Gastroesophageal junction adenocarcinoma (GEJA) accounts for 0.05% of pediatric malignant gastrointestinal tumors.1 The common age at presentation is above 50 years, and so its appearance in children and adolescents is extremely rare.2
There are very few case reports in pediatric patients,1 and they are listed in Table 1. Staging and treatment in that population is based on those established for adults. Prognosis is usually poor, given that those tumors in children are often poorly differentiated, and because the disease is largely unsuspected, it is diagnosed in advanced stages with metastasis, resulting in a mortality rate close to 100%. Thus, cases of dysphagia in children should potentially be studied.1,3
Due to the low presentation frequency of the tumor, its causes are not yet well defined.4 They have been related to certain risk factors in adults, such as smoking, alcohol use, fatty food and red meat consumption, A blood type, as well as Epstein-Barr virus infection and Helicobacter pylori infection, with the vacAs1-, vacAm1-, cagA-positive genotypes; those infections are potentiated in patients that are carriers of the cytokine gene polymorphisms, such as IL-1B-511*T/*T or IL-1B-511*T/*C. Cases are most likely de novo in children but germline mutations in E-cadherin, with an autosomal dominant inheritance pattern, must not be ruled out, which if present, can be a treatment target.2
Dysphagia is the most prevalent symptom, followed by weight loss, anemia, dehydration, nausea, epigastric or retrosternal pain, regurgitation, and hematemesis.4
In 1996, Siewert et al. proposed a classification based on the definition of GEJA, which is a neoformation that grows within 5cm of the cardia, in a distal or proximal direction, and that is divided into 3 subtypes:
- •
Type I: adenocarcinoma of the distal esophagus, extending 1 to 5cm above the junction.
- •
Type II: adenocarcinoma of the cardia; “junctional carcinoma”, extending 1cm above and 2cm below the junction.
- •
Type III: subcardial gastric carcinoma, extending 2 to 5cm below the junction.5
In the past, standard treatment was open surgical resection with negative margins. Currently, tumors that only affect the mucosa (T1a) can be treated through endoscopic resection.6 In patients with locally advanced disease (T3 or T4), perioperative chemotherapy and radiotherapy significantly improve survival.7 Treatment with epirubicin, cisplatin, and 5-fluorouracil have increased survival by 36%, compared with the 23% in patients treated only through surgery.8
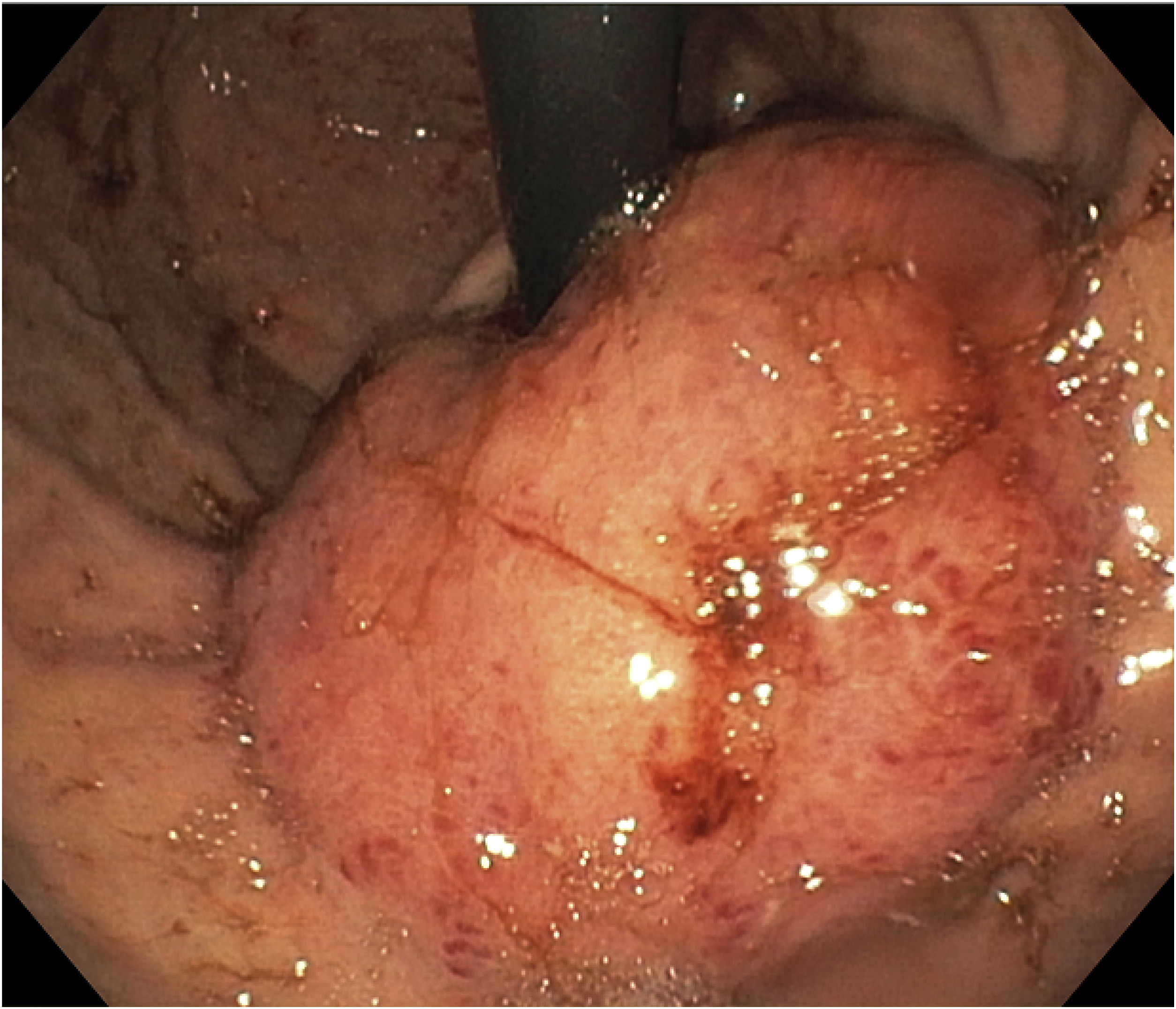
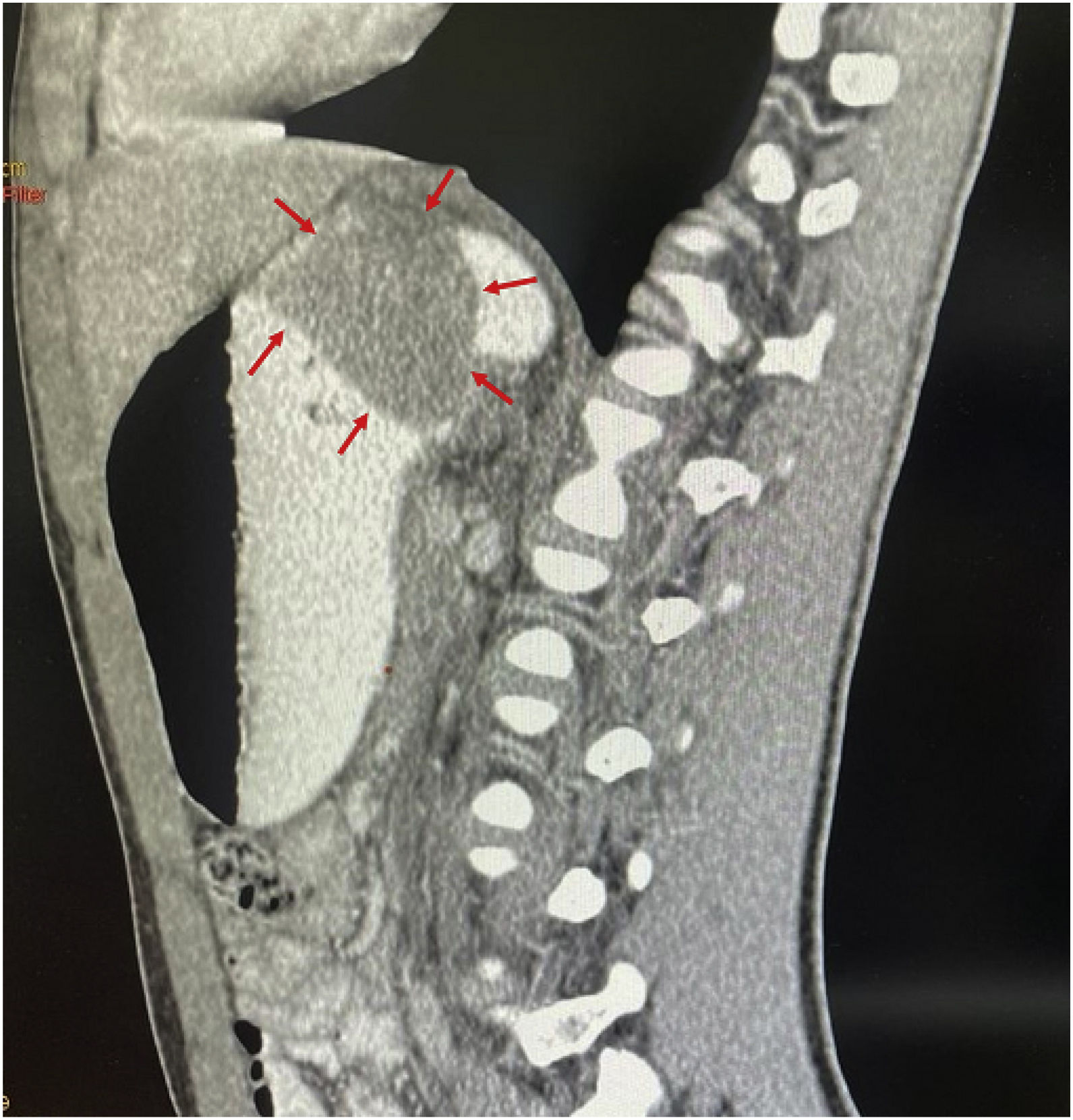
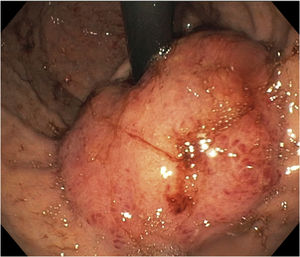
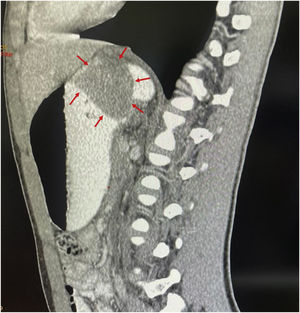
A 15-year-old boy was seen at the outpatient service of the Hospital Central del Estado de Chihuahua. He had a medical history of 4 months of progressive dysphagia, anemia syndrome, and weight loss. He was hospitalized, with Hb of 5.5g/dl, MCV of 74fl, MCH of 24pg, and platelets of 500×103/ul. He underwent transfusion with two units of red blood cells and then had an upper endoscopic examination. Retroflexion during the upper endoscopy revealed a tumor in the cardia, 6cm from the mucosa. Its aspect was adenomatous and friable, and it bled during the insufflation. The tumor extended into the lesser curvature and the inferior third of the esophagus, partially obstructing the lumen (Fig. 1), and corresponded to a type II GEJA, according to Siewert. A tomography scan of the chest and abdomen identified a 5.7×2.6cm infiltrative gastric tumor, with perigastric lymph node invasion, that had clinical staging (cTNM) of T3, N2, M0 (Fig. 2). The histopathologic findings through immunohistochemistry were a moderately differentiated adenocarcinoma, with invasion of the stroma, no microsatellite instability, integral DNA repair protein expression, and null p53 expression. The patient underwent preoperative chemotherapy administration with fluorouracil, leucovorin, oxaliplatin, and docetaxel (FLOT). Four months ago, he underwent total gastrectomy, extended with transhiatal resection of the esophagus, and retromesocolic Roux-en-Y reconstruction. After the surgery, the patient was given 4 more chemotherapy cycles with the FLOT regimen and currently is undergoing radiotherapy, with good response.
With our report of this case and the review of the literature, our aim was to favor the general understanding of these rare pediatric tumors and promote their diagnostic suspicion in a patient that presents with a history of dysphagia, weight loss, and anemia.
Ethical considerationsThe authors declare that this article contains no personal information that can identify the patient. All protocols according to the ethics committee of the Hospital Central del Estado were followed, with respect to preserving patient privacy. A written statement of informed consent was not requested, given that no personal information was used that could identify the patient and the photographs showed no personal data. Even so, the patient and mother gave their verbal consent for the publication of this case.
Financial disclosureNo financial support was received in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Amaya Villagrán G, Loya Lazcano KM, Baeza Zapata AA. Presentación atípica en la adolescencia de un adenocarcinoma de la unión esofagogástrica. Rev Gastroenterol Méx. 2023;88:299–301.