Abdominal pain in immunocompromised patients is a diagnostic and therapeutic challenge for clinicians because it presents as a nonspecific manifestation due to the inability of the patient to mount an adequate immune response.
Immunocompromised patients are those that have chronic diseases managed through immunomodulators and that suffer from an alteration in the immune response that is innate or secondary to some other pathology. That group of patients includes persons that are advanced in age, that have diabetes mellitus, HIV infection, or neoplasia. It also includes transplanted patients and those that take medications that modify the immune response, such as steroids, anti-TNF alpha, methotrexate, cyclosporine, and tacrolimus, among others.1 Myelosuppression is a major systemic toxicity generally associated with chemotherapy treatments. It considerably increases morbidity and mortality, as well as delays in oncologic treatment, thus altering overall survival in those patients.2
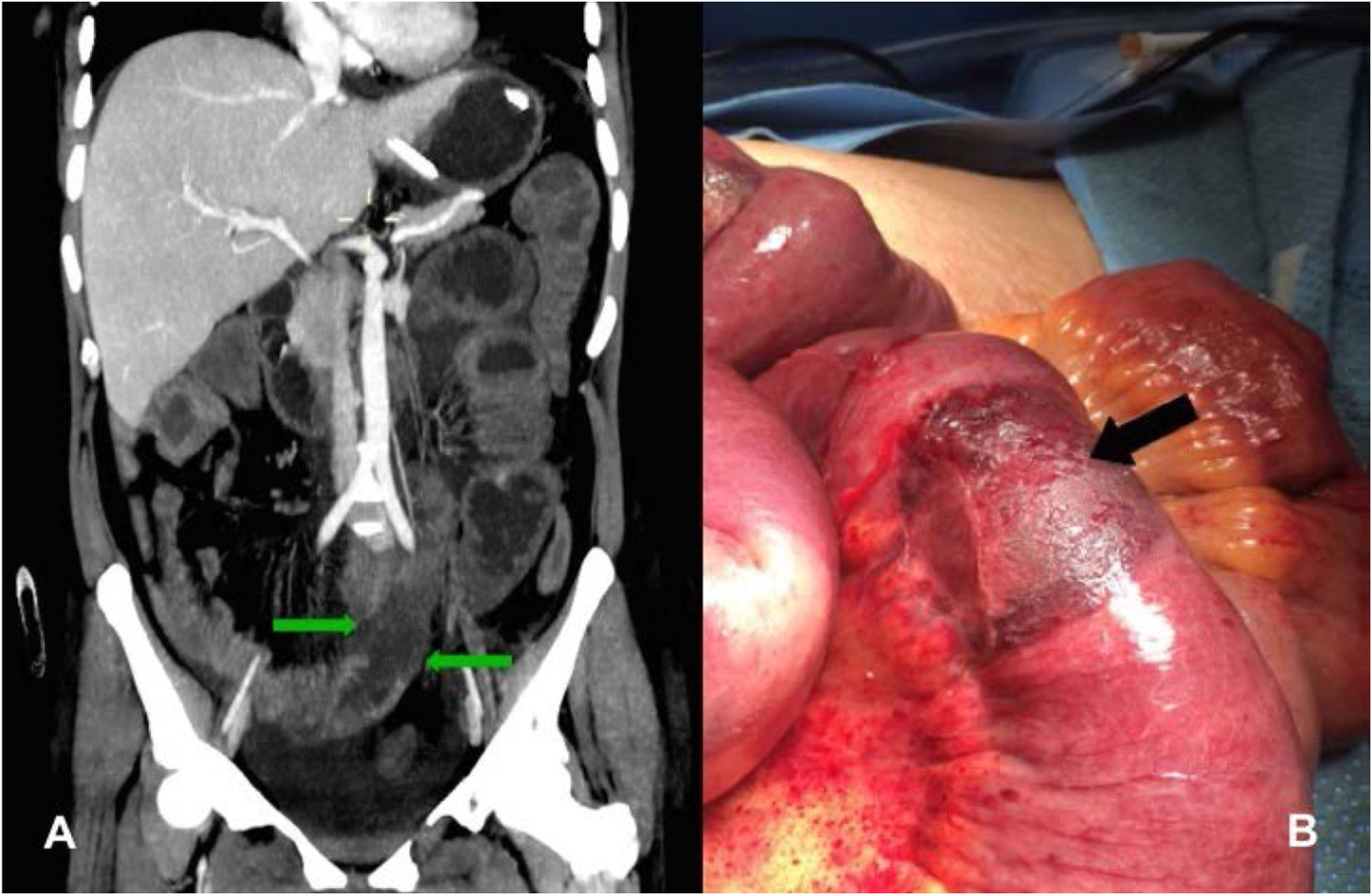
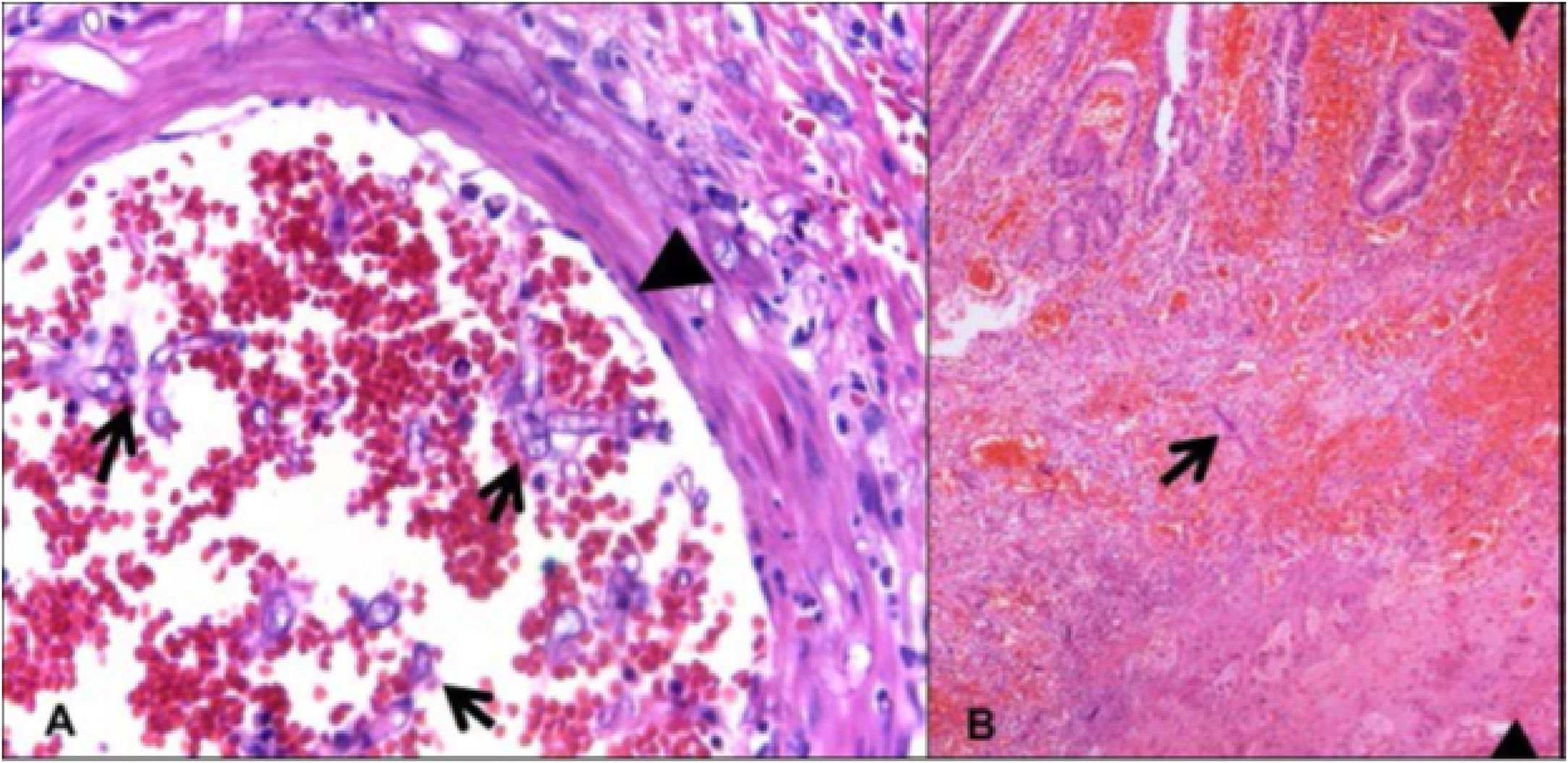
A 38-year-old woman diagnosed with acute myeloid leukemia sought medical attention at the emergency service due to painful abdominal syndrome. The patient was in her first relapse since treatment with chemotherapy and had no previous surgical history. Upon her arrival at the emergency service, she presented with diffuse abdominal pain, nausea, vomiting, and fever. Physical examination revealed abdominal distension and amphoric bowel sounds, and intestinal occlusion was diagnosed. Laboratory study results reported leukocytes 0.6 x 103/mm3 with 93.4% neutrophils (560/mm3 total) and lactate concentration of 2.3 mmol/l. Treatment was begun with fasting and a nasogastric tube, but after 48h the patient showed no clinical improvement. An intravenous contrast-enhanced abdominal tomography scan identified segmental areas of hypoperfusion in the wall of the small bowel (fig. 1A). The patient underwent exploratory laparotomy, revealing multiple circumferential lesions in the small bowel that appeared to be ischemic (fig. 1B). Intestinal resection and anastomosis were performed during the surgery. Figure 2 shows the histopathologic findings consistent with mucosal ulceration and bleeding, as well as thick hyphae with focal bulbous dilation and branching at right angles, resulting in the diagnosis of intestinal mucormycosis. Oral diet was begun on the third postoperative day and the patient received antifungal treatment with amphotericin B for 6 weeks. She was released on day 50 of her hospitalization.
Abdominal pain is estimated to be the reason for emergency service visits in 40% of patients with cancer. The gastrointestinal signs and symptoms in those patients can be directly related to the oncologic diagnosis or be complications of treatment with chemotherapy or radiotherapy. Chemotherapy can cause abdominal pain, nausea, vomiting, or diarrhea, whereas radiation can cause progressive occlusive vasculitis or intestinal stricture.3
Among the group of cancer patients that develop severe neutropenia and fever, more than 80% have hematologic malignancies resulting from clinically documented infections or positive hemocultures, 80% of which are caused by endogenous microbiota.4 The differential diagnosis for abdominal pain in patients with severe neutropenia is broad and includes neutropenic enterocolitis, Clostridium difficile infection, diverticulitis, appendicitis, and cholecystitis, among the most common pathologies.5
Patients with acute myeloid leukemia and deep neutropenia have up to 20 times more risk for invasive mycosis, the diagnosis and treatment of which is complex.4 Mucormycosis is an opportunistic fungal infection. It is caused by fungi that belong to the class Zygomycetes, the order Mucorales, the family Mucoraceae, and the genus Rhizopus is the most common. They are aerogenic microorganisms and therefore the main sites of infection are the paranasal sinuses and the lungs. Nevertheless, they have been documented to have different clinical forms, including rhinocerebral in 44 to 49% of patients, pulmonary in 10-11%, cutaneous in 10-16%, disseminated in 6-12%, and gastrointestinal in 2-7%. Despite its low frequency, intra-abdominal infection has devastating consequences, with a mortality rate as high as 85 to 90%.6
With respect to gastrointestinal site involvement, 57.7% of cases are in the stomach, 32.3% in the colon, 6.9% in the ileum, 7% in the esophagus, 2.3% in the duodenum, and 1.1% in the jejunum. Diagnosis has been reported to be antemortem in only 25% of the cases.7 Lesions are typically observed as dark ulcers with well-defined edges, with necrosis and thrombosis in the adjacent vessels. Histologic examination reveals thick hyphae with focal bulbous dilation and branching at right angles. Ninety-four percent of the specimens show zones of infarction and angioinvasion.8 Treatment consists of debridement, resection of the affected tissue, and antifungal therapy with amphotericin B.
Gastrointestinal mucormycosis is a diagnostic challenge for physicians and therefore requires a high degree of suspicion. The approach and treatment should be carried out by a multidisciplinary team.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureNo financial support was received in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Clemente-Gutiérrez U, Perez-Soto RH, Álvarez-Bautista FE, Domínguez-Rosado I, Cuellar-Mendoza M. Mucormicosis gastrointestinal: causa atípica de dolor abdominal en un paciente inmunocomprometido. Revista de Gastroenterología de México. 2019;84:409–411.