Obesity is a serious disorder in almost the entire world. It is an important risk factor for a series of conditions that affect and threaten health. Currently, bariatric surgery is the most effective treatment for morbid obesity, and in addition to the resulting weight loss, it reduces morbidity in this population. There has been a significant increase in the number of obese patients operated on. Despite the success of bariatric surgery, an important group of patients still present with major postoperative complications. In order for endoscopy to effectively contribute to the diagnosis and treatment of complications deriving from obesity surgery, the gastroenterologist must be aware of the particularities involved in bariatric surgery. The present article is a review of the resulting anatomic aspects of the main surgical techniques employed, the most common postoperative symptoms, the potential complications, and the possibilities that endoscopic diagnosis and treatment offer. Endoscopy is a growing and continuously evolving method in the treatment of bariatric surgery complications. The aim of this review is to contribute to the preparation of gastroenterologists so they can offer adequate endoscopic diagnosis and treatment to this high-risk population.
La obesidad es un transtorno grave en casi todo el mundo. Representa un importante factor de riesgo para una serie de condiciones que afectan y amenazan la salud. En la actualidad, la cirugía bariátrica es el tratamiento más eficaz de la obesidad mórbida y resulta además de la pérdida de peso en la redución de morbilidad en esta población. El número de pacientes obesos operados se ha incrementado significativamente. A pesar del éxito de la cirugía bariátrica, un grupo de pacientes presentará complicaciones mayores en el postoperatorio. Para que la endoscopia contribuya en el diagnóstico y tratamiento de las complicaciones de la cirugía de la obesidad, es necesario que el gastroenterólogo esté familiarizado con las particularidades de la cirugía bariátrica. En el presente artículo revisamos los aspectos anatómicos resultantes de las principales técnicas quirúrgicas empleadas, los síntomas más comunes en el postoperatorio, las ponteciales complicaciones y las posibilidades de diagnóstico y de tratamiento endoscópico. La endoscopia, en el tratamiento de las complicaciones de la cirugía bariátrica, es un área que está en crecimiento y en continua evolución. El objetivo de esta revisión es contribuir para la preparación de los gastroenterólogos para que ofrezcan diagnóstico y tratamiento endoscópico adecuado a esta población de alto riesgo.
The prevalence of obese patients has increased worldwide1. Obesity is associated with a series of conditions that threaten health, and therefore is a serious public health problem2,3. Clinical treatment has no long-term satisfaction for an important fraction of obese patients4,5. Surgical treatment is considered efficacious in relation to weight loss, maintaining that loss, and improving long-term morbidities6,7. The number of bariatric surgeries has increased systematically each year8. Bariatric surgery has a mortality rate lower than 1% in referral centers9, with an estimated 5-10% of the patients having acute complications and 9-25% late complications10. Endoscopic study after obesity surgery has well-defined indications for symptom evaluation, the diagnosis of complications, and eventually for therapeutic procedures11,12. In order for endoscopic study to contribute to the diagnosis and treatment of complications deriving from obesity surgery, adequate knowledge of the anatomic aspects resulting from the surgical techniques employed is necessary, as well as their potential complications and management13,14.
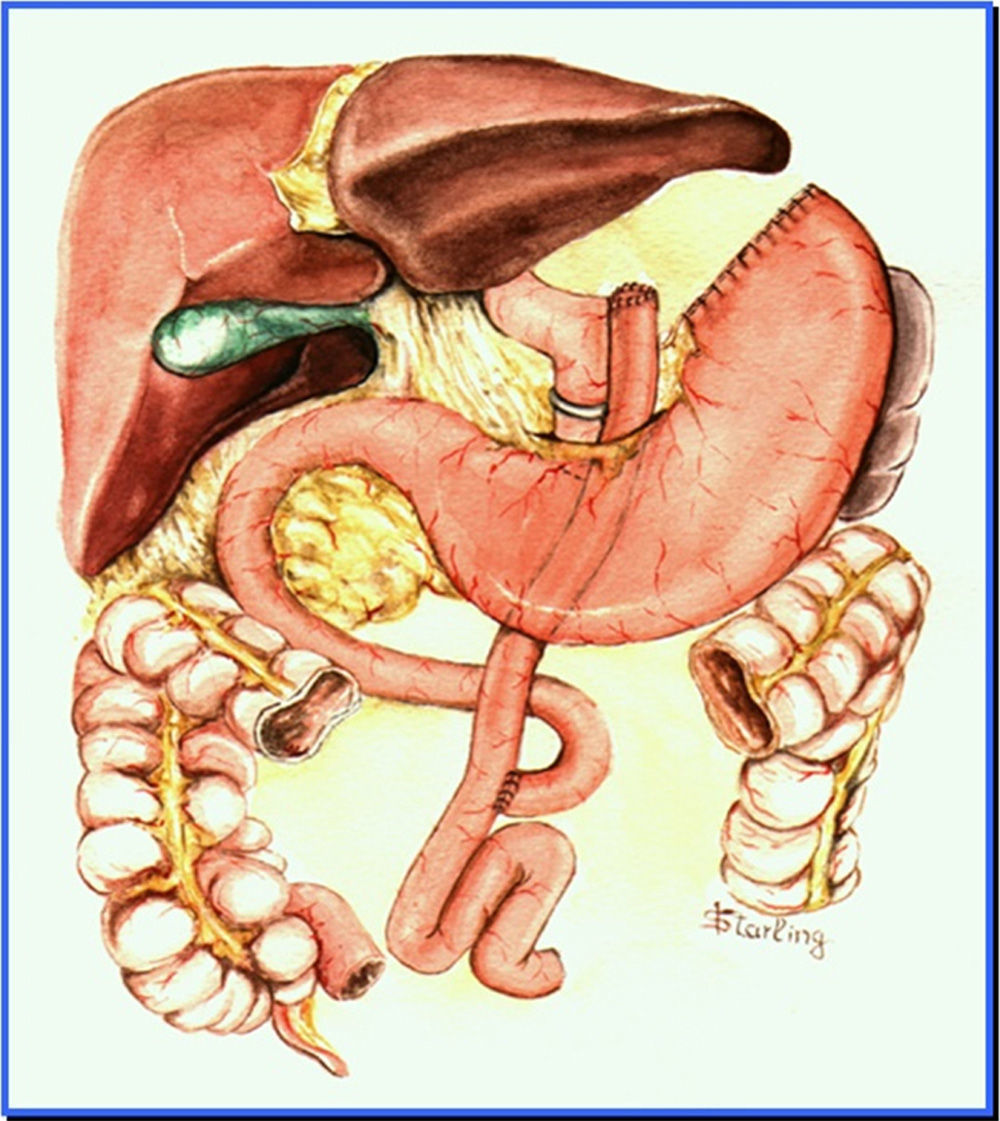
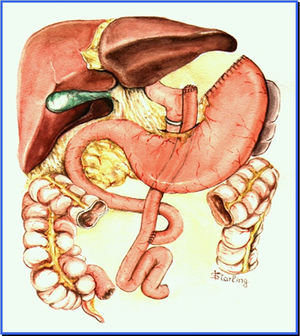
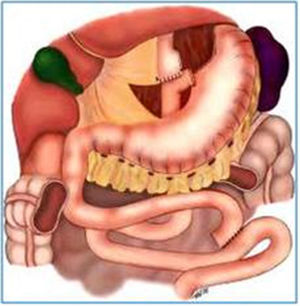
Endoscopic aspects of banded Roux-en-Y gastric bypass (Capella surgery)For many years, the most widely used technique was the Capella surgery15, in which the stomach is stapled and sectioned forming a small reservoir next to the cardia, called the gastric pouch. The rest of the stomach, duodenum, and part of the proximal jejunum are excluded from food transit. It is reconstituted with an end-to-side anastomosis between the gastric pouch and a Roux-en-Y loop of the jejunal segment (fig. 1). At endoscopy, the gastric pouch begins just below the esophagogastric transition and extends for 5-7cm. Sometimes the suture line of the gastric section can be seen. A synthetic band is placed externally around the pouch to limit its emptying, and when examined endoscopically, it is viewed as a 12mm annular impression at the most distal portion of the pouch. The gastrojejunal anastomosis has a diameter of approximately 12-14mm and is observed just below the band. The afferent segment loop is short, ends in a blind fundus, has a sharp angle and is imbricated at the suture line of the gastric pouch - a modification proposed by Fobi16. The efferent segment loop is long and remains available almost at the same axis of the pouch. The endoscopist must be aware of the esophageal mucosa, the size and integrity of the gastric pouch, especially at the suture line, the positioning and caliber of the band, the aspect of the anastomosis, and the proximal jejunal mucosa17,18.
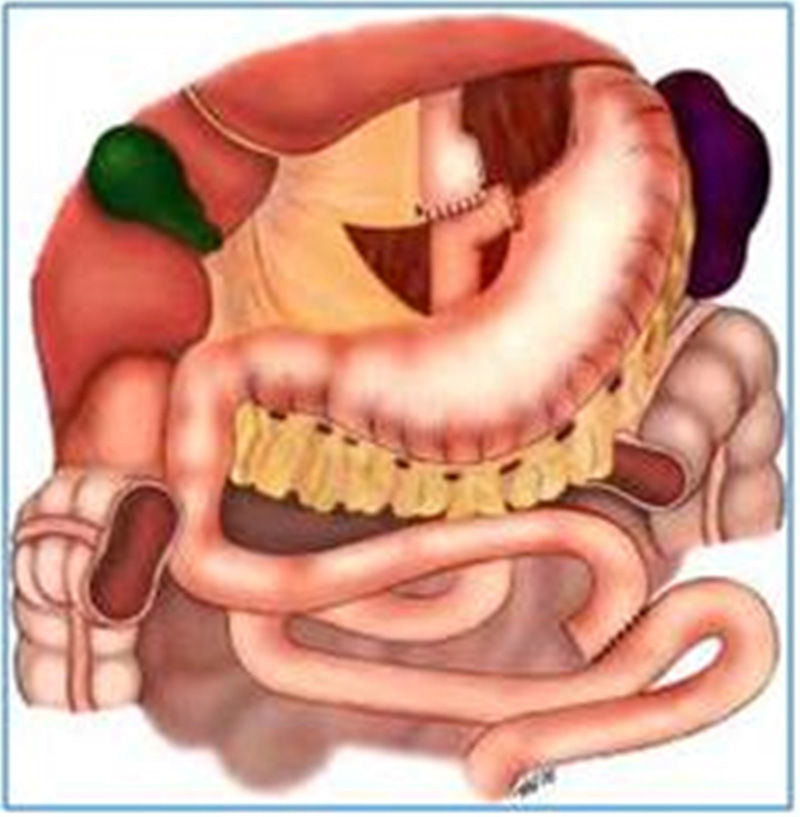
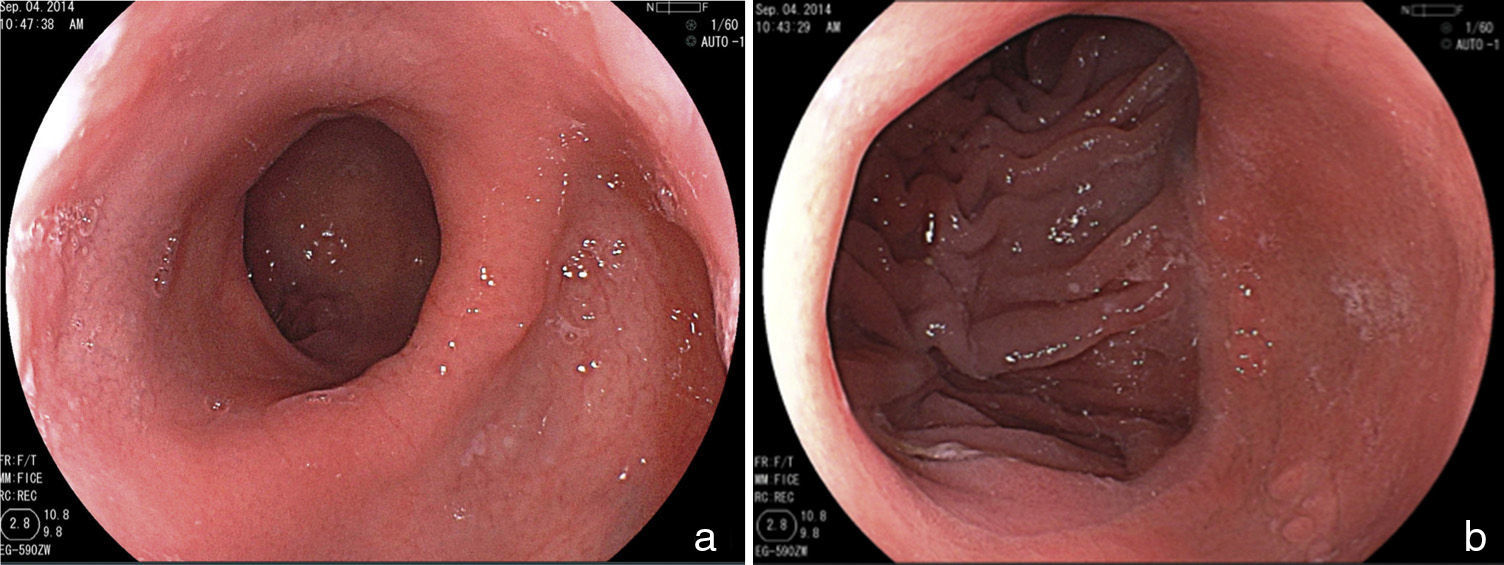
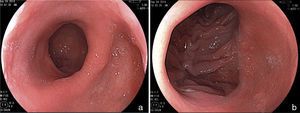
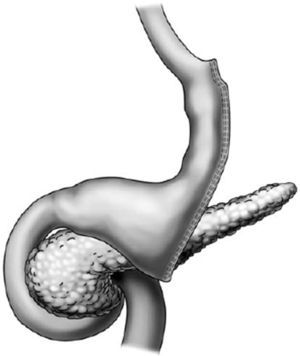
Endoscopic aspects of the Roux-en-Y gastric bypassThis is currently the most frequently performed surgery for obesity and is preferably done through laparoscopy. The technique is practically the same as that of the Capella surgery, but with no band placement and with the elaboration of a smaller pouch, especially at the side of the greater curvature. Either an end-to-end or end-to-side anastomosis is performed with a reduced caliber, which substitutes the restrictive effect of a band11,18 (fig. 2). The endoscopic aspect is similar to that of the Capella surgery (banded gastric bypass), with a tendency toward a smaller pouch and smaller caliber anastomosis, and obviously no band impression is observed17–19 (fig. 3).
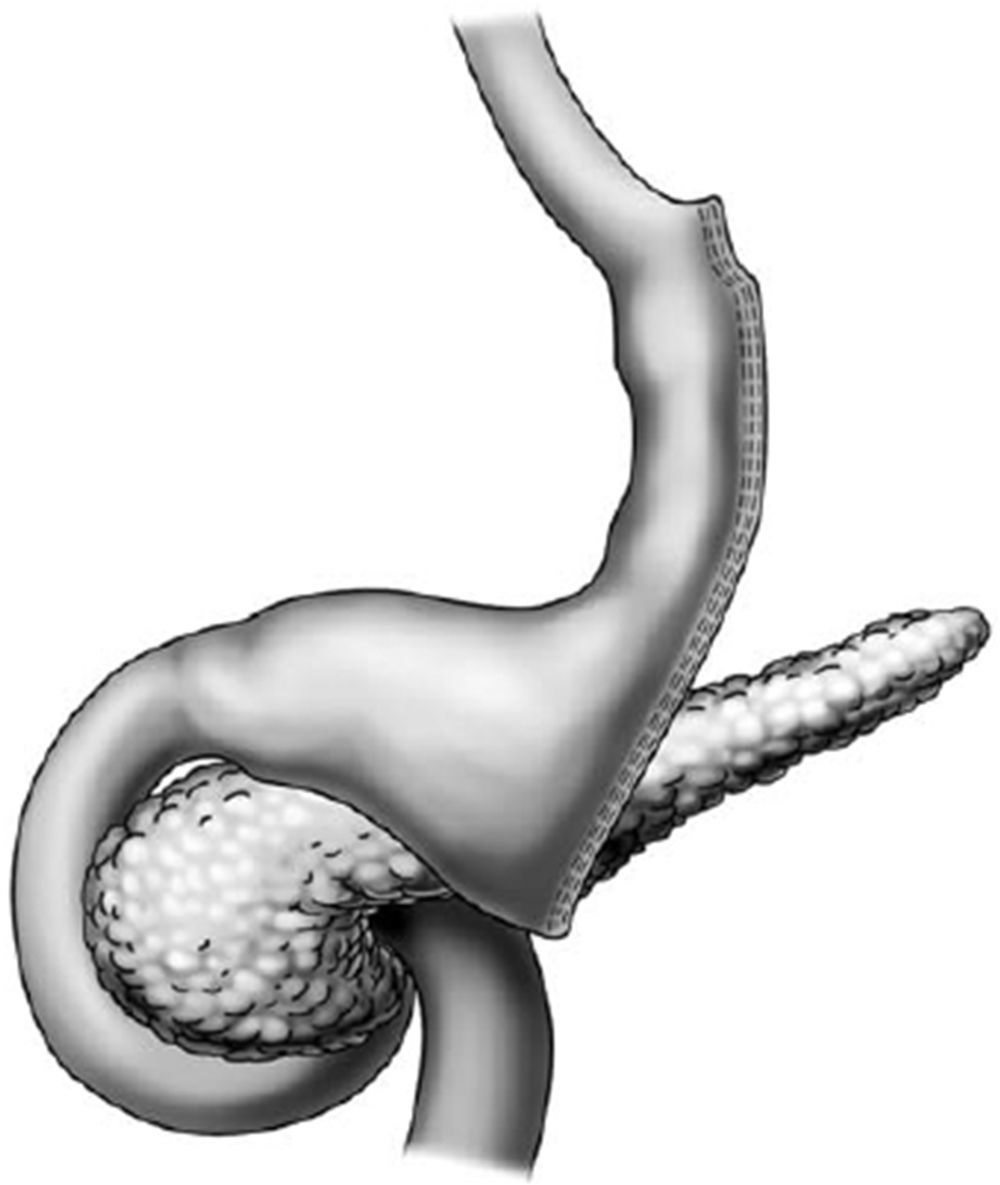
Endoscopic aspects of the vertical gastrectomy (Sleeve gastrectomy)Vertical gastrectomy is a purely restrictive technique. The greater curvature and the gastric fundus are resected, forming a vertical tube and resulting in a smaller volume stomach. The resection is done 7cm from the pylorus up to the His angle (fig. 4). At endoscopy we observe the proximal part of the gastric sleeve tunneled up to the angular incisura, where an intentionally constructed angulation is noted that impedes gastric emptying. After the angulation, the conserved antrum and duodenum are seen. The endoscopist should observe the esophageal mucosa, the esophagogastric epithelial transition, the axis of the tunneled portion, the transition of the tunneled portion of the antrum, and the antral and duodenal mucosa17–19.
Endoscopy in the immediate postoperative periodThis should be carried out with care and a minimum insufflation of air, even though it rarely results in complications20,21. In the first postoperative days, endoscopy is hindered by edema and friability of the regions of the band and the anastomosis. Its performance could be imperative if there is bleeding, manifested as hematemesis or melena. Bleeding occurs in the immediate postoperative period in 1-5% of the cases of gastric bypass22,23. One study demonstrated that bleeding presented during the first 4h in 70% of the patients24, but it is rare after vertical gastrectomy or band laparoscopy25. The hemorrhage rate is higher in laparoscopic gastric bypass (5.1%) than in access through laparotomy (2.4%), and re-bleeding is also greater in the laparoscopic group22. In a review of 933 patients that underwent gastric bypass, the rate of bleeding was 3.2%. Of those patients, 47% had one episode, 43% had 2 episodes, and 10% had 3 episodes23. Endoscopic examination is not always necessary, given that hemorrhage can be mild and/or self-limited. If bleeding is severe or recurrent after conservative management, endoscopy should be performed25. Bleeding commonly arises in the gastrointestinal anastomosis, with the possibility of endoscopic hemostasis14,25. The use of endoclips is a better option, compared with thermal methods, because it minimizes the lesion in the anastomosis and should be accompanied with the use of an adrenalin solution, given that the double therapy has better results13,26. In a review of 89 patients with immediate post-bypass bleeding, 77% were treated conservatively and diagnostic and therapeutic endoscopy was performed in only 6 (6.7%) and 5 (5.6%) of those patients, respectively27. In another report, endoscopy was performed on 27 out of 30 patients (90%), and bleeding arose from the gastrojejunal anastomosis in all the cases23. In 85% of those patients, there was active bleeding or blood stigmata, and therapeutic endoscopy with injection, thermal coagulation, or endoclip placement was employed. Bleeding was initially controlled in all the patients, but 5 (17%) had rebleeding and underwent repeat therapeutic endoscopy. Less commonly, hemorrhage can occur at the section line of the gastric pouch, the enteroenteric anastomosis, at another point of the small bowel or colon, or in the excluded stomach11,13,28.
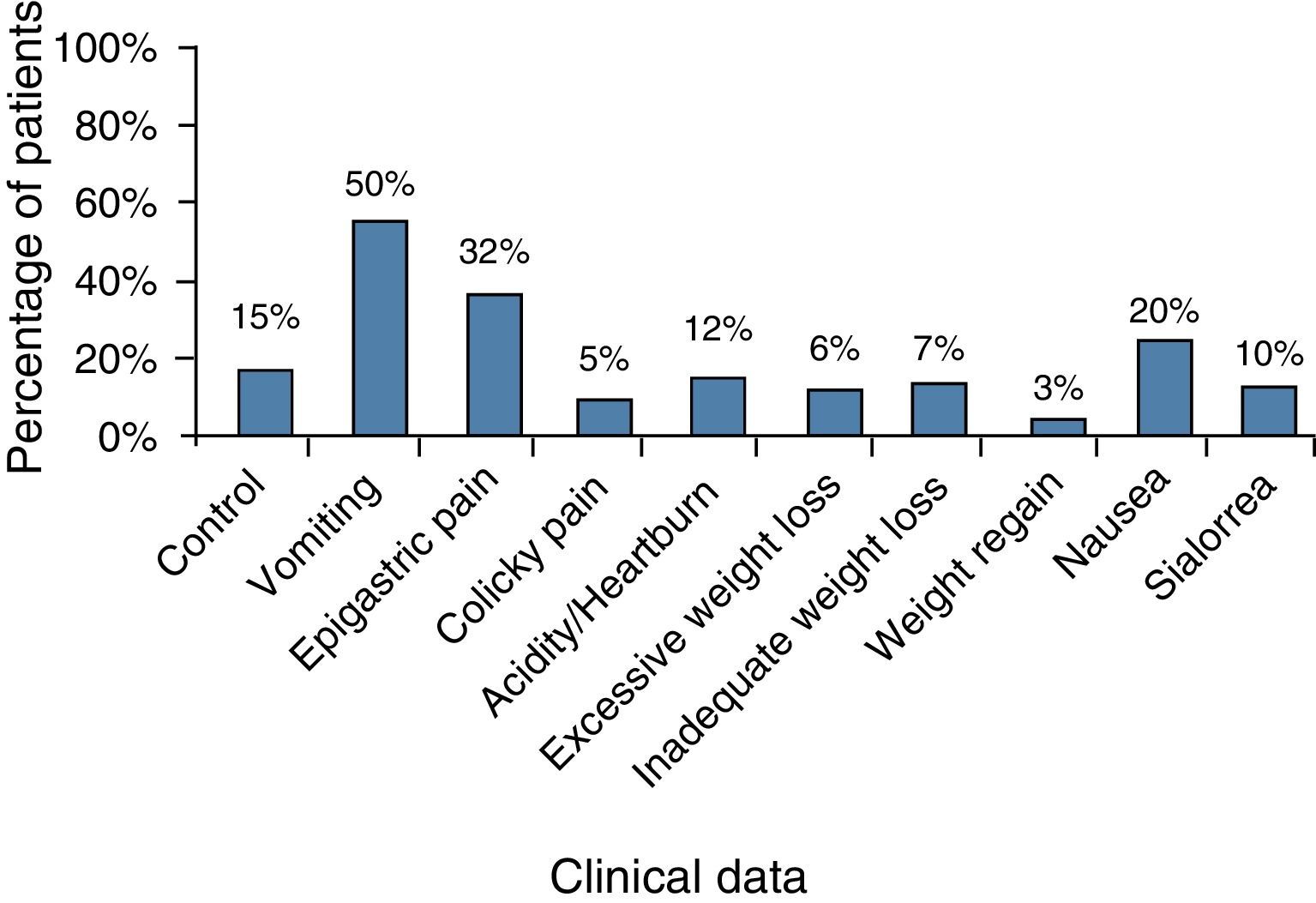
Endoscopy in the late postoperative periodThis can be performed, in the absence of symptoms, to certify and evaluate the surgical technique19. This indication is questioned by some, in relation to cost-benefit29. Endoscopy will be performed in 20-30% of the patients in the presence of symptoms that may occur19,30 that mainly include abdominal pain, nausea and vomiting, reflux symptoms, dysphagia, and weight-related problems11,19,31,32. Table 1 shows the endoscopy indications in 218 patients in the first postoperative year32. Esophagitis, marginal ulcer, anastomosis stricture, erosion, band slippage, hemorrhages, and fistulas were among the main endoscopic findings, with variable incidence according to the characteristics of the patients studied13,14,19,21.
Nausea and vomitingThese are not unusual in the first days, and normally last around one week. They are related to the use of medications, edema of the anastomosis, transitory dysmotility, or more frequently, to a combination of these factors33. When they do not disappear or improve enough to allow the ingestion of liquids, endoscopy is indicated31. These are complaints that also occur after the first postoperative weeks and, in themselves, are not an indication for endoscopic study14. In general, there is a tendency for improvement in regard to vomiting within 1-6 months, and close to 75% of patients will no longer present with vomiting, or if so, only sporadically34. Characterizing the vomiting is important in relation to aspect, if it is the clear saliva type or if there are food residues, in relation to frequency, if it is constant or postprandial, in relation to the number of episodes, its association with sialorrhea, dysphagia, or pain, and its correlation with surgery duration33,34. Endoscopy indication should take these factors into account so that, on the one hand, unnecessary studies are avoided, and on the other, diagnosis of stricture of the band or anastomosis, or even of food impaction, can be made11,12,19.
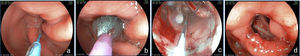
Inadequate weight lossWeight loss is greater in the first 6 months and decreases after that period. It is expected to be mild and constant up to 12 or 15 months, reaching up to a 45% loss of the initial weight6,7. Some patients may regain from 5-10% of their weight loss 2-4 years after surgery, which is acceptable35. It is estimated that from 18-30% of the patients can regain almost all the weight lost, characterizing surgical treatment failure35,36. Even if inadequate results in relation to weight loss are related to dietary, behavioral, or hormonal problems37, alterations susceptible to endoscopic management may be involved. Endoscopy is indicated when there is insufficient or exaggerated weight loss or when more weight than the weight that was lost is regained38. When there is insufficient loss, diagnosis may be fistulas between the gastric pouch and the anastomosed segment (gastrojejunal) or between the pouch and the excluded stomach (gastrogastric) and partial or total band erosion. Large pouches and dilated anastomoses can also be correlated with insufficient weight loss13,19,39. There are cases of endoscopic interventions on the dilated anastomosis to reduce its caliber and induce weight loss with the injection of sclerosants40, argon gas fulguration41, (fig. 5), and endoclip application42. Utilizing these methods, 64% of patients can lose up to 75% of the regained weight43,44. There are reports of experimental endoscopic interventions with different suturing platforms for reducing the diameter of the anastomosis or the size of the pouch. These techniques include plicatures with systems such as the EndoCinth45, Apollo OverStitch46, StomaphyX47, Rose, and BOB48. Likewise, endoscopic treatment of the gastrogastric and gastrointestinal fistulas is possible through suturing with these same systems13,48,49. These different approaches are successful in inducing weight loss in 75% of the patients48,50,51. Nevertheless, the long-term effect of these procedures on the anastomosis and the maintenance of these plicatures is not known. Thus, further studies are needed to determine the impact of these procedures, keeping in mind that weight loss is multifactorial13,48.
Marginal ulcerMarginal or anastomotic mouth ulcer can occur after gastric bypass for obesity, and is described both within the first days and many years after the surgery52. Incidence varies from 0.5-20%12,53 and depends on a series of factors. These include the frequency with which exploratory endoscopy is carried out, the time at which it is done, and the empirical treatment rate before endoscopy12,53. The incidence of marginal ulcer was greater in cases in which the 2 gastric chambers were not sectioned, given that the sleeves were able to be rechanneled, allowing the acid from the excluded stomach to directly reach the jejunal mucosa54. With the transection of the 2 gastric chambers and the interlaying of the segment between them, the possibility of fistula is rare54, reducing the incidence of ulcer11,13. Another technical aspect to consider is the fact that a large gastric pouch would have a greater production of acid and a greater probability of ulcer54. The current tendency of a small pouch reduces that incidence52,55. Likewise, marginal ulcer occurs in 0-6% of bypass surgeries30,55. Some surgeons separate the marginal ulcer of the stoma (of the suture line, gastric margin) from the marginal ulcer (of the jejunal mucosa, adjacent to the anastomosis)12,19. In cases of marginal ulcer, related to the factors described above, the lesion occurs later, can be single or multiple, and is located in the jejunal mucosa, adjacent to the anastomosis13. The ulcer of the stoma can also occur due to technical factors related to anastomosis and Roux-en-Y performance and not as a result of a large pouch, fistulas, or some other ulcerogenic factor. These ulcers are generally caused by the presence of a foreign body (suture thread) at the suture line52,55, diminished blood supply in the jejunal mucosa, compression and edema in the anastomosis, or tension due to a short mesentery55,56. These ulcers occur in the early postoperative period and are observed at the suture line, sometimes on a surgical thread, and they cicatrize in 2 or 3 months, mainly if the causal agent is removed56,57. Other factors related to marginal ulcer etiology are smoking, alcoholism, and the use of acetylsalicylic acid and anti-inflammatory drugs52–56. Some studies have analyzed the effect of Helicobacter pylori (H. pylori) on the development of ulcers after bariatric surgeries11,13. Serology is the best method for detecting H. pylori in this population, because pouch biopsies and breath tests can give false negatives13,56. The rate of infection in gastric bypass surgery is low and its role in the origin of marginal ulcer is not yet well defined12,52,56. Therefore, investigating the bacterium in the pouch and its treatment can only be done empirically. Abdominal pain is the most common symptom in patients with ulcer11–13. Nausea and vomiting can be present, with or without pain, and massive bleeding is uncommon52. Diagnosis is imminently endoscopic. Early ulcers, related to problems at the suture line, tend to spontaneously cicatrize52,56. Recurrent or persistent ulceration, associated with the presence of a foreign body, can be treated through endoscopic extraction of the foreign body57,58. The endoscopist can remove suture threads when they are visible in the lumen and if they are associated with a marginal ulcer. This behavior potentially facilitates cicatrization and thus alleviates symptoms of abdominal pain25. Ulcers caused by problems in the pouch construction, normally located in the jejunal mucosa, should be treated with proton pump inhibitors together with sucralfate. Cicatrization time can vary from 8 weeks to 6 months12,13,56. A review of the surgical procedure is necessary in cases of gastrogastric fistulas or large pouches and ulcer intractability12,13,53.
Food bolus impactionPatients that undergo Capella surgery have a small gastric pouch whose emptying is limited by the silicon band. In Roux-en-Y gastric bypass with no band, the anastomosis has a smaller caliber and also limits the emptying of the pouch. In some situations, through error or dietary abuse, difficulty in chewing, or stricture of the anastomosis or band, these patients can present with impacted food or food boluses in the pouch. In these cases, the patient complains of sialorrhea, dysphagia, odynophagia, and the sudden onset of nausea and vomiting19,59. Some patients state they have partial and temporary improvement after vomiting and they are able to drink small quantities of water, which can probably be explained by a valvular mechanism. Endoscopic study should be performed with special care to avoid bronchial aspiration59. The food bolus that is normally free in the gastric pouch can be made of meat, fruit seeds, or other less common foods. The endoscopist must evaluate the size and consistency of the impacted material and choose the best accessory and most adequate technique for its removal59,60. A polypectomy loop, Dormia basket, or biopsy or foreign body forceps can be used and the food bolus can be removed through the oral cavity, fragmented, and pushed beyond the band and the anastomosis, or aspirated with an elastic ligature cap59,60. During or after removal of the food bolus, the endoscopist must carry out a complete endoscopic examination, searching for obstructive alterations that explain the impaction. It is important to identify the alteration because this will determine the behavior to be adopted: a simple dietary reorientation or endoscopic or surgical resolution of the obstructive factor19,59.
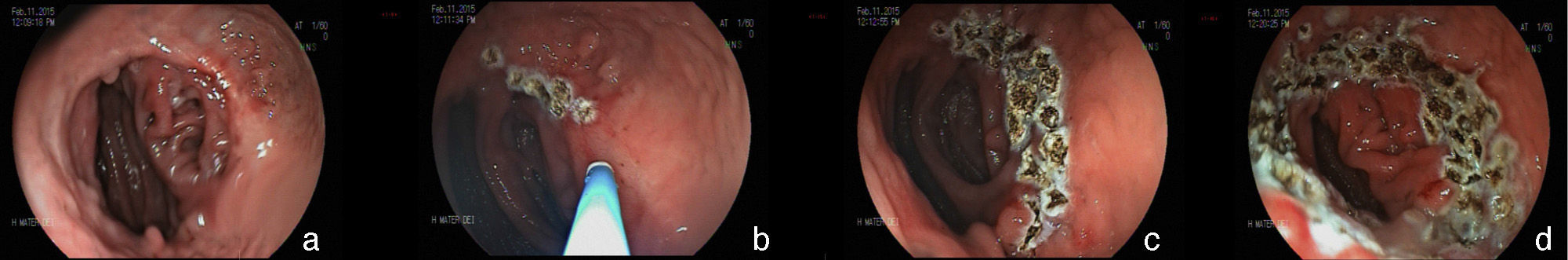
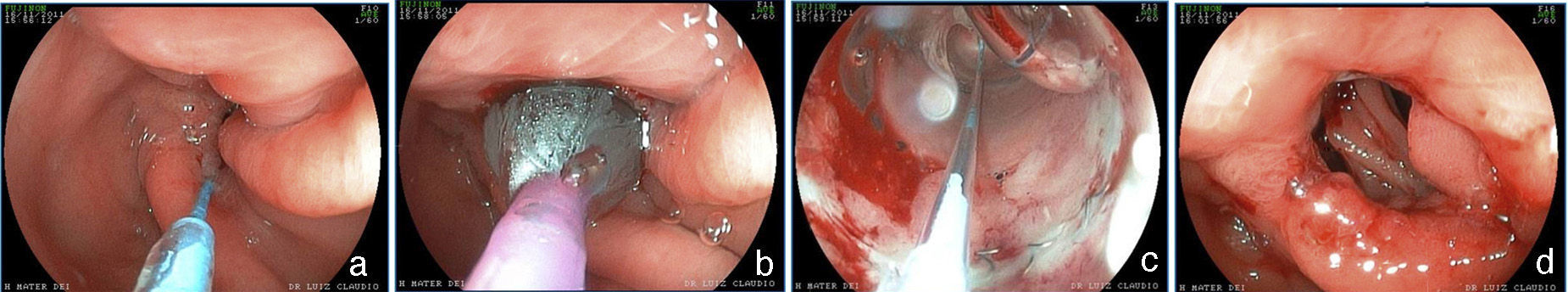
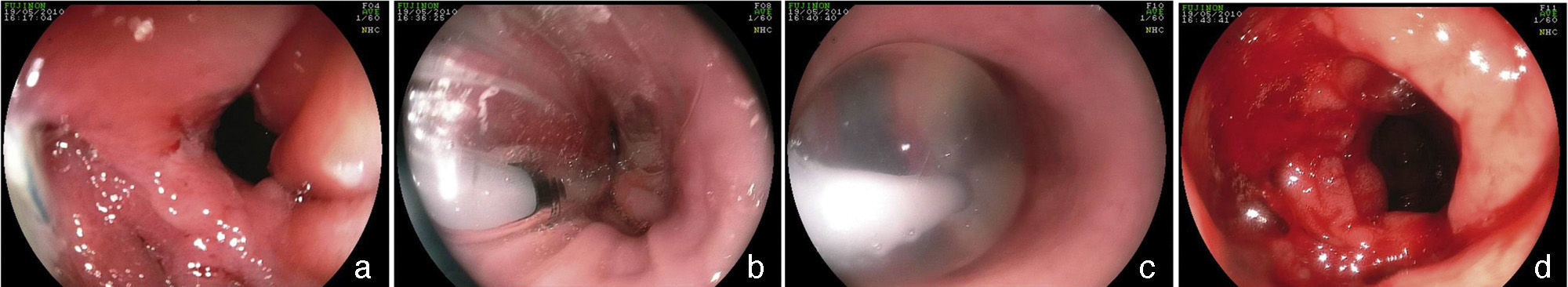
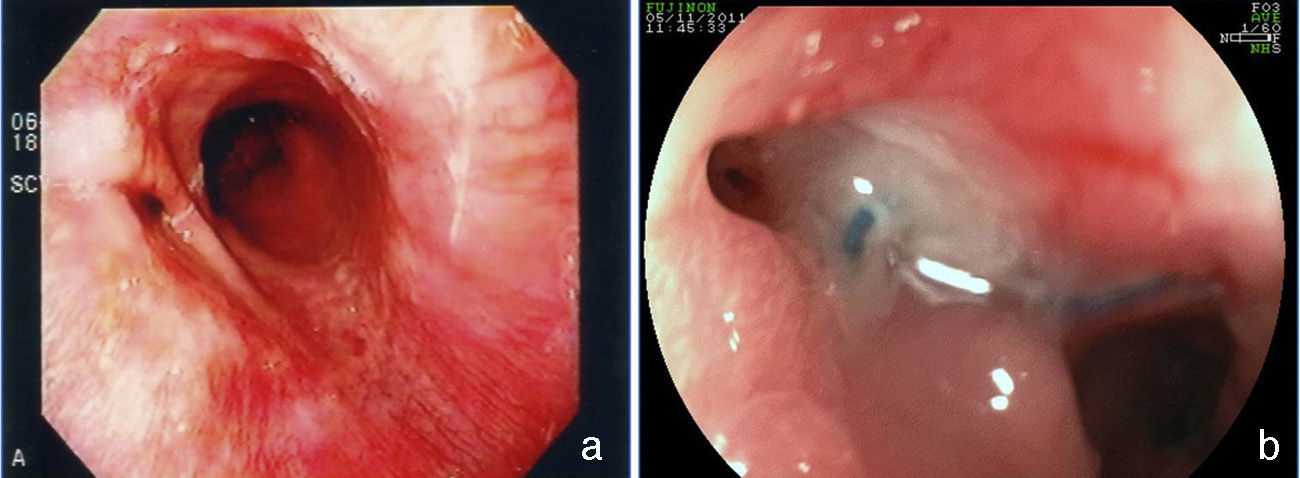
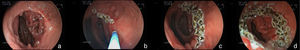
Stricture of the anastomosis and the bandStricture of the gastrojejunal anastomosis in Roux-en-Y gastric bypass has a frequency of 3-19%61–63. This variation is partially explained by the differences in technique64. In gastric bypass with no band, a lower caliber anastomosis is attempted and the incidence of stricture is slightly higher65. Incidence is higher with the laparoscopic access (5-12%) than with open surgery (3-5%)62,66. Stricture generally derives from some complication of the surgical technique, such as: dehiscence, hematoma, or ulceration, processes that produce fibrosis and retraction13,19,67. The patient can present with eating difficulties, especially with solid foods, as well as nausea and vomiting, between 4 and 10 weeks after surgery60,65,67. The endoscopic aspect is of an anastomosis with annular stricture, fibrotic, with a punctiform caliber that impedes the passage of the endoscope13,67, and sometimes with an ulcer in the adjacent mucosa67. Treatment is endoscopic through dilations with hydrostatic balloons introduced through the working channel of the endoscope and allowing the passage of a thread-guidewire67–69 (fig. 6). The balloon must be carefully passed through the punctiform stricture, because the blind afferent segment and the intestinal portion of the anastomosis are distal to the stricture13,67. Likewise, to prevent complications, such as perforation, which occur in an average of 2.2% of cases67, the balloon should be carefully passed in the direction of the efferent segment; this is facilitated by the previous passage of a guidewire that can be monitored by fluoroscopy11. Normally, initial dilation can reach up to 15mm, the same as in punctiform strictures70. However, progressive dilation, up to 12mm in the first session and 13.5 and 15mm in the subsequent sessions performed after 7 or 15 days, appears to be safer and with a lower complication rate11,12. In gastric bypass with no band, some authors recommend not to exceed 12-13mm, considering the possibility that it could result in a very wide anastomosis, which could have a long-term impact on weight loss71,72. Dilation with Savary-Gilliard dilators has been reported and in a review comparing the 2 methods, the result was similar, with a need for 2 or 3 dilations and a 3% complication rate67. Nevertheless, progressive dilation with a guided balloon, mainly in punctiform strictures, appears to be safer and more effective13,73. The majority of cases are resolved in 2 or a maximum of 3 sessions, with a resolution rate of 95 to 100%67–69,74. The smaller caliber band leading to stricture is less common, occurring in 1-2% of the patients21. Clinical symptoms are similar to those of anastomosis stricture. In the endoscopic examination, there is intense edema in the mucosa in the region of the anastomosis and no aspect of fibrosis or cicatrization, suggesting that there is very tight extrinsic band compression. Sometimes, when the endoscope approaches the band, it is possible to distally identify the line of the normal caliber anastomosis32. Balloon dilation up to 20mm is not effective and eventually can worsen symptoms due to the inflammatory reaction and edema caused by the compression of the mucosa against the band75. One option is dilation with an achalasia balloon (30mm), positioned like a Savary-Gilliard guidewire76. The goal is the rupture of the thread that internally sustains the band or simply the definitive increase in the diameter due to the elasticity of the thread (fig. 7). It is a complex technique that should be performed under fluoroscopy and its main potential complication is perforation. In addition to this alternative, surgical treatment should also be considered.
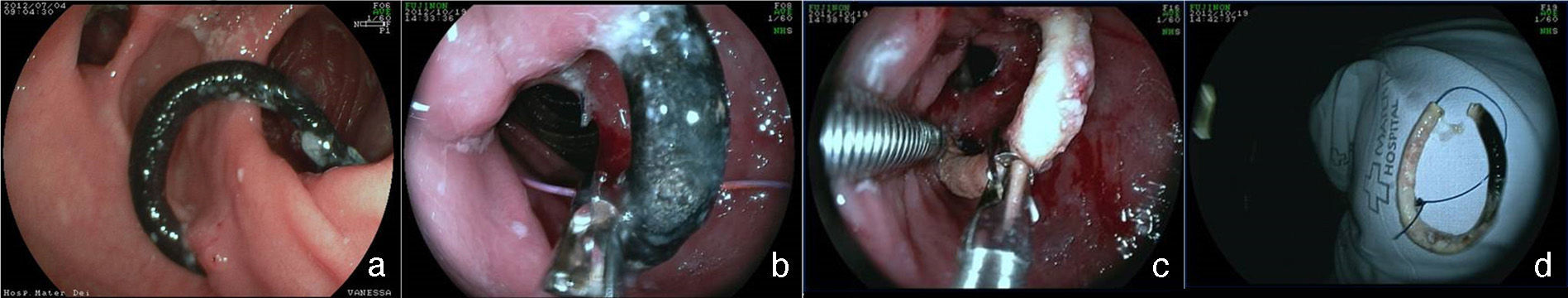
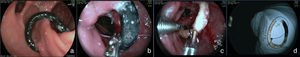
One band complication is ulceration of the mucosa due to band compression and its partial or total migration into the gastric lumen. In large case series, overall incidence of band migration to the lumen is around 1.6%21,59. This complication occurs in 0.9% of the primary surgeries, in 5.5% of the re-interventions, and in 28.5% of the surgeries with band replacement after previous band migration77. Band migration begins with an inflammatory reaction between the band and the gastric wall. Its cause is very tight placement of the band, suturing of the band to the stomach, or the presence of local infection75. This complication can be asymptomatic or can more commonly present as a syndrome of obstruction, causing nausea, vomiting, and weight loss. Other possible symptoms are epigastric pain, dysphagia, and more rarely anemia, hematemesis, or melena32. Endoscopy enables a precise diagnosis, showing the erosion or ulceration with partial band migration. Treatment can be surveillance, endoscopy, or surgery. Surveillance may be indicated in those asymptomatic patients with satisfactory weight loss and in whom only a small portion of the band has migrated. Removal is the treatment of choice78. Normally, the band is sectioned with endoscopic scissors or a guidewire fit to a mechanical lithotripsy system (fig. 8), in the same way as the removal of the migrated gastric band78,79. Sometimes the aid of an extra channel in the endoscope is necessary26. Another possibility for removing the migrated, eroded, or strictured band is passing a self-expanding stent that induces complete band migration and then 6-8 weeks later, remove the stent and the ring together79,80. One must be alert as to the possibility of the formation of a fistula, though rarely described, that is most likely due to the intense fibrotic process surrounding the region that also makes surgical treatment technically difficult13,32. The effect of band removal on weight loss and maintenance of that loss is not yet defined. Weight regain (from 61-75% of the weight previously lost) can occur in close to 14% of patients when the band is removed within the first 6 months, compared with 6% when removal is after that period77. Band slippage is an even rarer complication and occurs in less than 1% of the cases21,59. Inadequate band attachment can lead to displacement, usually of the anterior portion, up to the region of the anastomosis. The clinical symptom is obstruction, with vomiting and excessive weight loss60. The band can be seen out of its habitual position through radiographic imaging. The endoscopic aspect is characteristic; the pouch is a bit dilated with no annular compression of its most distal portion, the jejunal mucosa is partially everted, and the compression of the band at some portion of the segment can be observed, leading to a punctiform stricture75. In general, the endoscope cannot pass and food residuals can be seen in the pouch and even in one of the segments. Techniques of band dilation with a 30mm achalasia balloon76 or the placement of a stent have been described for treating this complication78,80, but surgical band removal is more frequently performed.
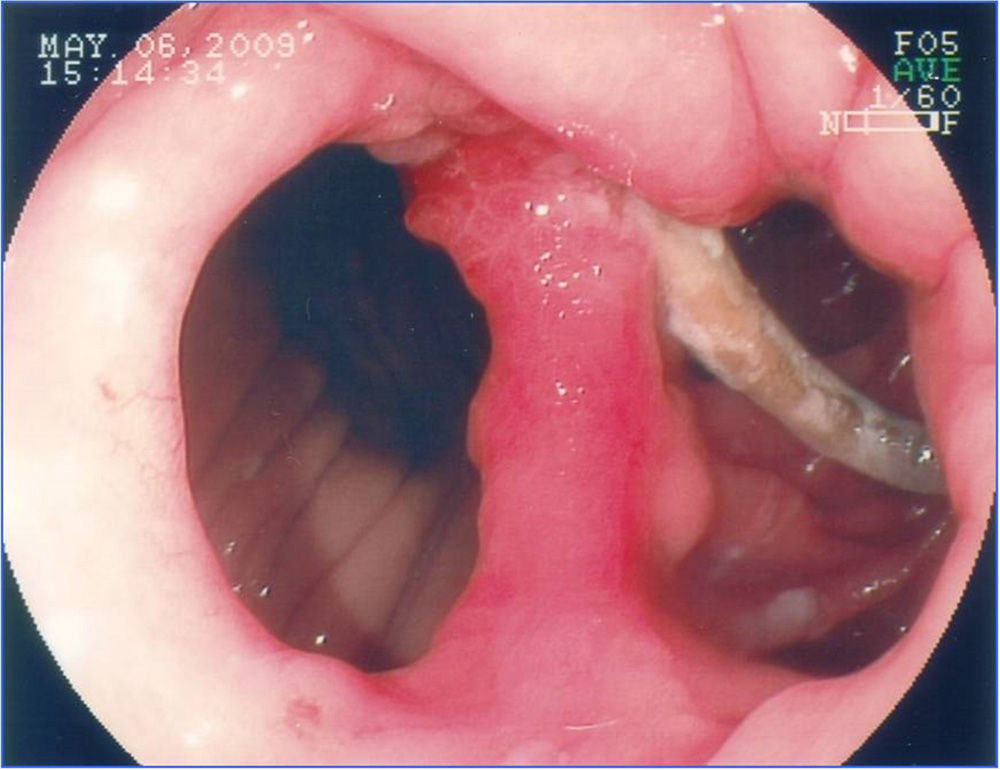
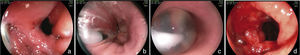
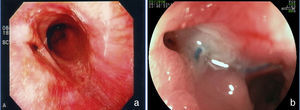
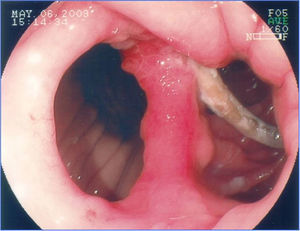
FistulasThe incidence of fistulas in bariatric surgery varies with the technique, the number of patients, and the period analyzed, and whether the case series describe endoscopic or surgical procedures. It was previously estimated from 0.4-26% of the cases21,49,81. However, thanks to surgical improvements, there was a significant decrease in this rate and fistulas are currently estimated to occur in 2.05-5.2% of patients after laparoscopic gastric bypass, in 1.68-2.60% after open bypass, and in 0.6-7% after vertical gastrectomy82–85. This incidence can reach up to 8% when the surgery is performed due to conversion from another technique59. It is one of the most serious complications and is the second cause of death from bariatric surgery, with a mortality rate of up to 1.5%86,87. Fistulas can be gastrocutaneous, internal (gastrogastric or gastroenteric) or they can be considered complex, affecting the gastric pouch and an adjacent or distant organ87. Gastrocutaneous fistula occurs after an early symptom of abdominal sepsis due to peritonitis or localized abscess and is treated with surgical intervention and/or drainage87. Clinical manifestation is late in the gastrogastric or gastrointestinal fistula, with inadequate weight loss or weight regain, epigastric pain (due to marginal ulcer), and reflux, but it can be subclinical, asymptomatic, and with satisfactory weight loss13. Endoscopy defines the presence of the fistulous orifice and characterizes it in relation to its location, size of the internal orifice, and the presence of a foreign body (suture thread) in the adjacent mucosa. Gastrocutaneous fistula occurs more commonly in the gastrojejunal anastomosis and in the upper portion of the suture line of the gastric pouch (bypass) or the gastric sleeve (gastrectomy), adjacent to the esophagogastric transition (fig. 9), most certainly due to a vascularization deficiency at that point14,87. We observed a wide communication in the internal fistula with the intestinal segment or with the excluded stomach (fig. 10). In the 2 locations, distal stricture can be diagnosed, related to the band and the anastomosis in the gastric bypass or excessive angulation at the final portion of the tunneled zone of the vertical gastrectomy. These are considered factors that predispose to and maintain fistulas86. Endoscopy can identify other alterations, such as internal migration of the band in the bypass, tortuosity and dilation of the tubular portion in the vertical gastrectomy, and the presence of mucosal septa adjacent to the fistulous orifice. Contrast-enhanced study of the fistula can be carried out to demonstrate and delimit the fistulous tract, diagnose the communication with other organs, diagnose complex fistulas, and especially, to evaluate emptying difficulty related to the strictures distal to the fistula13,19. Fistulas after bariatric surgeries are treated with nutritional support, suppression of gastrointestinal secretions, treatment of infection, and surgical excision of the fistulous orifice14. Endoscopy can help in these general measures with procedures such as the passage of a nasoenteric tube to enable nutrition, thus excluding transit in the region of the fistula, removal of foreign bodies in the region of the orifice, placement, traction, and repositioning of the drains or probes in the cavities and collections, and especially, treating eventual strictures distal to the fistula84. This type of treatment is of considerable value and enables closure of up to 85% of the fistulas88. Nevertheless, sometimes this approach can be delayed, expensive, or may not achieve the expected success. In such cases, endoscopic treatment specifically directed at the gastrocutaneous fistula that can lead to closure or contribute to a quicker resolution is suggested, reducing hospitalization and morbidity86. Fistula closure can require occlusion, not only of the fistulous orifice, but also of the entire tract. This has been attempted with the endoscopic injection of substances, such as biologic or synthetic glues, placement of an acellular matrix in the form of strips or cones on the tract or at the fistulous orifice, application of endoclips, and in special cases, the placement of self-expanding stents13,14,86. More commonly, a combination of techniques is employed. In order to indicate endoscopic fistula treatment, it is necessary to make sure that the fistula maintenance factor has been resolved, such as infection, foreign body, and distal obstruction. One of the endoscopic fistula treatment options after bariatric surgery is the placement of partially or totally covered self-expanding stents86,89. In the case of post-bariatric surgery fistulas, it is necessary to use special stents that can be removed90. Plastic stents were initially used, followed by metal ones89,90. The covered self-expanding stent forms a physical barrier between the fistula and the endoluminal content, favoring cicatrization, while enabling enteral nutrition91. Poli et al.92, reviewed 67 cases of fistulas after Roux-en-Y gastric bypasses, duodenal switch vertical gastrectomies, and banded vertical gastroplasties treated with stent placement. The results showed fistula closure in 87.7% of the cases, with a range between 79-94% (95% confidence interval). The time interval between stent placement and removal varied between one and 2 months in the majority of studies. Six of the 67 patients (9%) underwent surgical treatment after closure failure with the placement of up to two stents. There was stent migration in 16.9% of the cases, related to stent design or type of surgery and not to the endoscopic placement technique. Endoscopic removal of the stents was possible in almost 92% of the cases and the causes of failure were tissue hyperplasia and migration. There are reports on the difficulty of stent removal, with serious complications such as bleeding, removal in pieces, and even mucosectomy. There are cases of plastic stent placement inside the metallic stent to facilitate its removal93. Considering the difficulties and complications of removal, the migration rate, and the different anatomic details of the surgical techniques, it will be necessary to develop specific stents to be used in post-bariatric surgery fistulas86,91. Even though fistula treatment with stents appears promising, there are not yet enough controlled data to recommend their routine use14,90. These accessories should have differentiated size and caliber (adapted to the surgical anatomy), an anti-migration system, and a safe removal mechanism, or be biodegradable13,86,90. Finally, it appears that the tendency for endoscopy's role in relation to fistulas involves 2 situations: first, in the placement of stents in early cases93, and second, in the rigorous dilation of eventual distal strictures in the chronic cases19. In the cases of gastrointestinal and gastrogastric fistulas, classic treatment is surgical, and the morbidity and mortality can be two times higher than in the first surgery. Taking into account the problems of surgical re-operations, as well as fistula closure failure, endoscopic treatment is suggested. In the last few years, studies with small case series or case reports have shown the possibility of endoscopic suture of these defects, utilizing accessories such as the Endo-Cinch94, special clips (Ovesco)95, StomaphyX96, and Apollo OverStitch97, or the attempt to close the orifice utilizing a stent, biologic glue, debridement through argon plasma coagulation, and sometimes using a combination of two or more methods90. All the techniques have been shown to be feasible, although the durability of these endoscopic sutures needs further evaluation and long-term follow-up, especially in large communications between the pouch and the stomach and/or intestine86,90.
The incidence of biliary lithiasis after bariatric surgery is high, most certainly due to rapid weight loss98. Up to 36% of the patients develop cholecystolithiasis, generally within the first 6 postoperative months99. Approximately 30% of surgeons perform cholecystectomy during bariatric surgery in patients with a normal gallbladder19,100. Others regard this conduct as unjustifiable101. Considering the high incidence of biliary lithiasis in the patients operated on, when these patients present with symptoms and have laboratory and ultrasound studies suggestive of lithiasis, magnetic resonance cholangiography should be systematically carried out to make the diagnosis of choledocholithiasis that occurs in 4.7-7% of these patients11. The standard nonsurgical treatment for choledocholithiasis is through endoscopic cholangiography and papillotomy. This approach is limited in gastric bypass surgery because oral access is impossible. Some techniques have been proposed for performing endoscopic cholangiography and papillotomy after gastric bypass. This approach can be endoscopic or a combination of laparoscopy and endoscopy13,102. Solutions include balloon enteroscopy, percutaneous gastrostomy in the excluded stomach, or laparoscopic-assisted transgastric endoscopic access103–107. There is an 84% success rate using enteroscopy19,106,107. The disadvantages of this method are the lack of accessories with a length compatible with the enteroscope, the lack of an elevator, and frontal vision limitations of the endoscope for biliopancreatic therapy19. Percutaneous gastrostomy, performed through radiologic methods or at the time of bariatric surgery, offers multiple access possibilities, but requires time to mature and produces some discomfort since it cannot be rapidly removed102. Among the options, laparoscopy-assisted transgastric endoscopic cholangiography and papillotomy has been reported as the best option. It has a high success rate and is a low-risk procedure, especially in cholecystectomized patients. This technique is safe, reproducible, utilizes known and available equipment and accessories, and standardized laparoscopic and endoscopic techniques102,104,105. If the patient presents with cholecystolithiasis and choledocolithiasis in the postoperative period, the surgeon should perform cholecystectomy and can treat the choledocolithiasis through surgery or the combined approach of cholecystectomy plus the creation of a transgastric access for endoscopic papillotomy11,12. There are technical variations in this method that include the manner in which the surgeon prepares and performs the access to the stomach (using sutures, a trocar, or another tube) and how the endoscopist passes and positions the duodenoscope (directly or guided by the surgeon)102.
The excluded stomach in gastric bypassThe excluded stomach in gastric bypass surgery cannot be examined through the usual endoscopic or radiographic techniques108. Gastroduodenoscopy, using a pediatric colonoscope, introduced in a retrograde manner through the jejunal segment to the excluded segment was successfully performed in 86% of 77 attempts109. However, it appears to us that this technique is only possible in selected cases when a gastrojejunostomy is used for reconstruction and in the cases of short Roux-en-Y with ample enteroenteric latero-lateral anastomosis. The method of access through a long segment is at present practically impossible. Some studies have reported on successful and safe access to the excluded stomach through the use of the balloon enteroscope (simple or double)110,111. Indications for this method vary and include epigastric pain, anemia, excessive weight loss, active bleeding, and occult bleeding. In an analysis of 12 patients with occult bleeding and anatomy altered by Roux-en-Y, 6 for gastric bypass, the main findings were ulcer of the anastomosis, peri-anastomotic neovascularization, and Dieulafoy's lesion112. In contrast, in another case series of enteroscopy in 35 patients with Roux-en-Y, but indicated due to epigastric pain, the predominant findings were erosions and ulcers in the stomach in 35% of the patients and few diagnoses of ulcers and peri-anastomotic neovascularization113. One patient with gastric bypass for 10 years presented with melena and severe anemia and the examination of the Roux-en-Y excluded stomach through double balloon endoscopy revealed severe hemorrhagic erosive pangastritis that was adequately treated with high doses of proton pump inhibitors114. Some case series, in which examination of the excluded stomach was possible, reported superficial chronic gastritis in 87% of patients that was histologically confirmed in 42%, with 10% presenting with intestinal metaplasia; the meaning of these findings was not clear110,111. Acid production was lower than in the normal population and H. pylori was negative in 70% of the cases, suggesting that the excluded stomach is less ulcerogenic108. Nevertheless, peptic ulcer can occur in the excluded stomach, including perforation or bleeding, with an incidence under 0.3%113,115. The average time between surgery and a hemorrhagic episode is a mean of 9.5 years. There are reports in a literature review of five cases of gastric cancer in a gastric bypass excluded stomach, one case 13 years after the surgery, three cases 9 years after the surgery, and one case 5 years after the surgery116. It has an extremely low incidence, considering the large number of bariatric surgeries performed. Thus it is estimated that less than 1% of patients have a real necessity for endoscopic study of the excluded stomach108,109.
FundingThere was no source of funding.
Conflict of interestThe authors declare that they have no conflict of interests.
Please cite this article as: da Rocha LCM, Ayub Pérez OA, Arantes V. Manejo endoscópico de las complicaciones en la cirugía bariátrica: lo que el gastroenterólogo debe saber. Revista de Gastroenterología de México. 2016;81:35–47.