%). No significant differences were found regarding symptom duration or length of hospital stay, when the etiologic groups were compared.
ConclusionsIntussusception is rare in adults. Diagnosis is a challenge because of the nonspecific signs and symptoms. Surgical resection should be considered in the definitive treatment and management should be individualized according to the patient’s comorbidities, clinical presentation, and risk of malignancy.
La intususcepción es infrecuente en adultos y puede ocurrir en intestino delgado y colon. Su presentación atípica hace complejo el diagnóstico. El objetivo de este estudio fue evaluar las causas, características clínicas, desenlaces del tratamiento y determinar si existe asociación entre etiología y presentación clínica.
Material y métodosEstudio retrospectivo en un centro de tercer nivel, en pacientes mayores de 18 años con intususcepción tratados entre 2000 y 2020. Se utilizó estadística descriptiva e inferencial para resumir los hallazgos.
ResultadosSe identificaron 28 casos, con mediana de edad de 46 años (18-80) y duración de síntomas 18 días. El dolor abdominal fue el síntoma más frecuente (96.42%). Se registraron 14 intususcepciones entero-entéricas, 4 ileocecales, 4 ileocolónicas, 5 colo-colónicas, y una colorrectal. Quince de las intususcepciones fueron de etiología benigna, 9 asociadas a malignidad y 4 idiopáticas. Se realizó cirugía en 11 pacientes con intususcepción entero-entérica y en todos los casos de intususcepción ileocecal, ileocolónica, colo-colónica y colorrectal. Se presentaron 2 eventos de mortalidad perioperatoria (8%) y 8 de morbilidad postoperatoria (32%). No hubo diferencia significativa en la duración de los síntomas, ni en estancia hospitalaria al comparar los grupos etiológicos.
ConclusionesLa intususcepción es rara en adultos. El diagnóstico es un reto debido a los signos y síntomas inespecíficos. Para el tratamiento definitivo, se debe considerar la resección quirúrgica, individualizando de acuerdo a las comorbilidades del paciente, presentación clínica y riesgo de malignidad.
Intussusception is uncommon in adults, compared with the pediatric population. Five percent of all intussusceptions are estimated to occur in adults, and cause approximately 5% of bowel obstructions.1,2
Intussusceptions may result from intestinal conditions that change the normal pattern of peristalsis.3
Preoperative diagnosis remains challenging due to the nonspecific clinical presentation and duration. Optimal treatment is controversial1 and also depends on the underlying disease and the need for surgical management.4
In the present study, we reviewed a case series of adult intussusception, with respect to etiology and treatment. Rectal intussusception was not addressed.
Materials and methodsPatientsA retrospective study of adult patients (≥ 18 years of age) that developed bowel intussusception between November 2000 and October 2020 was carried out. Diagnosis was confirmed by diagnostic imaging or intraoperatively, or both. We excluded patients with rectal intussusception. The study was approved by the institutional research ethics review board at the Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán. Informed consent was not issued to patients due to the retrospective nature of the study.
Medical dataThe patient characteristics collected from the data were age, sex, medical history, clinical symptoms, diagnostic approach, type of intussusception according to the lead point, definitive treatment, histopathologic findings, and postoperative courses.
Clinical featuresClinical presentation data included abdominal pain, nausea, vomiting, abdominal distention, constipation, diarrhea, gastrointestinal bleeding, symptom duration, diagnostic imaging methods employed to make the diagnosis, type of intussusception according to the site of the lead point, and etiology. The types of intussusception were: 1) enteroenteric, in which intussusception is confined to the small bowel, 2) ileocecal, in which the ileocecal valve leads the intussusception, 3) ileocolonic, in which the ileum invaginates through the ileocecal valve, 4) colocolonic, in which the intussusception is confined to the large bowel, and 5) colorectal, in which the colon invaginates through the rectum.5,6 Etiology was assessed by histopathology, dividing patients into benign, malignant, and idiopathic (clinical and imaging diagnosis without histopathologic confirmation) subgroups.
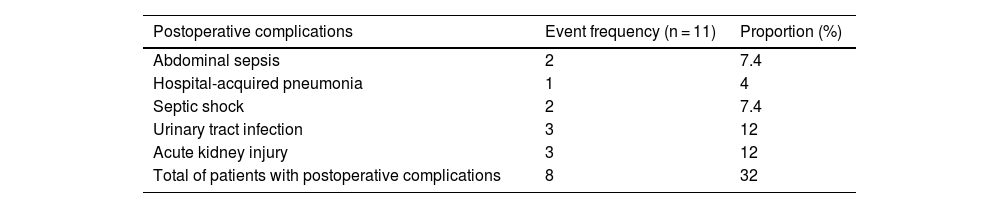
Treatment and outcomesTreatment of intussusception consisted of surgical or conservative management, which included bowel rest, intravenous fluids, pain management, and close monitoring. The complications of intussusception reported in the study were abdominal sepsis, hospital-acquired pneumonia, septic shock, urinary tract infection, and acute kidney injury. Perioperative 30-day mortality was reported.
Statistical analysisThe categorical variables were summarized using frequencies and proportions, and the continuous variables were summarized using medians and ranges. The Kruskal-Wallis test was utilized to compare the continuous variables. Length of hospital stay was subdivided into ≥ 7 days or < 7 days and the Fisher’s exact test was employed to assess a possible association between etiologic subtype and length of hospital stay. A p value < 0.05 was accepted as indicating statistical significance. The data analyses were performed using SPSS Statistics (version 25.0; Armonk, NY: IBM Corp.) software.
Ethical considerationsThe present study complies with the regulations of the ethics and research committee of the Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán.
Informed consent was not requested for the publication of this project, because it contains no personal data that could identify the patients.
ResultsClinical findingsThe youngest patient was 18 years old, and the oldest was 80 years old (a median age of 46 years), and the male/female ratio was 9:19.
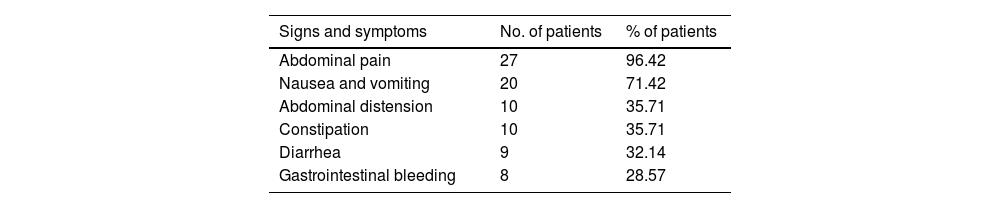
The most common symptom was abdominal pain in 96.42% of the patients, followed by nausea and vomiting in 71.42%. Other reported symptoms were abdominal distention, constipation, diarrhea, and bloody stools (Table 1). The median overall symptom duration reported by the patient from onset to diagnosis was 18 days (range, 1-365 days); 17.86% (n = 5) of the patients presented with acute symptoms, 17.86% (n = 5) with subacute symptoms, and 64.28% (n = 18) with chronic symptoms. Eleven patients (39.28%) had symptoms for more than one month.
Abdominal computed tomography (CT) was performed in 26 patients (92.85%). Small bowel follow-through study was performed in one patient, and intussusception was correctly diagnosed preoperatively, then confirmed during surgical management. Plain abdominal x-ray was performed in one patient, which showed suggestive findings of bowel obstruction; the diagnosis of bowel intussusception was made intraoperatively.
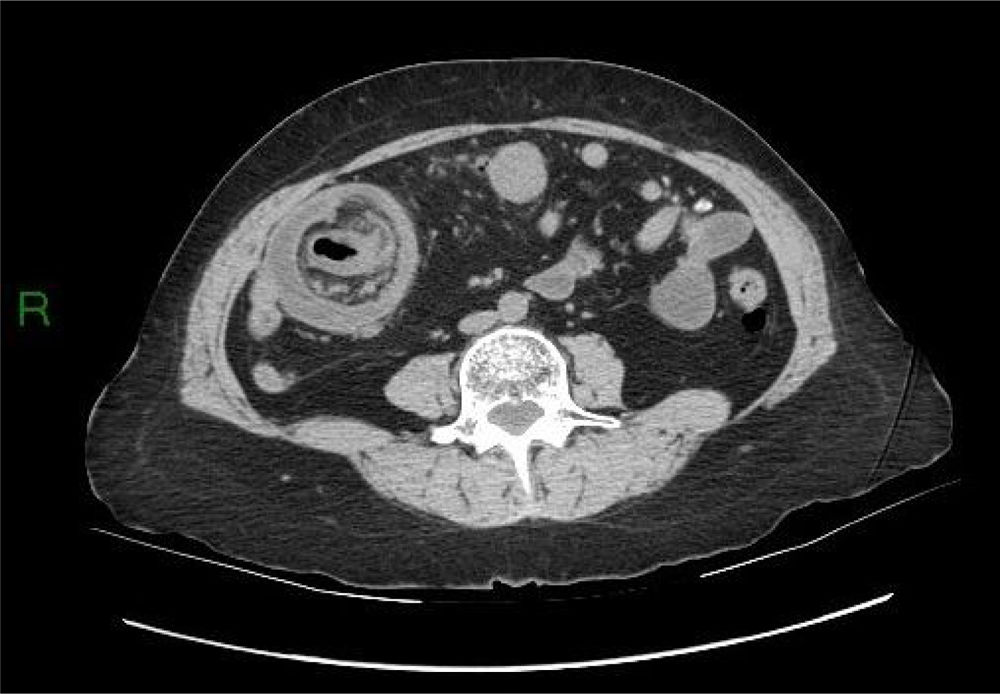
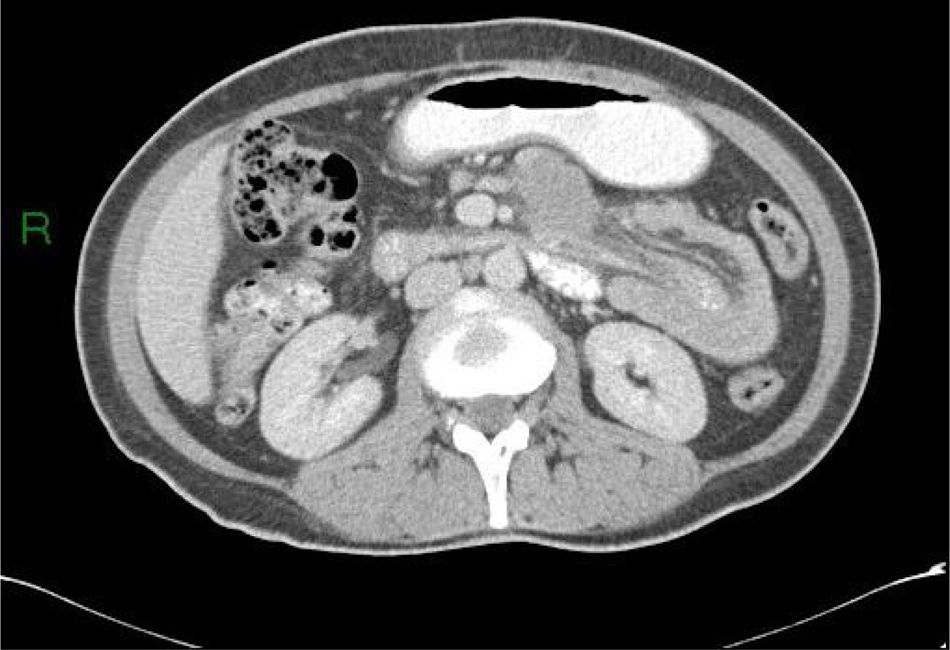
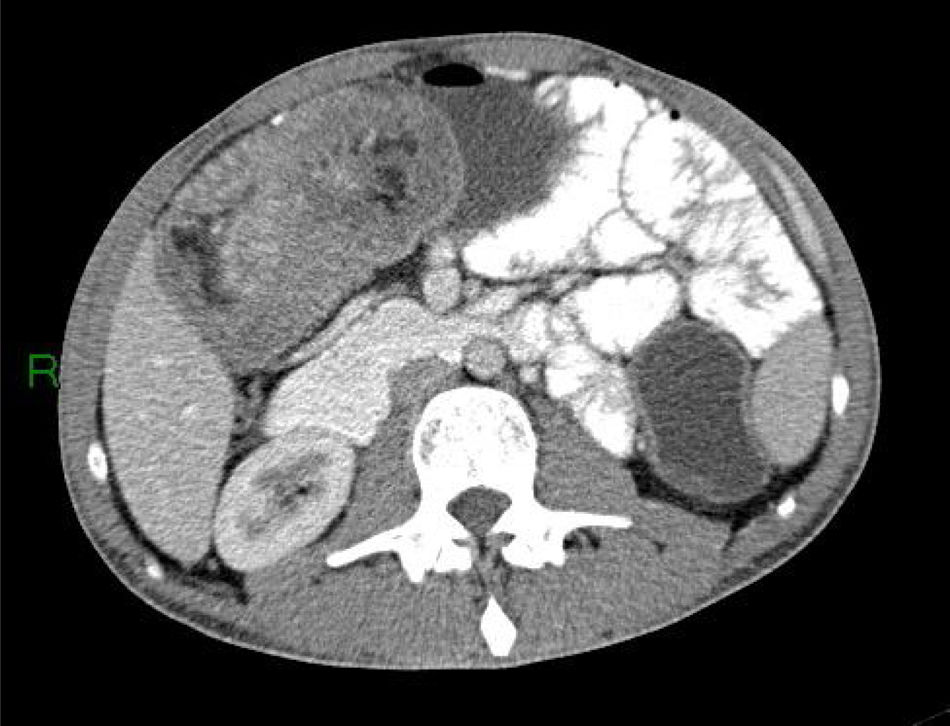
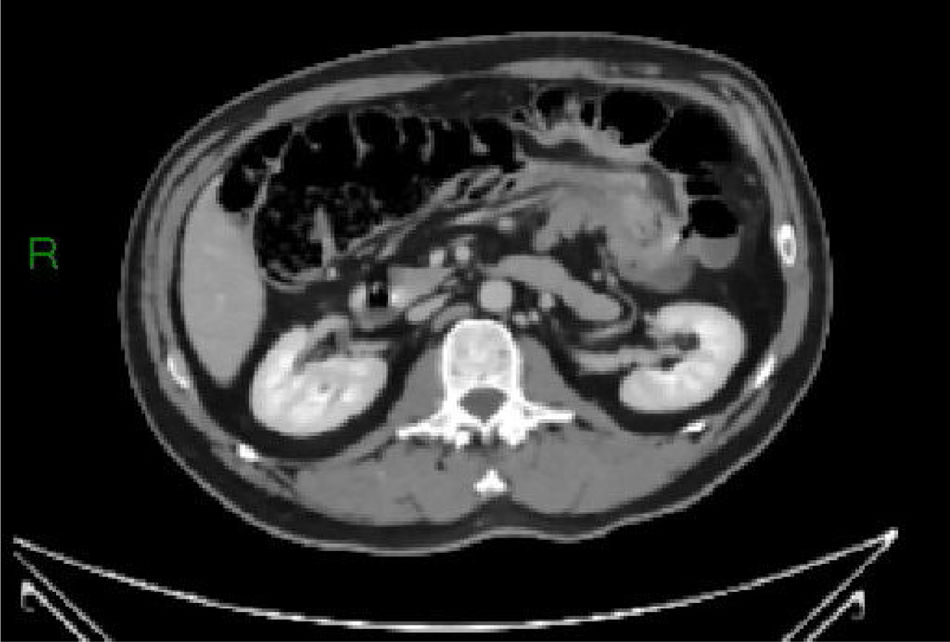
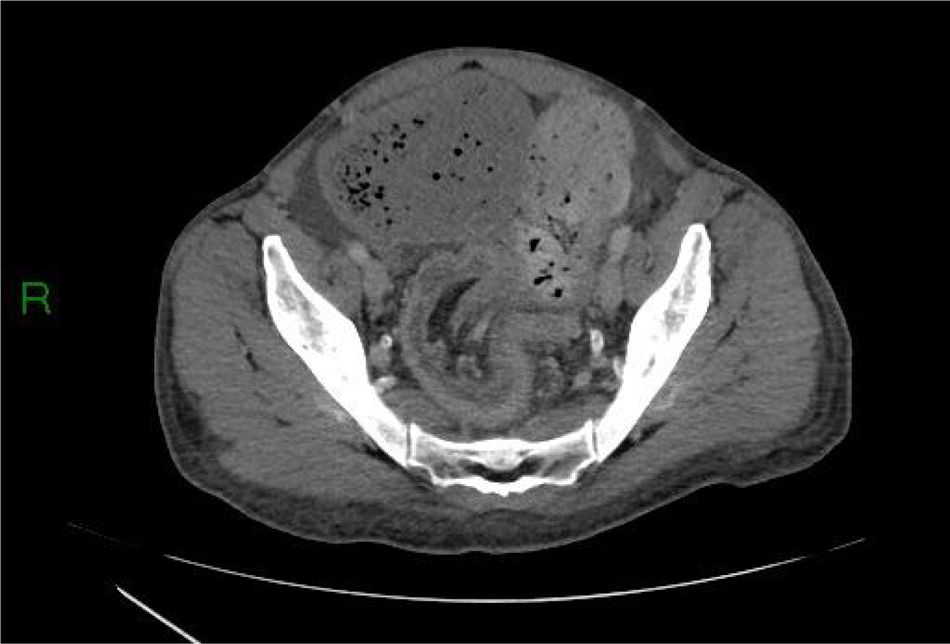
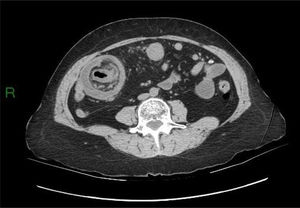
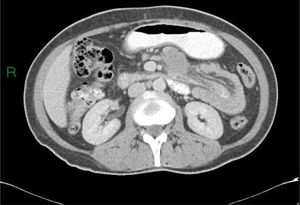
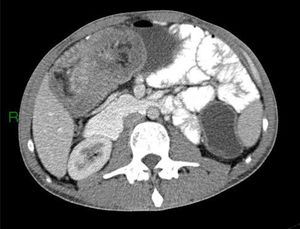
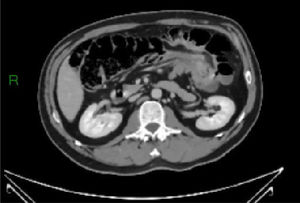
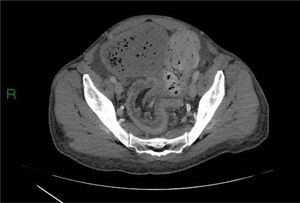
Different types of intussusceptions were found: 14 patients had enteroenteric intussusception, 4 had ileocecal intussusception, 4 had ileocolonic intussusception, 5 had colocolonic intussusception, and one had colorectal intussusception (Figs. 1–5).
Analysis of the median symptom duration by intussusception subtype produced the following results: 14 days (range, 1-365 days) for the enteroenteric type, 92 days (range, 9-210 days) for the ileocecal type, 38 days (range, 2-60 days) for the ileocolonic type, 40 days (range, 14-365 days) for the colocolonic type, and 16 days for the colorectal type. There was no significant difference in symptom duration, when comparing the etiology groups, using the Kruskal-Wallis test (p = 0.183).
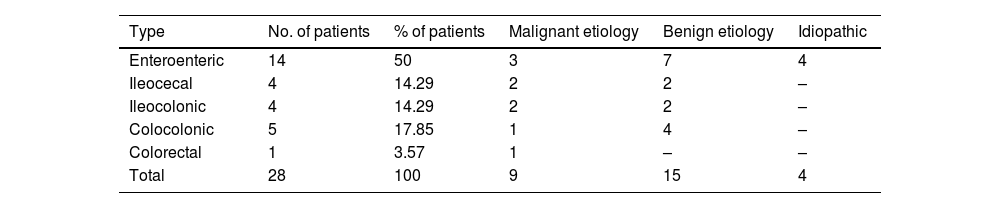
EtiologyIntestinal lesions were identified in 24 cases as lead points, and 4 were idiopathic. Benign lesions were found in 15 patients and malignant lesions in 9 patients (Table 2).
Treatment
Overall, 25 patients underwent surgery. Three patients were treated conservatively, with good results.
Surgery was performed on 11 of the 14 enteroenteric intussusceptions, including 10 small bowel segmental resections with primary anastomosis, and one manual reduction without resection. Three cases were managed without surgery.
Surgical treatment was performed on the 4 patients with ileocecal intussusception, including one small bowel segmental resection with primary anastomosis and 3 right hemicolectomies. Of the latter, one was carried out with primary anastomosis, and the rest required terminal ileostomy due to patient hemodynamic instability.
All the patients with ileocolonic intussusception (n = 4) were treated with right hemicolectomy. Regarding the patients with colocolonic intussusception, surgery was performed in all 5 cases, including 3 right hemicolectomies, one left hemicolectomy, and one transverse colon segmental resection. One patient with colorectal intussusception required manual reduction and loop colostomy due to malignancy (Table 3).
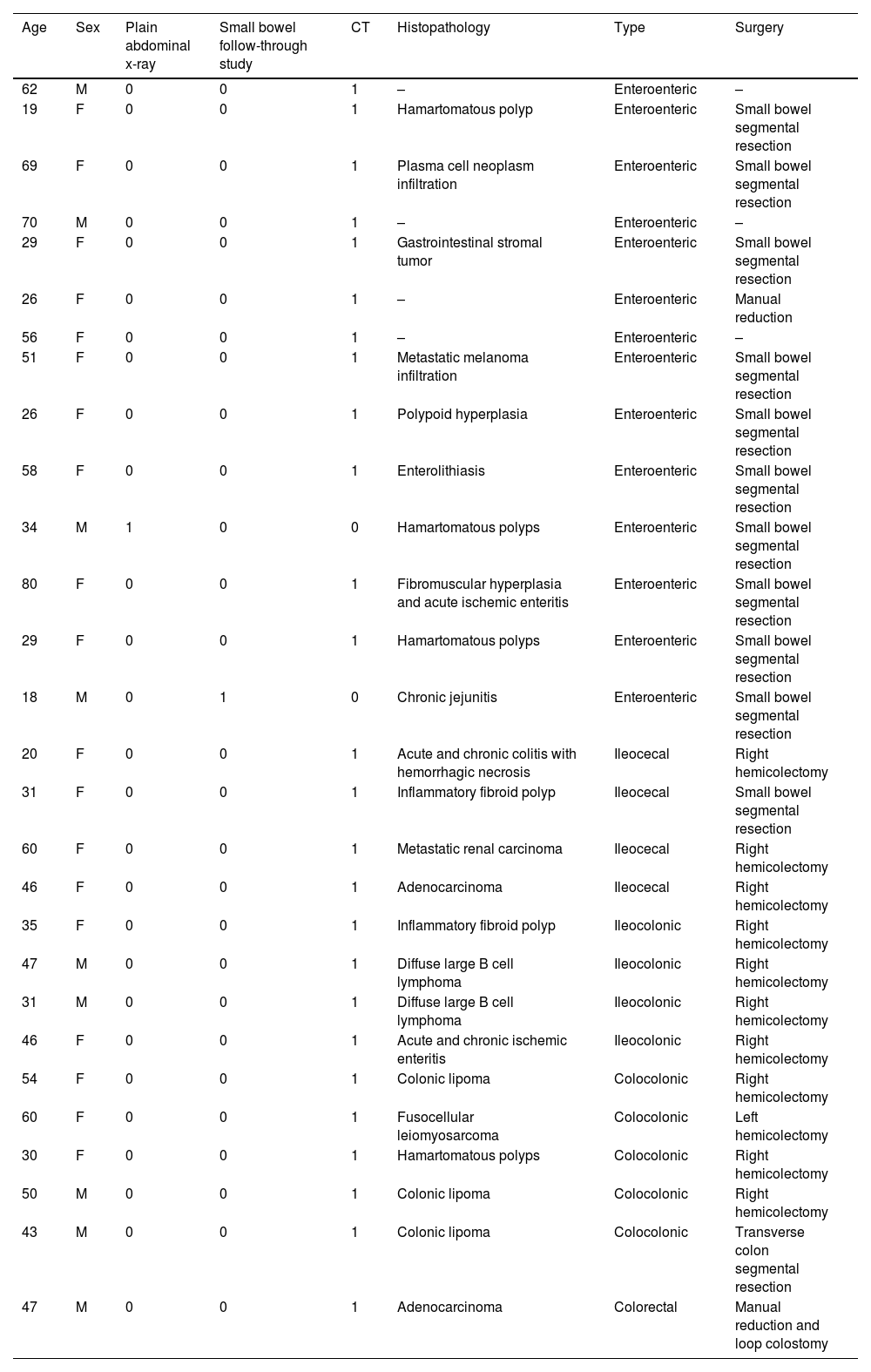
Preoperative diagnosis, etiology, and treatment of 27 cases of adult intussusception.
| Age | Sex | Plain abdominal x-ray | Small bowel follow-through study | CT | Histopathology | Type | Surgery |
|---|---|---|---|---|---|---|---|
| 62 | M | 0 | 0 | 1 | – | Enteroenteric | – |
| 19 | F | 0 | 0 | 1 | Hamartomatous polyp | Enteroenteric | Small bowel segmental resection |
| 69 | F | 0 | 0 | 1 | Plasma cell neoplasm infiltration | Enteroenteric | Small bowel segmental resection |
| 70 | M | 0 | 0 | 1 | – | Enteroenteric | – |
| 29 | F | 0 | 0 | 1 | Gastrointestinal stromal tumor | Enteroenteric | Small bowel segmental resection |
| 26 | F | 0 | 0 | 1 | – | Enteroenteric | Manual reduction |
| 56 | F | 0 | 0 | 1 | – | Enteroenteric | – |
| 51 | F | 0 | 0 | 1 | Metastatic melanoma infiltration | Enteroenteric | Small bowel segmental resection |
| 26 | F | 0 | 0 | 1 | Polypoid hyperplasia | Enteroenteric | Small bowel segmental resection |
| 58 | F | 0 | 0 | 1 | Enterolithiasis | Enteroenteric | Small bowel segmental resection |
| 34 | M | 1 | 0 | 0 | Hamartomatous polyps | Enteroenteric | Small bowel segmental resection |
| 80 | F | 0 | 0 | 1 | Fibromuscular hyperplasia and acute ischemic enteritis | Enteroenteric | Small bowel segmental resection |
| 29 | F | 0 | 0 | 1 | Hamartomatous polyps | Enteroenteric | Small bowel segmental resection |
| 18 | M | 0 | 1 | 0 | Chronic jejunitis | Enteroenteric | Small bowel segmental resection |
| 20 | F | 0 | 0 | 1 | Acute and chronic colitis with hemorrhagic necrosis | Ileocecal | Right hemicolectomy |
| 31 | F | 0 | 0 | 1 | Inflammatory fibroid polyp | Ileocecal | Small bowel segmental resection |
| 60 | F | 0 | 0 | 1 | Metastatic renal carcinoma | Ileocecal | Right hemicolectomy |
| 46 | F | 0 | 0 | 1 | Adenocarcinoma | Ileocecal | Right hemicolectomy |
| 35 | F | 0 | 0 | 1 | Inflammatory fibroid polyp | Ileocolonic | Right hemicolectomy |
| 47 | M | 0 | 0 | 1 | Diffuse large B cell lymphoma | Ileocolonic | Right hemicolectomy |
| 31 | M | 0 | 0 | 1 | Diffuse large B cell lymphoma | Ileocolonic | Right hemicolectomy |
| 46 | F | 0 | 0 | 1 | Acute and chronic ischemic enteritis | Ileocolonic | Right hemicolectomy |
| 54 | F | 0 | 0 | 1 | Colonic lipoma | Colocolonic | Right hemicolectomy |
| 60 | F | 0 | 0 | 1 | Fusocellular leiomyosarcoma | Colocolonic | Left hemicolectomy |
| 30 | F | 0 | 0 | 1 | Hamartomatous polyps | Colocolonic | Right hemicolectomy |
| 50 | M | 0 | 0 | 1 | Colonic lipoma | Colocolonic | Right hemicolectomy |
| 43 | M | 0 | 0 | 1 | Colonic lipoma | Colocolonic | Transverse colon segmental resection |
| 47 | M | 0 | 0 | 1 | Adenocarcinoma | Colorectal | Manual reduction and loop colostomy |
The median overall length of hospital stay was 9 days (range, 2-27 days). The median length of stay by intussusception subtype was: 15 days (range, 2-27 days) for the enteroenteric type, 6 days (range, 4-19 days) for the ileocecal type, 8 days (range, 4-27 days) for the ileocolonic type, 10 days (range, 6-19 days) for the colocolonic type, and 9 days for the colorectal type. There was no significant difference in total length of stay, when comparing the etiology groups, using the Kruskal-Wallis test (p = 0.810). A subdivision of the length of hospital stay into ≥ 7 days and < 7 days was performed, and a possible association between length of stay and etiologic subtype of intussusception was evaluated using the Fisher’s exact test. However, no statistically significant association was found between those two variables (p = 0.232).
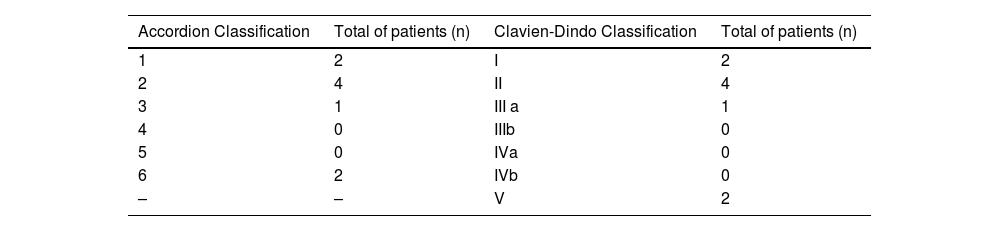
Morbidity was documented in 9 patients, 8 of whom received surgical treatment (Tables 4 and 5). Two of our patients passed away within 30 days of surgery. One of those patients had a history of myelodysplastic syndrome and the other had poorly controlled human immunodeficiency virus infection.
As part of the in-hospital follow-up of the 3 patients with idiopathic intussusception that did not receive surgical management, in addition to the clinical resolution, one of them underwent a push enteroscopy, in which intussusception was resolved and no lesion acting as a lead point was found. The remaining 2 patients had an abdominal CT scan, showing intussusception remission. None of them required hospitalization due to a new intussusception event.
Discussion and conclusionsAdult intussusception accounts for 5% of all cases of intussusceptions and only 1-5% of intestinal obstruction cases.2 In contrast to the pediatric population, nearly 90% of the cases of adult intussusceptions are secondary to a pathologic condition that functions as a lead point,7 and 8-20% are classified as primary or idiopathic.2,8,9 There is a 65% risk of associated malignancy in adult intussusception cases,10 signifying that almost 70-90% of those cases could require surgical resection.9
Malignancy accounts for 30% of the cases of small bowel intussusception9 and up to 66% of the cases of colonic intussusceptions.7 We retrospectively reviewed 20 years of data from adult patients with intussusception and found that 32.14% of the cases (n = 9) were related to malignancy, 53.57% (n = 15) had benign etiology, and 14.29% (n = 4) were idiopathic. On the other hand, in a pediatric case series, approximately 90% of the cases were idiopathic.11
Similar to the results of Zubaidi et al.1 and Wang et al.,12 enteroenteric intussusception was the most common type in our series, whereas the colocolonic and colorectal types were less common.
Clinical presentation is nonspecific, with variable symptom duration. In a study by Honjo et al.4 that included 44 adult patients with intussusception, abdominal pain was reported in 54.5%, vomiting in 10%, abdominal distension in 4%, gastrointestinal bleeding in 6%, and diarrhea in 8%. Our results showed a different distribution of those symptoms, with 96.42%, 71.42%, 35.71%, 28.57%, and 32.14%, respectively.
In a retrospective review of 41 patients with intussusceptions, Wang et al.12 classified clinical presentation, according to symptom duration, as follows: acute symptoms: < 4 days; subacute symptoms: 4-14 days; and chronic symptoms: > 14 days. In their series, 24.4% of the patients had acute symptoms, 24.4% had subacute symptoms, and 51.2% had chronic symptoms. In our series, most of the patients presented with chronic symptoms (64.28%), followed by acute (17.86%) and subacute (17.86%) symptoms.
Abdominal CT has been reported as the most useful imaging technique for diagnosing intussusception,13 with 58 to 73% diagnostic accuracy.2,14 In our study, CT was used in 92.85% of the cases, with 100% diagnostic accuracy. A small bowel follow-through study was used in one case, by which, preoperatively, the patient was correctly diagnosed. In a study by Barussaud et al.,14 barium enema was reported to have 73% diagnostic accuracy and upper gastrointestinal series 33% sensitivity. Other studies reported 54% diagnostic accuracy for barium enema and 21-45% diagnostic accuracy for upper gastrointestinal series.2,15
Surgical resection remains the recommended treatment in most cases, to address the pathologic lead point, which can be malignant. Surgical or endoscopic reduction of the intussusception has the risk of increased recurrence, and malignancy cannot be ruled out because a specimen is not retrieved for pathologic examination.
In our series, there were 5 cases of Peutz-Jeghers syndrome. Four of them were treated with segmental resection of the small bowel with primary anastomosis, and the remaining case was treated with a right hemicolectomy and ileotransverse anastomosis due to colocolonic intussusception. Given that intussusception is frequent among patients with Peutz-Jeghers syndrome, intussusception reduction, followed by enterotomy and polypectomy, can be recommended as a treatment option, to preserve intestinal length. The endoscopic “clean sweep” technique, through which the intestinal tract is examined with an endoscope and polyps are removed, may be used as a treatment option, to reduce further risk of intussusception.16
Our study limitations include its retrospective design, the limited number of patients due to the infrequent nature of adult intussusception, and the fact that it was carried out at a single center. However, the study provides information on the etiologic causes, clinical presentation, and possible treatment outcomes of the condition.
The results of our study do not necessarily represent the population of other localities, so they should be interpreted with caution.
In conclusion, intussusception is a rare condition in the adult population. Diagnosis is challenging, given that the signs and symptoms are nonspecific, and so it must be contemplated in the differential diagnosis. Today, noninvasive imaging studies are available for providing a timely diagnosis, and abdominal CT is the most useful study for adequate characterization.
Surgical resection should be considered for the definitive treatment, and management should be individualized, according to patient comorbidities, clinical presentation, and the risk of malignancy.
Financial disclosureThe authors received no financial support for the research, authorship, and/or publication of this article.
Author contributionsF.E. Alvarez-Bautista, P. Moctezuma-Velázquez, and A.S. Pimienta-Ibarra designed this work, collected and interpreted the data, and drafted the manuscript. O. Vergara-Fernández and N. Salgado-Nesme interpreted data, critically revised the manuscript, and performed overall supervision. All authors contributed to the final approval of the manuscript.
Conflict of interestThe authors declare there are no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Please cite this article as: Alvarez-Bautista FE, Moctezuma-Velázquez P, Pimienta-Ibarra AS, Vergara-Fernández O, Salgado-Nesme N. Intususcepción en adultos: todavía un reto diagnóstico para el cirujano. Rev Gastroenterol Méx. 2023;88:315–321.