The prevalence of functional gastrointestinal disorders (FGIDs) in Argentinean children and adolescents has not yet been studied. Our aim was to determine the prevalence of FGIDs among children and adolescents in Argentina using the Rome III diagnostic criteria.
Materials and methodsA total of 483 children, 12-18 years of age, from 3 private schools and 3 public schools, were included in the study. Each child completed the Spanish version of the Questionnaire on Pediatric Gastrointestinal Symptoms-Rome III), which is an age-appropriate and previously validated instrument for diagnosing FGIDs according to the Rome III criteria. Sociodemographic data (age, sex, type of school, family structure and size, family history of gastrointestinal disorders) and data on stressful life events were also obtained.
ResultsThe mean age of the population studied was 15 years (standard deviation 1.74, range 12-18, 52.8% boys). Of the respondents, 229 children (47.4%) attended private school and 254 children (52.6%) attended public school. In total, 82 children (17.0%) were diagnosed with an FGID, according to the Rome III criteria. Abdominal migraine (16.4%) was the most common diagnosis, followed by irritable bowel syndrome (7.0%), functional constipation (6.4%), and aerophagia (5.6%). Girls suffered significantly more from FGIDs than boys (22.4 vs. 12.2%, P=.0032). Children attending private school had significantly more FGIDs than children in public schools (20.5 vs. 13.8%, P=.0499).
ConclusionFGIDs are common among Argentinean children and adolescents.
La prevalencia de los trastornos funcionales digestivos (TFD) en niños y adolescentes argentinos no ha sido estudiada aun. El objetivo fue determinar la prevalencia de los TFD entre niños y adolescentes argentinos utilizando los criterios de diagnóstico de Roma III.
Materiales y métodosSe incluyó a un total de 483 niños de entre 12 y 18 años de edad, reclutados de 3 escuelas privadas y 3 escuelas públicas. Cada niño completó el Cuestionario Pediátrico de Síntomas Gastrointestinales-Roma III en su versión en español, el cual es un instrumento adecuado para esa edad y que ha sido previamente validado para diagnosticar los TFD de acuerdo a los criterios de Roma III. También se obtuvieron datos sociodemográficos (edad, sexo, tipo de escuela, estructura y tamaño de la familia, historia familiar de enfermedades gastrointestinales) y datos sobre eventos estresantes de la vida.
ResultadosLa edad promedio de la población estudiada fue de 15 años de edad (desviación estándar de 1.74, rango de 12-18, el 52.8% varones). Doscientos veintinueve de los 483 niños (47.4%) fueron estudiantes de escuelas privadas y 254 (52.6%) de escuelas públicas. En total, 82 niños fueron diagnosticados con un TFD de acuerdo a los criterios de Roma III. La migraña abdominal fue el diagnóstico más común (16.4%), seguido del síndrome de intestino irritable (7%), estreñimiento funcional (6.4%), y aerofagia (5.6%). Los TFD fueron significativamente más frecuentes en niñas que en niños (22.4 vs. 12.2%, p=0.0032). Con relación al tipo de escuela, el porcentaje de los TFD fue mayor en los niños de escuelas privadas que en los de escuelas públicas (20.5 vs. 13.8%, p=0.0499), con diferencia estadísticamente significativa.
ConclusiónLos TFD son comunes entre los niños y adolescentes argentinos.
Functional gastrointestinal disorders (FGIDs) are common in children worldwide and are characterized by the absence of an identifiable underlying structural, infectious, inflammatory, or biochemical abnormality.1,2 Symptoms related to FGIDs are often chronic, recurrent, and frequently disabling, leading to poor health and functional impairments, such as sleep disturbance, school absenteeism, poor school performance, and compromised social development.3–5 Moreover, it has been reported that psychological disorders, such as anxiety and depressive disorders, frequently occur concomitantly with FGIDs in both adults and children.6
FGIDs are diagnosed according to the Rome criteria. Those symptom-based criteria were created by a group of experts in the field of pediatric gastroenterology, based on available evidence and a consensus process.1 Since 2006, the Rome III criteria have been used for that purpose.7 Those criteria were updated in 2016, becoming the Rome IV criteria.8
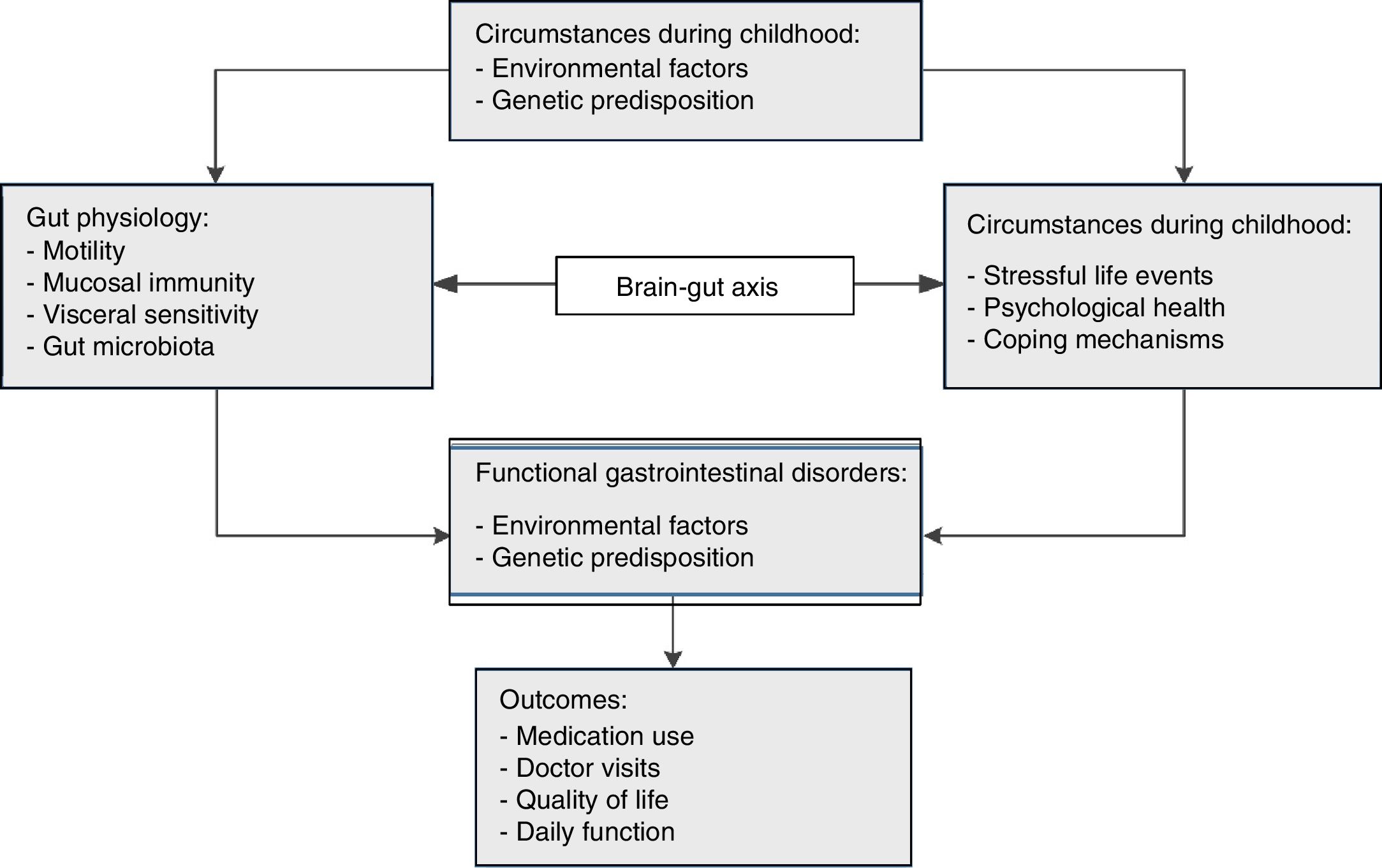
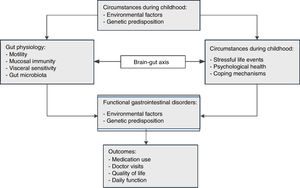
The pathogenesis of FGIDs is currently considered to be based on a biopsychosocial model, which links the clinical expression of FGIDs to genetic and physiologic determinants that, in turn, are influenced by sociocultural, environmental, and psychological factors.7 Predisposing factors for abdominal pain-related FGIDs include genetic variations, psychological stress, child maltreatment, and gastrointestinal infections.3 The expressions of FGIDs may vary, depending on individual susceptibility to stress, psychological condition, and coping skills, as well as other predisposing factors (fig. 1).
The reported prevalence of FGIDs, according to the Rome III criteria, varies between 13.9 and 23.1% among children and adolescents.9–11 In children, the most prevalent FGIDs are irritable bowel syndrome (IBS) and functional constipation, with reported worldwide prevalence rates between 2.8-25.7% and 0.7-29.6%, respectively.12,13 Those data indicate that FGIDs are common across the globe, but that prevalence may vary among races, cultures, and geographic areas.7 Apart from environmental and cultural differences, Argentina has a different ethnic background, compared with other South American countries. Whereas most Argentineans are of colonial European descent, the populations of the other continental South American countries have predominantly mestizo and mulatto ancestries. Uruguay and Chile are exceptions, with more mixed populations. Taking those distinctions into account, Argentina could have a different FGID prevalence rate, compared with the other countries in the region.
To improve awareness, diagnosis, and treatment of FGIDs, it is necessary to understand those regional differences in prevalence and to identify the underlying factors that are potentially responsible for them. Therefore, the aim of the present study was to assess the prevalence of FGIDs among Argentinean children and adolescents. As a secondary outcome measure, we studied the association between FGIDs and personal and socioeconomic life stressors.
Materials and methodsWe performed a cross-sectional survey study to assess the prevalence of FGIDs in Argentinean adolescents, according to the Rome III criteria. Data were collected at high schools between July and September 2015 in the province of Buenos Aires, Argentina. Buenos Aires is the most densely populated province in the country and is a destination for migrant workers from the neighboring countries of Uruguay, Peru, Chile, and Paraguay, resulting in a culturally diverse population. A list of all the schools in the greater metropolitan area of Buenos Aires was drafted. To ensure a socioeconomically diverse sample, both private and public schools in the inner city and suburban areas were selected as study sites. A member of the research team contacted all the schools, explaining the purpose of the study and inviting them to participate. Three private schools and 3 public schools were randomly chosen from the schools interested in taking part in the study.
Children between 12 and 18 years of age were given a leaflet with information about the study and a consent form to be given to their parents or guardians. All the children that presented a signed statement of informed consent on the day of the survey participated in the study. The questionnaires were completed during class periods under teacher supervision, and a researcher was present to clarify any questions about vocabulary used in the questionnaires or about test dynamics. Given the personal nature of some of the questions, and to ensure the complete anonymity of the questionnaires, they were completed in an examination setting.
We applied the Questionnaire on Pediatric Gastrointestinal Symptoms Rome III Version (QPGS-RIII), a validated questionnaire designed to diagnose FGIDs in children, based on the Rome III criteria.14 Its questions are on gastrointestinal symptom location, frequency, and severity, as well as related disability and somatic symptoms. The QPGS-RIII questionnaire employed was a previously validated translation from English to Spanish.15,16
Because an association between stress and FGID onset was suspected, a tool for measuring perceived stress was created solely for that purpose. The survey contained several questions about the presence of life stressors that could possibly generate stress among children. Those questions were divided into 3 separate parts within the questionnaire. The first part consisted of questions about the presence of stressful life events within the last 3 months, such as parental divorce, a death in the family, or a parent losing his or her job. The second part contained questions about mental abuse on the part of parents, acquaintances, or peers at any point in the study participant's life. The third and final part included questions on whether the study participant had ever been subjected to any form of physical violence.
Minimal sample size was calculated using Slovin's formula.17 There are no data on the prevalence of FGIDs in Argentina, so an expected prevalence of 29%, found by Saps et al. in Colombia in 2014, was used.18 With a 95% confidence interval, a 5% degree of absolute precision, a standard normal deviation of 1.96, and an attrition rate of 20%, the minimal sample size of 396 was determined. The Pearson's chi-square test was used to calculate the presence of statistically significant factors on the development of FGIDs.
Ethical approval for the study was obtained from the Argentinean State Health Research Ethics Committee and the respective school authorities.
ResultsThe questionnaire was distributed to 562 children. After reviewing the completed questionnaires, 79 (14.1%) were discarded because the age of the child did not match the inclusion criteria or because the child did not answer questions on sex, school type, or whether he or she suffered from stomach pain.
After excluding those children, the total study population was 483, made up of 255 boys (52.8%) and 228 girls (47.2%). Of the respondents, 229 children (47.4%) attended private school and 254 children (52.6%) attended public school. Participants had a mean age of 15.0 years (standard deviation 1.74, range 12-18).
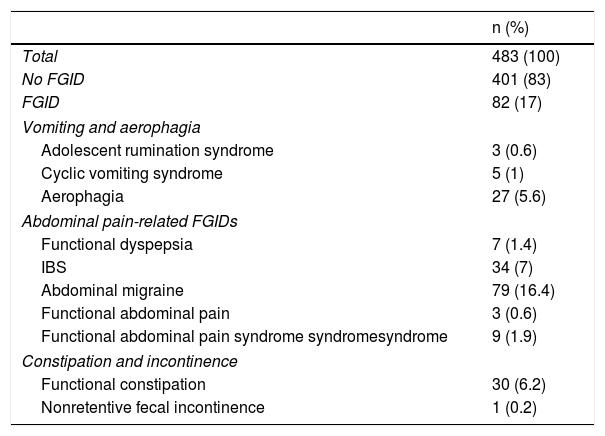
In total, 82 children (17.0%) were diagnosed with an FGID, according to the Rome III criteria (Table 1). Abdominal migraine (16.4%) was the most common diagnosis, followed by IBS (7.0%), functional constipation (6.2%), and aerophagia (5.6%). Functional nonretentive fecal incontinence was diagnosed in only one child (0.6%).
FGID prevalence.
| n (%) | |
|---|---|
| Total | 483 (100) |
| No FGID | 401 (83) |
| FGID | 82 (17) |
| Vomiting and aerophagia | |
| Adolescent rumination syndrome | 3 (0.6) |
| Cyclic vomiting syndrome | 5 (1) |
| Aerophagia | 27 (5.6) |
| Abdominal pain-related FGIDs | |
| Functional dyspepsia | 7 (1.4) |
| IBS | 34 (7) |
| Abdominal migraine | 79 (16.4) |
| Functional abdominal pain | 3 (0.6) |
| Functional abdominal pain syndrome syndromesyndrome | 9 (1.9) |
| Constipation and incontinence | |
| Functional constipation | 30 (6.2) |
| Nonretentive fecal incontinence | 1 (0.2) |
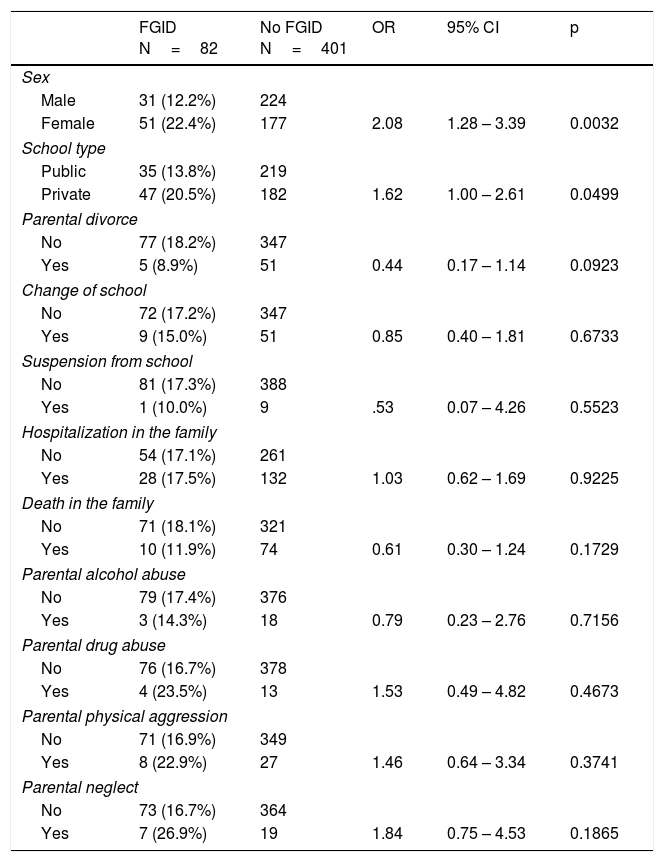
Sex, school type, and family structure were compared in children with and without FGIDs (Table 2). The chi-square tests were used to calculate whether there was a relationship between those demographic factors and the prevalence of FGIDs. The prevalence of FGIDs was significantly higher among girls than among boys: 22.4 vs 12.2% (OR 2.08; p=0.0032). The prevalence of FGIDs was also significantly higher among children that attended private school, compared with children that attended public school: 20.5 vs 13.8%, respectively (OR 1.62; p=0.0499) (Table 2).
Comparison of characteristics between children with and without FGIDs.
| FGID N=82 | No FGID N=401 | OR | 95% CI | p | |
|---|---|---|---|---|---|
| Sex | |||||
| Male | 31 (12.2%) | 224 | |||
| Female | 51 (22.4%) | 177 | 2.08 | 1.28 – 3.39 | 0.0032 |
| School type | |||||
| Public | 35 (13.8%) | 219 | |||
| Private | 47 (20.5%) | 182 | 1.62 | 1.00 – 2.61 | 0.0499 |
| Parental divorce | |||||
| No | 77 (18.2%) | 347 | |||
| Yes | 5 (8.9%) | 51 | 0.44 | 0.17 – 1.14 | 0.0923 |
| Change of school | |||||
| No | 72 (17.2%) | 347 | |||
| Yes | 9 (15.0%) | 51 | 0.85 | 0.40 – 1.81 | 0.6733 |
| Suspension from school | |||||
| No | 81 (17.3%) | 388 | |||
| Yes | 1 (10.0%) | 9 | .53 | 0.07 – 4.26 | 0.5523 |
| Hospitalization in the family | |||||
| No | 54 (17.1%) | 261 | |||
| Yes | 28 (17.5%) | 132 | 1.03 | 0.62 – 1.69 | 0.9225 |
| Death in the family | |||||
| No | 71 (18.1%) | 321 | |||
| Yes | 10 (11.9%) | 74 | 0.61 | 0.30 – 1.24 | 0.1729 |
| Parental alcohol abuse | |||||
| No | 79 (17.4%) | 376 | |||
| Yes | 3 (14.3%) | 18 | 0.79 | 0.23 – 2.76 | 0.7156 |
| Parental drug abuse | |||||
| No | 76 (16.7%) | 378 | |||
| Yes | 4 (23.5%) | 13 | 1.53 | 0.49 – 4.82 | 0.4673 |
| Parental physical aggression | |||||
| No | 71 (16.9%) | 349 | |||
| Yes | 8 (22.9%) | 27 | 1.46 | 0.64 – 3.34 | 0.3741 |
| Parental neglect | |||||
| No | 73 (16.7%) | 364 | |||
| Yes | 7 (26.9%) | 19 | 1.84 | 0.75 – 4.53 | 0.1865 |
Out of 82 children with FGIDs, 25 (30.5%) had 2 or more FGIDs. Twenty-one children had 2 FGIDs: 7 fulfilled the criteria for abdominal migraine in combination with IBS; 4 children had abdominal migraine and functional constipation; 3 were diagnosed with abdominal migraine and aerophagia; 2 were diagnosed with abdominal migraine and functional dyspepsia; one child had functional abdominal pain syndrome in combination with aerophagia; one child had IBS and nonretentive fecal incontinence; one child had functional constipation and functional abdominal pain; one child had functional abdominal pain and aerophagia; and one child had cyclic vomiting syndrome and IBS. Four children had 3 FGIDs: 3 children had aerophagia, abdominal migraine, and IBS; the other child had adolescent rumination syndrome, functional constipation, and abdominal migraine.
To investigate a possible relationship between stress and FGID onset, the questionnaire contained several questions on situations and events that could generate stress among children. The statistical analysis did not reveal any significant differences in the prevalence of FGIDs with respect to those variables, some of which are shown in Table 2.
Discussion and conclusionTo the best of our knowledge, this is the first study to assess the prevalence of FGIDs in Argentinean adolescents using the internationally accepted Rome criteria. In our sample, we found a prevalence of FGIDs of 17.0%. Unlike previous studies, abdominal migraine was the most common FGID with a prevalence rate of 16.4%.18–21 In addition, girls suffered from FGIDs significantly more than boys. Our data also showed that children attending private school had significantly more FGIDs than children in public school. Contrary to our hypothesis, an association between life stressors and FGIDs was not found.
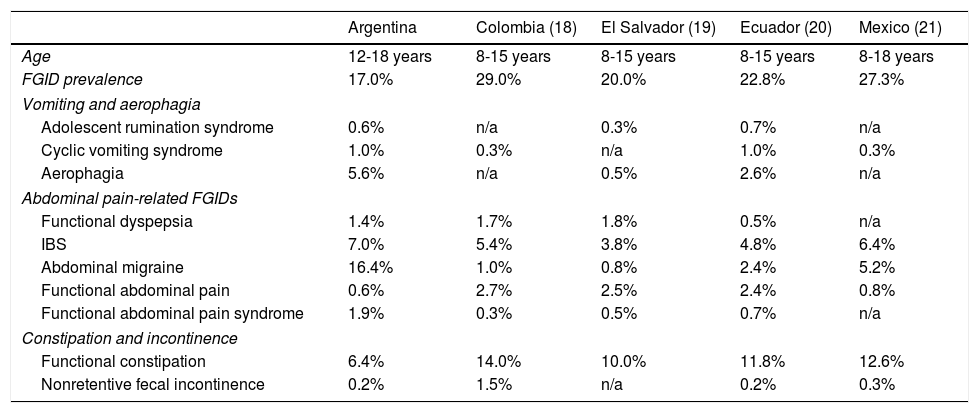
Similar studies evaluating the prevalence of FGIDs, using the same questionnaire, have been conducted in other countries in South America and Central America, such as Colombia, Ecuador, Panama, and El Salvador, as well as in Mexico.18,20–22 Differences in prevalence between the present study and those previously published studies are shown in Table 3.
Comparison of prevalence rates found in similar studies.
| Argentina | Colombia (18) | El Salvador (19) | Ecuador (20) | Mexico (21) | |
|---|---|---|---|---|---|
| Age | 12-18 years | 8-15 years | 8-15 years | 8-15 years | 8-18 years |
| FGID prevalence | 17.0% | 29.0% | 20.0% | 22.8% | 27.3% |
| Vomiting and aerophagia | |||||
| Adolescent rumination syndrome | 0.6% | n/a | 0.3% | 0.7% | n/a |
| Cyclic vomiting syndrome | 1.0% | 0.3% | n/a | 1.0% | 0.3% |
| Aerophagia | 5.6% | n/a | 0.5% | 2.6% | n/a |
| Abdominal pain-related FGIDs | |||||
| Functional dyspepsia | 1.4% | 1.7% | 1.8% | 0.5% | n/a |
| IBS | 7.0% | 5.4% | 3.8% | 4.8% | 6.4% |
| Abdominal migraine | 16.4% | 1.0% | 0.8% | 2.4% | 5.2% |
| Functional abdominal pain | 0.6% | 2.7% | 2.5% | 2.4% | 0.8% |
| Functional abdominal pain syndrome | 1.9% | 0.3% | 0.5% | 0.7% | n/a |
| Constipation and incontinence | |||||
| Functional constipation | 6.4% | 14.0% | 10.0% | 11.8% | 12.6% |
| Nonretentive fecal incontinence | 0.2% | 1.5% | n/a | 0.2% | 0.3% |
In agreement with the Colombian study, we found a higher prevalence of FGIDs in girls.18 That finding coincides with higher rates of FGIDs in women in several adult studies regarding FGID prevalence in different populations.9,23 Those differences may be related to hormonal differences between men and women. To support that hypothesis, Chang et al. found differences in gastrointestinal sensitivity and physiological response to visceral stimuli between men and women in IBS, which could explain a higher prevalence rate in women with IBS.23 Remarkably, that difference in FGID prevalence between the sexes was not supported by the studies previously conducted in Mexico, El Salvador, and Ecuador.19–21 That discrepancy could be related to the fact that different age groups were evaluated in the studies. We investigated children and adolescents with an age range of 12 to 18 years, with a mean age of 15 years. The studies conducted in Mexico, Ecuador, and El Salvador were carried out on children with a different age range, including children as young as 8 years old, resulting in a younger mean age of the study population: 11.6, 11.8, and 12.0 years, respectively.19–21 The effect of the abovementioned hormonal differences could be of less relevance in those younger populations, given that a sizable part of the girls analyzed were premenarcheal.
Our results show that children attending private school had a significantly higher risk for being diagnosed with an FGID than children attending public school, which could possibly be explained by the difference in lifestyle and diet that comes with a higher socioeconomic status in developing countries. In Argentina, only a small percentage of children from affluent families attend private schools, which are considerably more expensive than the free public schools. It has been suggested that in developing countries such as Argentina, people with a higher socioeconomic status are the first to shift to a Western diet, with a low fiber count and a higher fat and sugar intake, and to a more sedentary lifestyle.24 An association between several FGIDs and a Western diet has been suggested in the literature.25–29 A second possible explanation for that finding is the difference in attitude towards a child's health. According to Levy et al., families that are overly solicitous to a child's illness may amplify symptoms and illness behaviors.30 It could well be the case that parents of children growing up under less favorable economic conditions are more likely to work multiple jobs and be consumed by pressing economic matters, and so they cannot spend as much time caring for what is perceived as a non-life-threatening disease. Moreover, high quality healthcare may be less easily accessible to families of lower economic means. Conversely, mothers that are less likely to work, may be able to seek prompt medical care in private clinics for their child's functional health problems.
As illustrated by Drossman, the pathophysiology of FGIDs is multifactorial and a correlation exists between one's susceptibility to life stress and functional GI symptoms and clinical outcome.7 Taking that into account, it was expected that life stressors and events would lead to significant differences in FGID prevalence with respect to such variables. To examine that, the questionnaire contained items about events or situations that were expected to generate stress among children. To our surprise, none of the questions posed were associated with a significantly higher prevalence of FGIDs. The fact that the questionnaire measured life stressors, and not the amount of stress perceived by each subject, could be a possible explanation for that finding. By simplifying something as complicated as stress to the presence of one or several life stressors, without taking into account the child's coping skills and the many factors involved in whether or not the event or situation is considered as stressful by the subject, may lead to unreliable results.
Even though no relationship was found between life stressors and FGIDs, that does not disprove a relation between perceived stress and FGIDs. Moreover, we used a non-validated tool to measure stress, which may have influenced our results.
In the data analyses, we assumed that the effect of multiple stressors was cumulative. Initially, we divided the subjects into 2 groups: children that had experienced up to 2 life stressors, and children that had experienced three or more life stressors. We decided not to pursue that form of measurement. First of all, because the questions that were asked varied significantly, in relation to gravitas. For example, one of the questions was about failing an exam, whereas another was about the occurrence of a death in the family. Secondly, children, like all people, cope with stressors very differently. What can be a huge cause of stress for one child (failing an exam) can be completely irrelevant to another. Therefore, it was unreliable to add up those factors as if they had the same weight for each child.
Interestingly, we found a very high prevalence of abdominal migraine in the present analysis, and it was within the range of that reported in other studies. A study by Baber et al. found a prevalence of abdominal migraine of 23.1%, applying the Rome III criteria in a cohort of children in the US.31 However, Saps et al. found a prevalence rate of 1% in their study on Colombian schoolchildren.18 Because abdominal migraine is not commonly encountered in clinical practice, that finding should be interpreted with caution. The high prevalence rate of abdominal migraine in our study could be related to the fact that the questions on the QPGS-RIII for that disorder may be nonspecific. Such a situation was described in a study showing that, compared with diagnoses by expert pediatric gastroenterologists, a large number of children presenting with an abdominal pain-predominant FGID, were misclassified as having abdominal migraine using the QPGS-RIII.32 For example, children suffering from 2 episodes of gastroenteritis within 12 months could mistakenly be thought to fulfill the Rome III criteria if they had severe abdominal pain for one hour or more that interfered with daily activities and was associated with nausea and vomiting. Furthermore, the Rome III criteria state that there should be no evidence of an inflammatory, anatomic, metabolic, or neoplastic process explaining the subject's symptoms, but that criterion is not easily answered by a child through a questionnaire and may lead to bias. Thus, the overall prevalence of FGIDs can be overestimated.33 Mindful of that potential problem, the Rome IV committee has modified the diagnostic criteria for abdominal migraine.8
In the present study, the second most prevalent FGID was IBS, which was diagnosed in 7.0% of our study population. That rate is comparable to those of school studies conducted in other South American countries using the Rome III criteria (Table 2). The similarity in findings among children of different geographic location, ethnicity, culture, climate, and environment is interesting and worth studying further.
One of the essential criteria for the diagnosis of FGIDs according to the Rome III system is the absence of evidence of organic diseases that could explain the child's symptoms. Limitations of our research include the lack of information on the medical status of the respondents, as well as of a thorough physical examination. However, the fact that organic gastrointestinal disorders are not common in that age group, with a prevalence rate of less than 1%, makes it an unlikely influence on our results.34 Even though our study population was comparable to that of a number of other population-based studies on pediatric FGID prevalence, the number of children with FGIDs was still low and a larger sample size would increase the reliability of our results. Furthermore, we selected a specific sample of children in Buenos Aires, and the results may not be representative of the rest of Argentina. Finally, prior studies have shown that the prevalence of FGIDs is affected by seasonal variation.35,36 Buenos Aires has a climate with distinct seasons and the data were only collected in August and September, during winter. Conducting the same study at a different season could lead to different results.
In conclusion, we found a high prevalence of FGIDs in children and adolescents living in Buenos Aires, Argentina. In our population, 17% of the schoolchildren fulfilled the criteria for at least one FGID. Abdominal migraine was the most common FGID, although we suspect that the number of cases was an overestimation. In our population, we found that children attending private school had significantly more FGIDs than children in public school. Our results also showed that girls suffered significantly more from FGIDs than boys. Those results are comparable to previously published data from similar studies conducted in other South American countries.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureNo financial support was received in relation to this study/article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Nelissen LG, Koppen IJN, Follett FR, Boggio-Marzet C, Saps M, Garzon K, Benninga MA. Prevalencia de los trastornos funcionales digestivos entre los adolescentes de Buenos Aires, Argentina. Revista de Gastroenterología de México. 2018;83:367–74.
See related content at DOI: https:// 10.1016/j.rgmxen.2018.06.011, Velasco-Benítez CA. Functional gastrointestinal disorders in Latin American adolescents: From Argentina to Mexico. Rev Gastroenterol Méx. 2018;83:365–6.