An anal fistula, or fistula-in-ano, is an abnormal granulating tract between the anorectum and the perianal region. Incidence varies between 0.86 and 2.32 per 10,000/year and is predominant in males, with ratios ranging from 2:1 to 5:1.1 Lipomas are benign soft tissue tumors composed of adipocytes within a thin fibrous capsule and account for almost 50% of all soft tissue tumors.2 Able to occur in any part of the body that has normal fat deposits, they develop where those deposits are greatest, such as the trunk, forearms, and thighs. Lipomas are rarely found in areas that naturally have little fat, such as the perineum.3 Soft tissue lipomas are commonly seen in daily practice and present in around 2% of the population.2
A 35-year-old man had an unremarkable past medical history, except for surgical drainage of a perianal abscess, 7 years prior. He arrived at our surgical clinic, presenting with a purulent discharge and drainage of pus near the anus that irritated the perianal space and the anal canal, causing itching and discomfort. He stated that his symptoms had not resolved since his initial procedure 7 years earlier and he complained of a painless lump in the left buttock of 4-month progression.
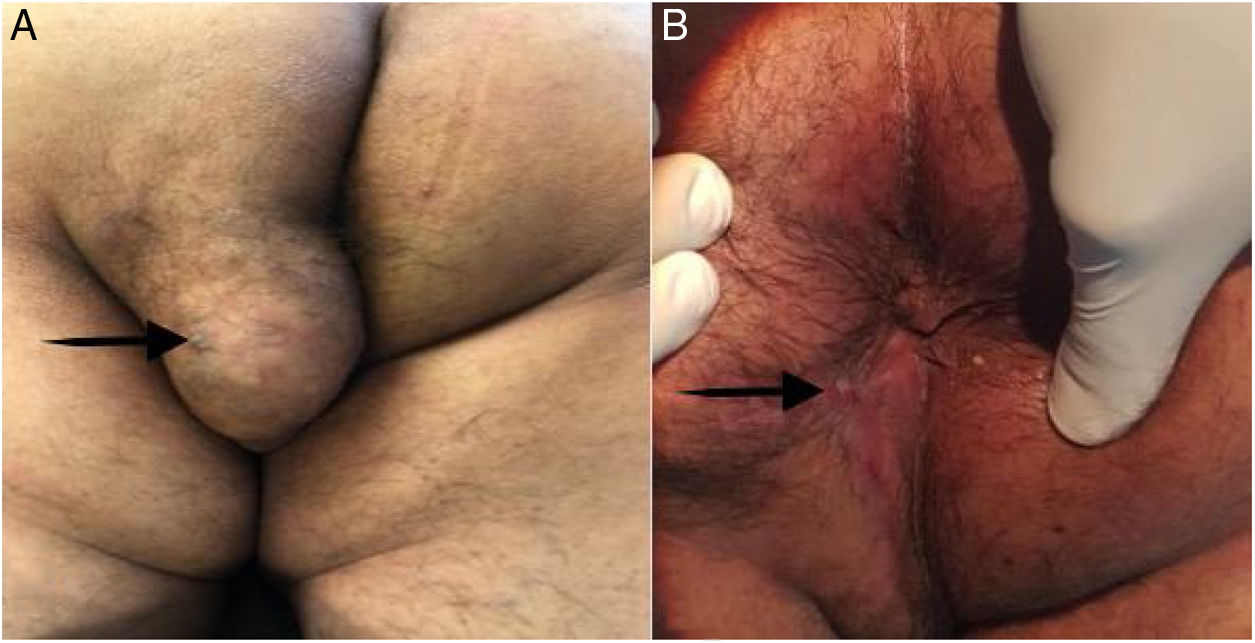
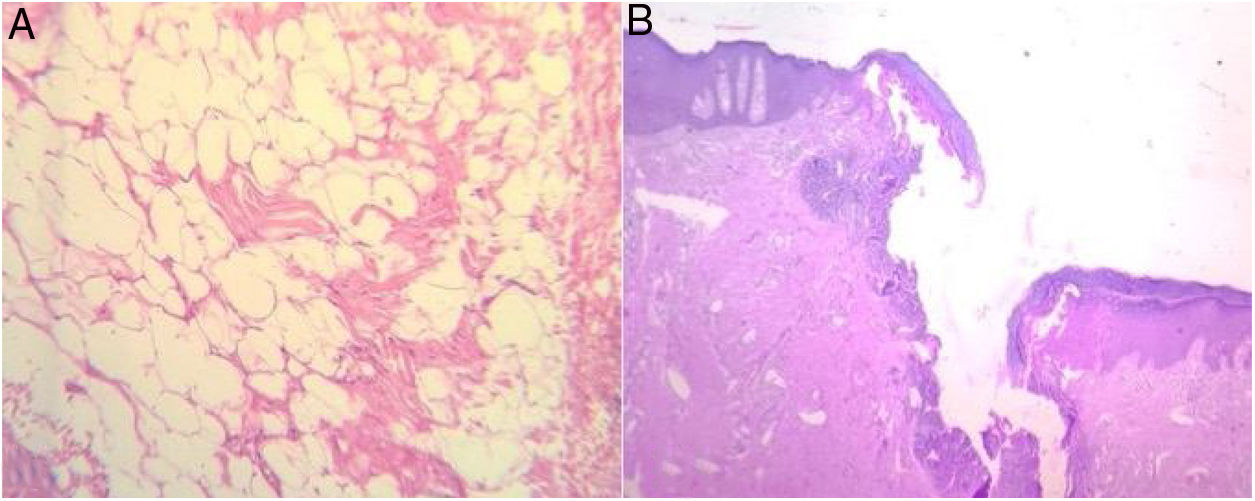
Physical examination revealed a well-defined, non-tender, freely mobile, 6×6cm lump on the left buttock whose overlying skin was normal in color, texture, and temperature. It was superficially situated on the subcutaneous plane, 3cm from the anal verge (Fig. 1A). The initial diagnosis was benign soft tissue tumor. Digital rectal examination revealed a fibrous cord beneath the skin, between the lump and the anal verge, that caused discomfort and pain. There was no evidence of swelling, purulent discharge, or internal masses. The patient was transferred to the operating room, and under regional epidural anesthesia, was placed in the jack-knife position. An anoscopy was performed, identifying the internal orifice of the communicating tract at the 7 o’clock position. An intersphincteric fistula passed from the internal opening into the lump, in a straight line. The fistula was de-roofed through careful diathermy, and the lump was excised, using an elliptical incision. The wound was left open and the tract and wound were packed. Upon gross examination, the tumor was soft and well-circumscribed by a thin fibrous capsule. The patient was discharged on postoperative day 4, with no complications. The histopathologic examination confirmed the diagnosis of lipoma, with a fistulous tract reaching the anal canal, and no evidence of malignancy (Fig. 2A and B). Six months after the initial procedure, the tract was obliterated, with no loss of sphincter function, and the wound was completely healed by secondary intention, with no significant deformities (Fig. 1B). At the follow-up at 12 months, the patient was healthy, with no complications.
(A) A well-defined, 6×6cm tumor in the left buttock and perineum. The black arrow points to the external orifice of the perianal fistula. (B) The perianal wound was healed by secondary intention, at the follow-up at 12 months. The black arrow points to the scar of the completely healed perianal fistula's external orifice.
An anal fistula is the chronic phase of an ongoing perianal infection. Most fistulas begin as anorectal abscesses. When the abscess opens spontaneously, a fistula may occur, which is then kept open by an infectious source.4 In over 90% of cases, anal fistulas are caused by infected anal glands, which provide free channels through which the infection can pass from the anal lumen into the deep sphincter muscles, becoming the chronic phase of an ongoing perianal infection. The infection penetrates the wall of the anal canal through a fissure or other wound, and once established, the infected tract is kept open by fecal content.5
Our patient had presented with a perianal abscess 7 years earlier, which we believe was the origin of the fistulous tract. Only the abscess had been treated at the time, and the fistulous tract was left intact. Most likely, over time, a soft tissue tumor developed at the site of the cavity of the previous abscess, with the internal orifice of the fistulous tract at the anal canal and the development of its external orifice at the site of the tumor.
The perianal region is a rare site for lipomas or soft tissue tumors. It is difficult for those patients to be in a seated position and there can be interference with defecation if there is intersphincteric extension or mechanical obstruction from swelling.3,6 Endosonography, computerized tomography, and magnetic resonance imaging (MRI) can be used in the diagnosis of perianal tumors, with MRI being the best modality for ruling out intersphincteric tumor extension.3,7 None of those imaging studies were available at our hospital, so we took the patient directly into the operating room to perform an anal examination under anesthesia, to determine the anatomic relation of the sphincters to the mass, and perform the necessary intervention. Perianal soft tissue tumors should be carefully dissected away from the perianal fat, always attempting to preserve the anal sphincters, if they are involved. In our patient, the anal sphincters were indirectly involved through communication with the tumor and so fistulotomy was performed, with no complications.
We found no cases in the literature of perianal lipoma with a fistulous tract reaching the anal canal and a surgical approach as the treatment of choice.
Ethical disclosuresThe authors declare that no experiments were performed on humans or animals for this report. It was approved by the ethics committee of the Tecnológico de Monterrey and complies with the norms of the bioethical research regulations.
A written statement of informed consent was obtained from the patient for the publication of this scientific letter and its accompanying images. A copy of the written consent statement is available for review by the Editor-in-Chief of this journal upon request.
FundingNo specific grants were received from public sector agencies, the business sector, or non-profit organizations in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: González-Urquijo M, Zambrano-Lara M, Espinosa-Loera JJ, Gil-Galindo G. Lipoma perianal con fístula interesfintérica en un paciente adulto. Revista de Gastroenterología de México. 2020;85:368–370.