A submucosal lesion (SML) is a “bulging” covered with normal mucosa found during endoscopy. In general, they are asymptomatic lesions and are considered benign if they are < 2cm. Conventional management is periodic surveillance and these lesions should be resected only if they begin to grow or cause symptoms.1 However, there is a risk for malignancy, regardless of size, depending on their histology. Endoscopic ultrasound (EUS) enables the evaluation of their origin with 100% accuracy2 and has a 78-91% sensitivity in relation to biopsy.3 Thus, surveillance would cause a delay in diagnosing the malignancy of some SMLs, along with stress for the patients, resulting in a greater need for resection.4
Resection can be surgical (thoracoscopy or laparoscopy)5 or endoscopic (ligature, dissection, total endoscopic resection).6 Surgery implies longer hospital stay and is more expensive than endoscopy, but endoscopy can present with a greater number of complications (perforation, incomplete resection).7
In 2010 peroral endoscopic myotomy was developed;8 this technique enables dissection of the muscularis propria of the esophagus in patients with achalasia through a submucosal tunnel with excellent results and minor complications. Recent reports have described good results with this method in the resection of SMLs.9,10 Our aim was to communicate the use of this technique in the resection of a giant esophageal SML.
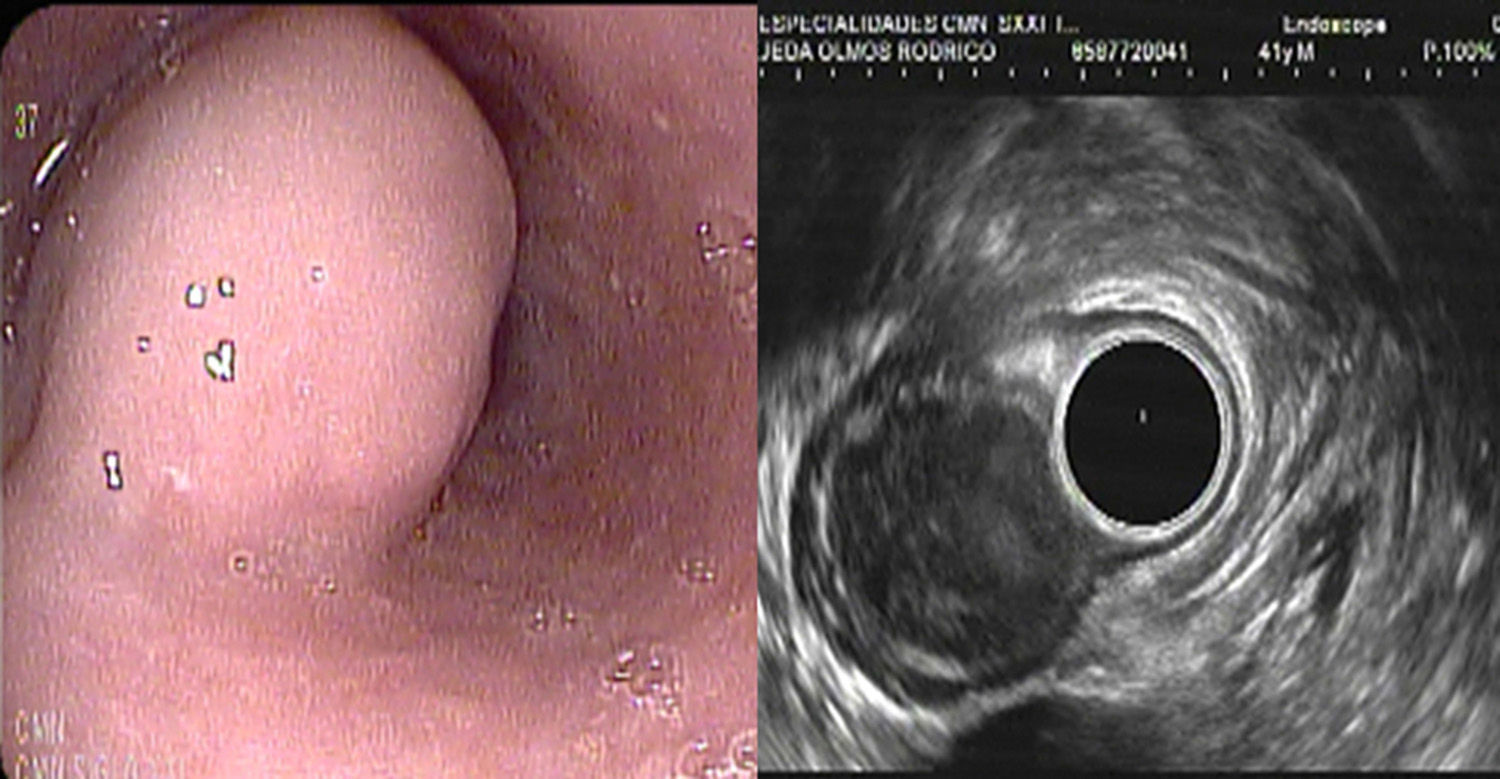
A healthy 45-year-old man sought medical attention for dysphagia of 6-month progression. Endoscopy revealed a 2cm SML in the distal esophagus that took up 80% of the lumen. EUS identified a well-defined 21 x 25mm hypoechogenic lesion that was dependent on the muscularis propria with no data suggestive of malignancy. Aspiration puncture was negative. Lesion resection with the submucosal tunnel method was decided upon, the patient signed a statement of informed consent, and the procedure was approved by the hospital ethics committee.
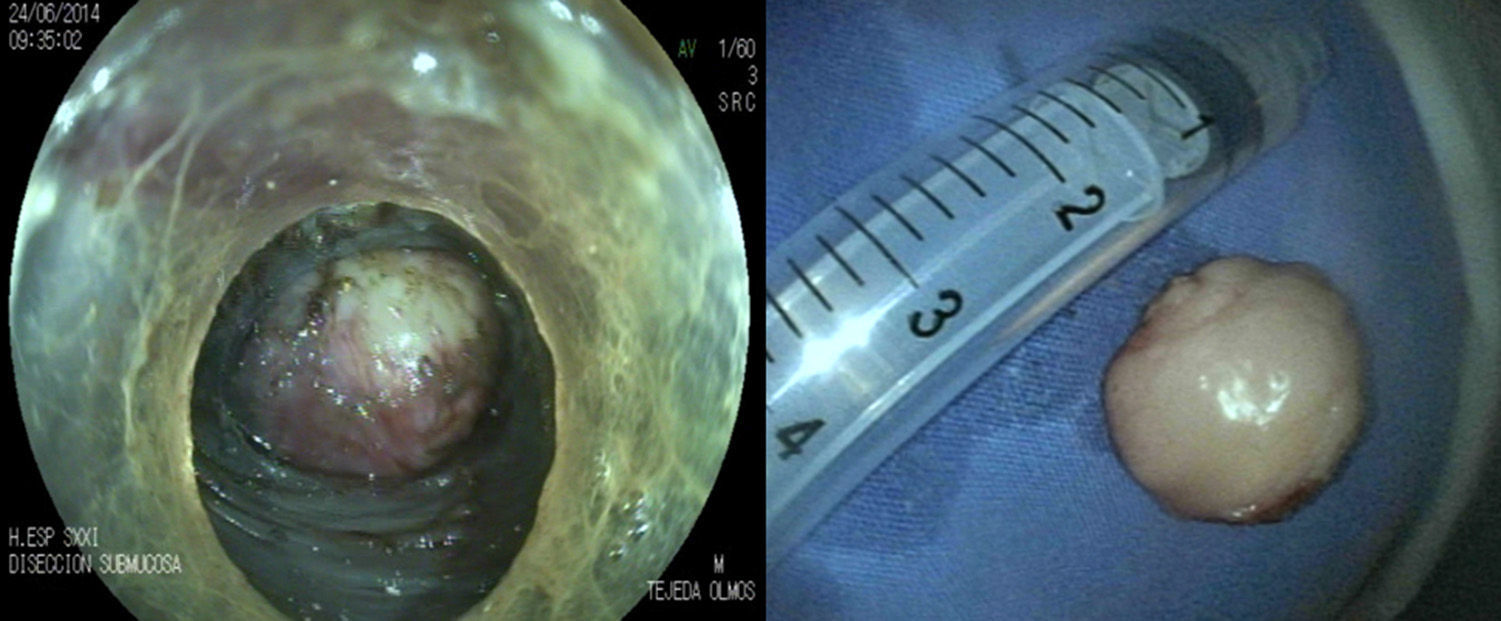
The patient was hospitalized, put in a fasting state, and given intravenous antibiotics. We used the following materials: a model EG590WR endoscope (Fujinon, Tokyo, Japan), a model DH-28GR transparent hood (Fujinon, Tokyo, Japan), and ERBE VIO Model 300D electrosurgical equipment (Tübingen, Germany) used in the coagulation spray mode (2 to 50W endocut effect) for the incision and tunnel creation; the tumor was resected with a 3 to 40W endocut effect, using a BT 2.0 flush knife (Fujinon, Tokyo, Japan) and resolution clips (Boston Scientific, USA). The incision was begun at 10cm proximal to the lesion, injecting a 10 cc solution of 0.3% carmine indigo combined with adrenaline at 1:10,000. A 20mm longitudinal incision was made. The submucosal tunnel was created through dissection up to the lesion that was dependent on the muscularis propria, which was then dissected (fig. 1).
The dissection was completed, the specimen was extracted, and closure was performed with hemoclips. The patient remained fasting for 48h. Chest x-ray and water-soluble contrast swallow were normal, the patient began to eat a regular diet, and he was released on the 5th postoperative day with no complications. The final histologic diagnosis was a 25 x 28mm leiomyoma that was resected en bloc (fig. 2).
The present case demonstrated complete resection of a giant esophageal SML through this new method. Despite the size of the SML, its origin (muscularis propria), and the technical difficulty, there were no late complications and hospital stay was short. The main advantages of this technique are the different entrance and resection sites, represented by the “submucosal tunnel”, a safety space that separates them; even in the case of incidental perforation, the entrance site can be closed with hemoclips, avoiding contact with the contents of the esophageal lumen, thus reducing or preventing the complications characteristic of a perforation (mediastinitis). Finally, complete lesion resection results in the correct clinical behavior based on lesion histology. Nevertheless, further studies with a larger number of patients are needed to determine the place this technique will hold in relation to SML treatment.
Financial disclosureNo financial support was received in relation to this study.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Hernández-Mondragón OV, Blancas-Valencia JM, Altamirano-Castañeda ML. Resección endoscópica de leiomioma esofágico gigante por técnica de tunelización. Revista de Gastroenterología de México. 2015;80:167–168.