Extraction can turn out to be complex in 15-20% of choledochal stones due to size (> 15mm), number (≥ 3), or the container-content dissociations determining impactions.1,2 Under these adverse circumstances, other endoscopic techniques should be applied: large-volume balloon dilation or mechanical, laser, or electrohydraulic lithotripsy.3–5 If therapeutic success is not achieved, the placement of plastic biliary stents is employed as a bridge until definitive intervention. Over the last decade, the useof self-expanding metal stents in the context of benign biliary pathology has increased, but their role in treating biliary stones has not been described.6–8We present herein the case of complex bile duct stones resolved through the placement of a removable metallic biliary stent.
A 59-year-old woman had a past medical history of cholecystectomy and severe aortic stenosis. She sought medical attention for intense epigastric pain irradiating to the upper right quadrant and back,accompanied with jaundice and choluria of 15-day progression. A liver function test showed cholestasis and abdominal ultrasound revealed dilated intrahepatic and extrahepatic bile ducts with a 20mm stone in the retropancreatic part of thebile duct.
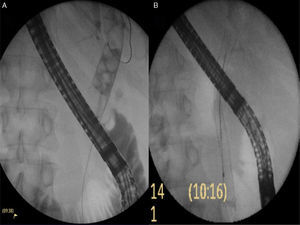
She underwent endoscopic retrograde cholangiopancreatography that revealed dilated bile ducts with multiple giant stones, one of which was square-shaped (> 20mm)and impacted in the middle bile duct (fig. 1).
Ample sphincteropapillotomy was performed with sequential dilation using a large balloon until reaching a diameter of 15mm.
A mechanical lithotripsy basket was introduced that did not open completely and the stone was unable to be retrieved.
The decision was made to place a totally covered 10mm x 80mm metal stent (WallFlex® Biliary, Boston Scientific, MA, USA) (fig. 1).
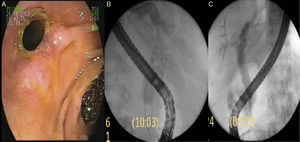
A repeat endoscopic cholangiography was performed 6 weeks later identifying hyperplastic tissue atthe distal end of the stent, at the papilla of Vater (fig. 2). Through insufflation of a 12mm dilating balloon inside the stent, it was dislodged from the hyperplastic tissue and removed with a polypectomy loop.
The cholangiogram showed multiple stone fragments under 10mm that were completely removed with a biliary extraction balloon and Dormia basket (fig. 2).
The patient has had no biliary intercurrence during follow-up.
Many authors have stressed the importance of plastic biliary stents in the management of complex stones because they ensure bile duct permeability and exert friction on the stones, resulting in their fragmentation. However, the reported bile duct stone clearance rates after plastic stent removal are between 40 and 70%.6–9
The particularities of covered metal stents have increased resolution rates to 91%.9 Their radial expansion force compresses and applies friction to the stones, fragmenting them, softening them, and reducing their size. In addition, they exert sustained dilation on the papilla, as well as the distal bile duct, improving the container-content relation. Published studies have reported higher bile duct stone clearance rates with fewer procedures, making this technique more cost-effective than the placement of plastic stents.2,7–9
No major complications have been reported in relation to either the placement or removal of these stents. A low percentage of distal migration and papillary tissue hyperplasia with no clinical repercussions has been reported.8,9
We should underline that this technique does not represent a risk for patients that have a gallbladder, given that there has been no evidence of increased rates of cholecystitis associated with the use of covered metal stents.10
Our patient presented with severe aortic stenosis that contraindicated surgical management and so resolution had to be attained with the least number of interventions possible. This demanded a method that would work on both the content (stone) and the container (distal bile duct). The covered metal stent met all the necessary conditions to be the most effective option.
In conclusion, for patients with failed initial stone extraction, the placement of a covered, self-expanding metallic biliary stent can be safe and effective for attaining transitory biliary drainage. In addition, through the exertion of radial force, stone fragmentation and papillary dilation are achieved. Randomized and controlled trials are required to validate this technique for the management of complex stones.
Financial disclosureNo financial support was received in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
The authors wish to thank the Research Area of the Hospital El Cruce Dr. Néstor Carlos Kirchner, and especially the physicians Maximiliano De Abreu and Laura Antonietti for their collaboration in preparing this manuscript.
Please cite this article as: Curvale C, Guidi M, Hwang H, De Maria J, Matanó R. Resolución de coledocolitiasis compleja con stent metálico removible. Reporte de un caso. Revista de Gastroenterología de México. 2016;81:56–58.