Several groups have reported associations of primary biliary cholangitis with other autoimmune entities, particularly Sjögren's syndrome and hypothyroidism. Its prevalence and characteristics in Mexican patients is unknown.
AimTo determine the frequency and characteristics of autoimmune diseases in a Mexican cohort of patients with primary biliary cholangitis.
Materials and methodsThe medical records of patients that presented with primary biliary cholangitis within the time frame of 2005 and 2012 were reviewed and assessed for other autoimmune diseases.
ResultsSeventy-eight patients, 75 women and 3 men, were included. Their mean age was 55.8 years. Seventy-three cases had positive antimitochondrial antibodies (94.8%) and disease was confirmed in 5 through liver biopsy. Five patients (8%) had anti-smooth muscle antibodies and 55/78 (70.5%) had antinuclear antibodies by indirect immunofluorescence. Forty-nine patients (62.8%) were positive for an autoimmune disease other than primary biliary cholangitis. Among those, 20 patients had one associated disease, 14 had 2, and 15 patients had 3 concomitant diseases. They included: Sjögren's syndrome in 23/78 patients (29.5%), dysthyroidism in 21/78 cases (26.9%), Raynaud syndrome in 11/78 (14.1%), CREST syndrome in 9/78 patients (11.4%), rheumatoid arthritis in 6/78 patients (7.7%), vitiligo in 5/78 (6.4%), scleroderma in 4/78 patients (5.1%), and other diseases in 8 patients. In 12/78 patients (15.4%), there was a documented family background of autoimmune disease.
ConclusionsThe presence of autoimmune associations in our cohort was frequent, and similar in characteristics to the information reported by other groups. The clinical implications of those findings remain to be determined.
La colangitis biliar primaria es una enfermedad hepática colestásica crónica de origen autoinmune. Diferentes grupos han reportado asociaciones de esta enfermedad con otros padecimientos autoinmunes, particularmente el síndrome de Sjögren y el hipotiroidismo. Se desconoce la prevalencia y las características en pacientes mexicanos.
ObjetivosEl objetivo del presente trabajo fue determinar la frecuencia y las características de padecimientos autoinmunes en una cohorte mexicana de pacientes con colangitis biliar primaria.
Material y métodosSe realizó una revisión de los expedientes de pacientes con colangitis biliar primaria entre 2005 y 2012 evaluando por otras enfermedades autoinmunes.
ResultadosSe incluyeron 78 pacientes, 75 mujeres y 3 hombres, con una edad promedio de 55.8 años. Setenta y tres de ellos presentaron anticuerpos antimitocondriales positivos (94.8%) y 5 fueron confirmados mediante biopsia hepática. Cinco (8%) de los pacientes presentaron anticuerpos antimúsculo liso positivos y 55/78 (70.5%) presentaron anticuerpos antinucleares positivos por inmunofluorescencia indirecta. Cuarenta y nueve de los 78 (62.8%) pacientes presentaron otra enfermedad autoinmune además de la colangitis biliar primaria. De estos, 20 tuvieron solo una enfermedad asociada, 14 mostraron 2 enfermedades asociadas y 15, 3 enfermedades asociadas. Por orden de frecuencia descendente se encontraron: síndrome de Sjögren en 23/78 (29.5%) pacientes, distiroidismo en 21/78 (26.9%), fenómeno de Raynaud en 11/78 (14.1%), CREST en 9/78 (11.4%), artritis reumatoide en 6/78 (7.7%), vitiligo en 5/78 (6.4%), esclerodermia en 4/78 (5.1%) y otras en 8 pacientes. En 12/78 (15.4%) existió antecedente documentado de enfermedades autoinmunes en la familia.
ConclusionesLa presencia de asociaciones autoinmunes en nuestra cohorte fue frecuente y con características similares a lo reportado por otros grupos. Desconocemos las implicaciones clínicas de estos hallazgos.
Primary biliary cholangitis (PBC) is a slowly progressive hepatic cholestatic disease that predominates in females and may culminate in cirrhosis and its complications. It is considered a prototype immune disease due to the presence of the highly specific antibodies, antimitochondrial antibodies, and the autoreactive T cells against the biliary epithelium. Its association with other autoimmune diseases, mainly with Sjögren's syndrome (SS) and autoimmune dysthyroidism, has been described. Familial association of autoimmune disease has also been described. The aim of this paper was to describe the frequency and characteristics of the autoimmune diseases associated with PBC in a cohort of Mexican patients.
Materials and methodsA descriptive, observational, cross-sectional, and retrospective study was conducted on all patients diagnosed with PBC within the time frame of January 2005 and October 2012. Only patients with complete medical charts at the Centro Médico ISSEMyM in Metepec, Estado de México, were included in the study. That hospital center belongs to the Instituto de Seguridad Social del Estado de México y Municipios. PBC diagnosis was based on the currently accepted criteria, in patients with 2 or more of the following: a cholestatic pattern (once other diseases were excluded) with elevated alkaline phosphatase, the presence of antimitochondrial antibodies detected by indirect immunofluorescence (Hep2 cells), and compatible histopathologic findings (chronic periportal inflammation with lymphocytes and plasma cells, and bile duct damage with ductular proliferation and/or ductopenia, granulomas, with/without fibrosis).1–3 Patients with other symptoms were assessed by the rheumatology department. The following were the criteria employed to diagnose the autoimmune associations:
- -
SS was diagnosed if the criteria of the American-European Consensus Group 20024 were met.
- -
Thyroid pathology (dysthyroidism) was established through the detection of abnormal TSH, T3 and/or T4 values, as well as positive anti-thyroglobulin antibodies, anti-peroxidase antibodies and/or antibodies against TSH receptors, obtained if considered necessary by the endocrinologist.
- -
Raynaud syndrome was clinically established in patients with the classic 3-phase triad associated with PBC.5,6
- -
Rheumatoid arthritis was diagnosed according to the 1987 criteria of the American College of Rheumatology and those established in 2010 by the American College of Rheumatology and the European League against Rheumatism.7,8
- -
Systemic sclerosis and calcinosis, Raynaud syndrome, esophageal dysmotility, sclerodactyly, and telangiectasia (CREST) syndrome were diagnosed according to the criteria established by the American College of Rheumatology in 1980.9
- -
Other diagnoses were obtained directly from the Rheumatology Department notes.
Patients with other causes of hepatic disease were excluded, as well as those with hepatic overlap syndromes and patients with incomplete charts. The statistical analysis was carried out using measures of central tendency.
Our study was approved by the Research Ethics Committee of the Instituto de Seguridad Social del Estado de México y Municipios.
ResultsOne hundred and fourteen medical charts were identified, 36 of which were excluded because they were incomplete, or the patients had been diagnosed with an overlap syndrome. A total of 78 patients, 75 women (96.2%) and 3 men, were included in the study. The mean patient age at diagnosis was 55.8 years, with a range of 32 to 78 years. Non-autoimmune associated diseases were documented in 47 individuals (60.25%). In descending order, they included: type 2 diabetes mellitus (n = 20), systemic arterial hypertension (n = 16), gastroesophageal diseases (n = 8), neoplasms (n = 6), a history of colon cancer (n = 1), a history of breast cancer (n = 1), non-Hodgkin's lymphoma (n = 1), plasmacytoma (n = 1), a history of follicular thyroid cancer (n = 1), and a retroperitoneal tumor (n = 1).
Autoimmunity in the family. Twelve of the 78 cases (15.4%) had a family history of autoimmune disease, including: rheumatoid arthritis in 3 cases, PBC in 2, cirrhosis of undetermined cause in 3, thyroid disease in 2, anti-phospholipid syndrome in one, and type 1 diabetes mellitus with celiac disease in one case.
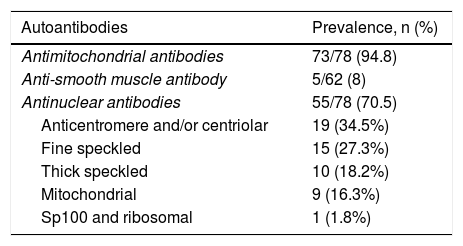
Autoantibodies. Seventy-three patients were positive for antimitochondrial antibodies (94.8%) and the other 5 were diagnosed through liver biopsy (antimitochondrial antibody-negative PBC). In 62 patients, anti-smooth muscle antibodies were determined, and they were positive in 5 (8%) cases. Fifty-nine patients were tested for antinuclear antibodies by indirect immunofluorescence and they were positive in 55 (70.5% of the entire cohort). The most frequently detected patterns were: anticentromere and/or centriolar in 19 (34.5%) patients, fine-speckled in 15 (27.3%), thick-speckled in 10 (18.2%), anti-mitochondrial in 9 (16.3%), anti-Sp100 in one patient, and anti-ribosomal in one case (1.8%). Eighteen (32.7%) patients had more than one pattern (Table 1). At diagnosis, 57 patients (73%) had high serum globulin levels. Different immunoglobulins were determined in 33 patients. Seventeen patients (51.55%) had elevated IgM, 12 (36.4%) cases had increased IgG, and 12 (36.4%) had elevated IgA.
Presence of antibodies in a cohort of Mexican patients diagnosed with primary biliary cholangitis.
| Autoantibodies | Prevalence, n (%) |
|---|---|
| Antimitochondrial antibodies | 73/78 (94.8) |
| Anti-smooth muscle antibody | 5/62 (8) |
| Antinuclear antibodies | 55/78 (70.5) |
| Anticentromere and/or centriolar | 19 (34.5%) |
| Fine speckled | 15 (27.3%) |
| Thick speckled | 10 (18.2%) |
| Mitochondrial | 9 (16.3%) |
| Sp100 and ribosomal | 1 (1.8%) |
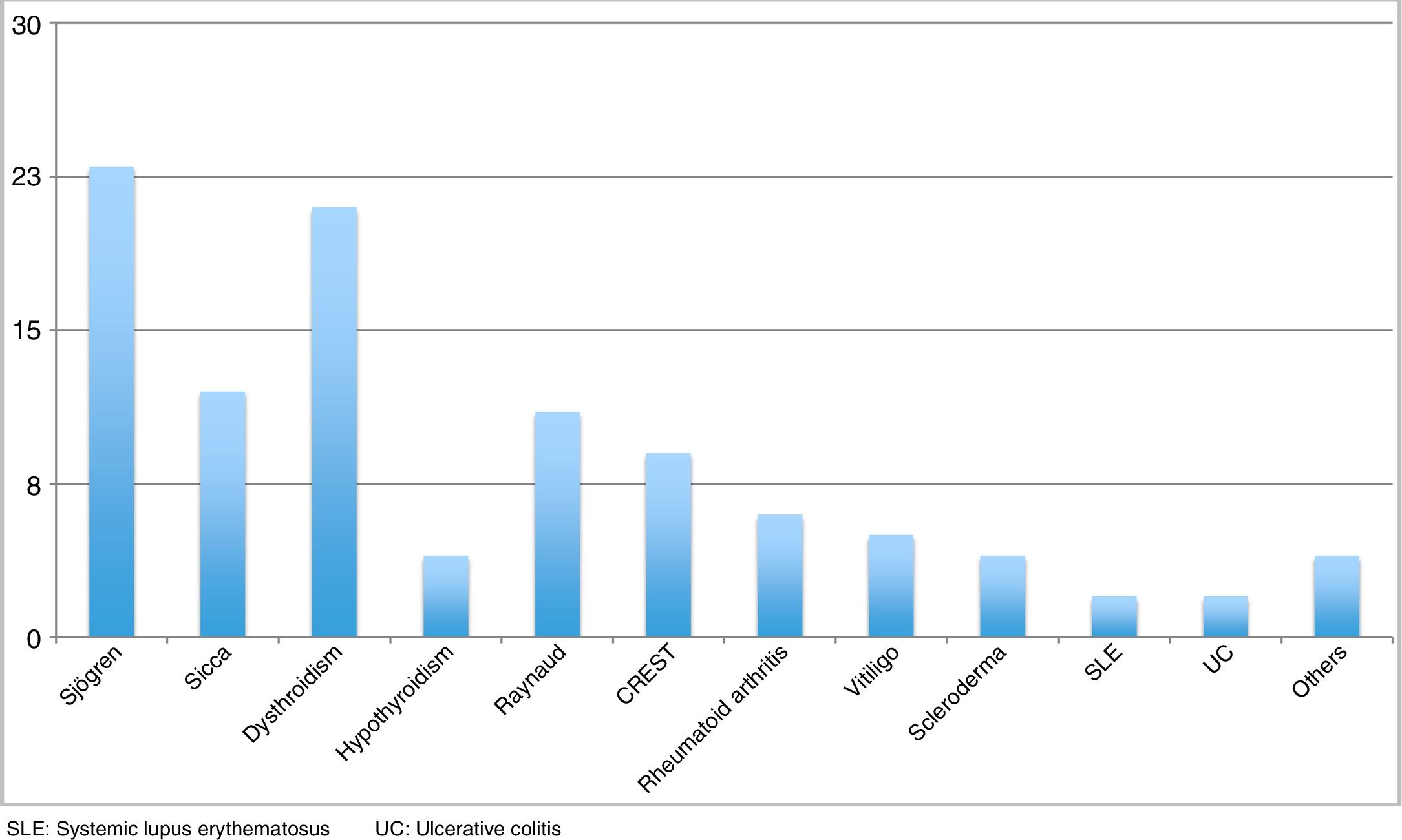
Autoimmune associations. Forty-nine (62.8%) individuals presented with autoimmune associations. Twenty (25.6%) patients had only one associated autoimmune disease, 14 (17.9%) presented with 2, and 15 (19.2%) patients had 3. Figure 1 shows the main associated diseases in descending order by frequency, which are:
- -
SS/SICCA: Twenty-three (23) patients (29.5%) fulfilled the diagnostic criteria for SS, whereas 12 other patients presented with symptoms, but did not meet the criteria (SICCA syndrome).
- -
Autoimmune dysthyroidism: A thyroid profile was obtained in 44 of the 78 patients. Twenty-one (26.9%) had an abnormal thyroid profile with elevated TSH, 20 had low T4, and 18 patients had low T3 values. Antithyroid antibody testing (antithyroglobulin and antiperoxidase) was carried out in only 10 cases and 4 of them were positive for those antibodies (9%). A patient with previously diagnosed hypothyroidism, receiving substitution therapy, had a normal thyroid profile and was also included in the study.
- -
Raynaud syndrome in 11 patients (14.1%).
- -
CREST in 9 patients (11.4%).
- -
Rheumatoid arthritis in 6 patients (7.7%).
- -
Vitiligo in 5 patients (6.4%).
- -
Scleroderma in 4 patients (5.1%).
- -
Systemic lupus erythematosus in 2 patients (2.5%).
- -
Ulcerative colitis in 2 patients (2.5%).
- -
Anti-phospholipid syndrome, lymphocytic colitis, celiac disease, and polyglandular autoimmune syndrome were diagnosed in one patient, each (1.27%).
In our cohort of patients with PBC, the predominance of adult women with a high prevalence of antimitochondrial antibodies was similar to the information reported in the international literature.10 Even though it was not the primary aim of our study, it is important to highlight the high frequency of patients with a positive autoimmune history and/or the presence of associated neoplasms in 7.6% (6/78) of the cases. Such an elevated incidence was previously described by Liang et al. in a meta-analysis that included 16,300 patients with PBC.11 Another relevant finding in our cohort, was the high frequency of antinuclear antibodies (70.5%), similar to that described in the literature by Muratori et al. (50-72%).12 We are unaware of their possible clinical implications.
In terms of associated autoimmune diseases in patients with a diagnosis of PBC, that phenomenon was described some decades ago.13–17 We found that the frequency of at least one autoimmune disease associated with PBC in our cohort, was 62.8% (49/78), a high percentage when compared with previous reports over the past few decades, but similar to that reported by Floreani in 2015.18 His group reported a prevalence of extrahepatic autoimmune disease of 61.2%. The most frequent autoimmune manifestations were SS, autoimmune hypothyroidism, and Raynaud syndrome, in 56, 29.4 and 23.6% of cases, respectively. Watt and contributors19 described a 53% prevalence of autoimmune association in their cohort of 160 patients in the north of England. The most frequently associated entities were SS (25%), thyroid disease (23%), and rheumatoid arthritis (13%). The cohort of 322 Chinese patients in the study by Wang et al.,20 revealed a prevalence of associated autoimmune disease of 46.6%, the most frequent of which was SS (36%), and unlike reports in Western groups, it was followed in frequency by systemic lupus erythematosus (3.7%) and polymyositis (3.1%). In a published analysis in 2005 by Gershwin et al.21 on 1,032 patients from the United States, he described autoimmune comorbidities in 32% of cases. The most frequent were Raynaud syndrome (12%), SS (10%), and rheumatoid arthritis (10%).
Finally, in a 2012 study on 111 Greek patients from the Island of Crete, Mantaka et al.22 reported a prevalence of at least one associated autoimmune disease in 36.9% of the patients. The most frequent were Hashimoto's disease (18%), Raynaud's phenomenon (6.3%), and SS (5.4%). It should be mentioned that their cohort resided on the island, so the characteristics of that relatively captive population could be different from other cohorts, due to possible genetic and environmental biases. SS was also the most frequent association in our group, present in 23 patients (29.5%), and 12 other patients had SICCA syndrome. In a cohort from Northern England, Watt et al.19 described 33 cases of SICCA, in addition to 40 cases of SS. Whether that syndrome, associated with PBC, is an incomplete form of SS or simply requires more time to manifest completely, remains unknown. That association has been studied for several decades now, and several authors have stated that it is part of a systemic disorder with a common pathophysiologic basis, given that PBC and SS share common clinical characteristics, such as a predominance in women, development on average in the fifth decade of life, and the involvement of epithelial cells.14–16,23 SS is characterized by the destruction of the salivary epithelial tissue, lacrimal glands, and other exocrine glands, leading to the absence of secretions, or a minimum amount of them. In 1979 Strand and Talal observed and documented the condition of different exocrine glands, coining the term “autoimmune exocrinopathy”,24 which was replaced by “autoimmune epithelitis” in 1994, clearly indicating immune-mediated injury.25 In addition, Granito et al.,26 reported the coexistence of SSa/Ro antibodies as a marker of advanced histologic disease.
Some of the theories behind those facts stem from the concept that serum antibodies (antimitochondrial antibodies, anti-Ro for PBC, and anti-La for SS) and their specific receptors are present in all nucleated cells.27 There is thought to be an environmental trigger for both conditions (infections or xenobiotics) that induces apoptosis of epithelial cells at the biliary and lacrimal levels. Additionally, those cells contribute to the autoimmune process by expressing cytokines, adhesion molecules, and the type II major histocompatibility complex.28 Since there is no specific treatment for either of the 2 diseases, further research of their underlying immunologic and genetic mechanisms is essential to the development of a specific treatment, early detection methods, and perhaps to the possibility of modifying the natural history of both pathologies.
Autoimmune dysthyroidism is the second entity most frequently associated with PBC. Several groups have described the concomitant presence of Hashimoto's thyroiditis, and less frequently, Graves’ disease.18,19 The approximate frequency reported in the literature ranges between 12 and 29%.9,10,18,22,28,29 In our group, the second most frequent association was an abnormal thyroid profile in 26.9% of the cases. Unfortunately, only 10 individuals were tested for antithyroid antibodies, 4 of whom were positive, representing 9% of the population. That value would most likely have been higher, had antibodies been determined in all patients with an abnormal thyroid profile and PBC.
Raynaud syndrome was the third most frequent extrahepatic autoimmune finding in our population, at 14.1%, which was very similar to the frequency range reported by Floreani and Mantaka.18,22 The association between systemic lupus erythematosus and PBC (2.5%) was similar to that reported by Gershwin et al. in a United States population (3%).21 Rheumatoid arthritis was present in 7.7% of our cohort. The literature has reported a frequency varying from 1.8 to 10%. The frequency of associated scleroderma in the literature is variable.18 The highest, 9.9%, was reported by Floreani et al. In our study, 4 patients (5.1%) presented with scleroderma, whereas the CREST variant was more frequent, presenting in 9 cases (11.4%).
Each of the following diseases was found in one patient per pathology: celiac disease, anti-phospholipid syndrome, lymphocytic colitis, and autoimmune polyglandular syndrome. The literature describes less frequent associations of those diseases,18,28 although Volta et al. reported celiac disease in 4% (7/173) of the PBC patients in their cohort.30 Our cohort did not include any cases of poly/dermatomyositis, unlike those reported by the Asian group cited above. However, we documented 5 patients (6.4%) with vitiligo, a disease that has rarely been described in association with PBC.
The high frequency of autoimmune associations has triggered the search for a genetic basis that may play a role in the pathophysiology of PBC, possibly enabling the early identification of patients with risk factors and leading to their early detection, as well as identifying family patterns, resulting in the description of specific mutations.31 To date, however, there is little conclusive evidence that could tentatively answer those questions. Despite those difficulties, it is clear that PBC has a genetic component, so interest in the study of family members and of cases associated with other autoimmune diseases has surged and will hopefully foster the deciphering of genetic abnormalities that are possibly shared. A review of the immunogenetics of PBC has recently proposed that certain variants described in the Genome Wide Association Studies are under scrutiny and appear to be common to different autoimmune diseases.32
Even though it was not the primary aim of the present study, we documented a high frequency of autoimmune comorbidities in first-degree relatives, a phenomenon described by other authors in similar percentages (15%), which undoubtedly supports the genetic basis of PBC.
Our study has the limitations of being a retrospective study, as well as of having a captive population from a tertiary care hospital with a high number of rheumatology referrals. Therefore, the prevalence of autoantibodies and other diseases may be greater than in other PBC cohorts. Prospective studies are needed to evaluate the relationship between the present study results and the progression, complications, and decompensation of PBC. Despite its limitations, we believe our study provides the soundest evidence of associations of autoimmune diseases with PBC that has been reported in Mexico to date.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureNo financial support was received in relation to this study/article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: González-Huezo MS, Delgado-Ayala LY, Osorio-Núñez AL, Meléndez-Mercado C. Asociaciones autoinmunes en una cohorte mexicana con colangitis biliar primaria. Revista de Gastroenterología de México. 2019;84:130–135.