¿ Introduction
Primary epiploic appendagitis is a rare condition that occurs after either torsion or spontaneous venous thrombosis with subsequent development of infarct and inflammation. Before the use of the CT scan, most of the cases were diagnosed during surgery. Clinical presentation is unspecific, and most of the times can mimic acute diverticulitis, acute cholecystitis or acute appendicitis. Once the diagnosis of epiploic appendagitis is made, conservative treatment must be initiated to avoid unnecessary surgery. Surgical treatment is reserved for patients in whom conservative treatment fails or for patients whose signs and symptoms worsen.
¿ Case report
Case 1
A 53-year-old woman arrived in the emergency room complaining of acute abdominal pain located on the left flank of 12 hours of evolution. The pain was constant in intensity, rating 7 out of 10 without radiations. No nausea, vomiting, fever or chills were associated. During the physical examination the vital signs were normal and the patient had left lower quadrant pain with tenderness and rebound. The white blood cell count was 6,200 leukocytes /mm3. The rest of the laboratory workup was normal.
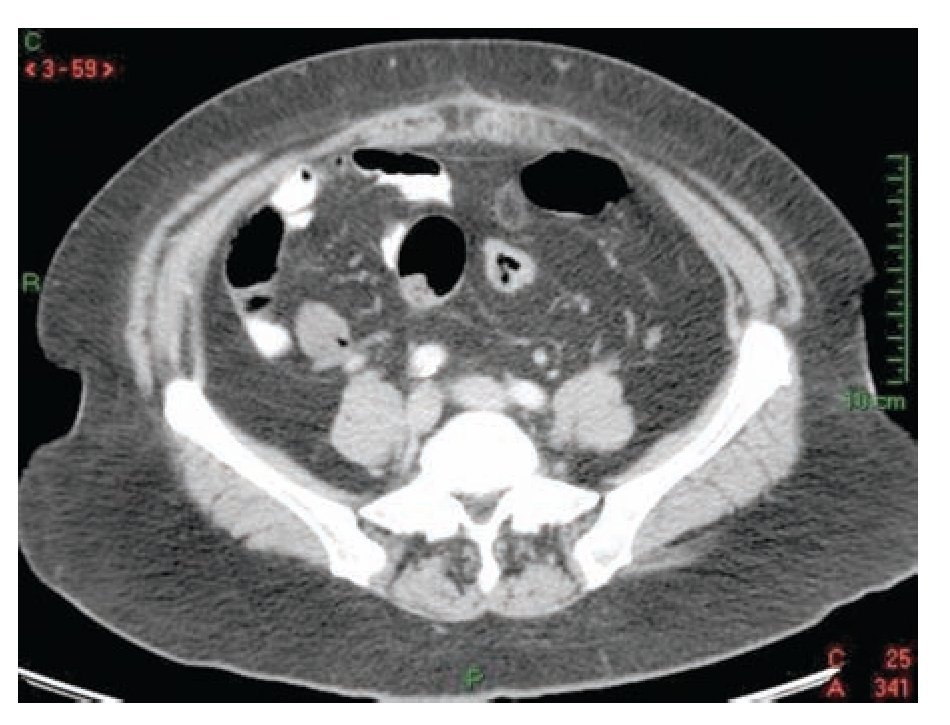
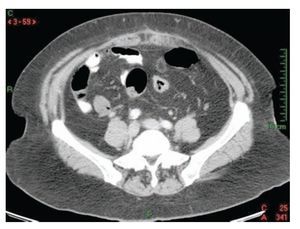
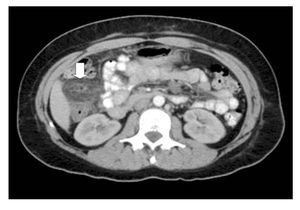
With the clinical suspicion of acute diverticulitis the patient underwent an abdominal computed tomography (CT), and findings were suggestive of acute epiploic appendagitis (Figure 1). The patient was admitted for hospitalization and intravenous non-steroidal anti-inflammatory drugs (NSAID) were started; 24 hours after the hospitalization the symptoms improved and pain decreased in 50% and the patient was discharged from the hospital to continue ambulatory treatment with NSAID orally. Symptoms disappeared five days later and no further complications occurred. Six weeks after the hospitalization, the patient underwent a colonoscopy which ruled out colonic diverticular disease.
¿ Figure 1. Abdominal CT showing an ovoid mass with inflammatory changes in surrounding fat.
Case 2
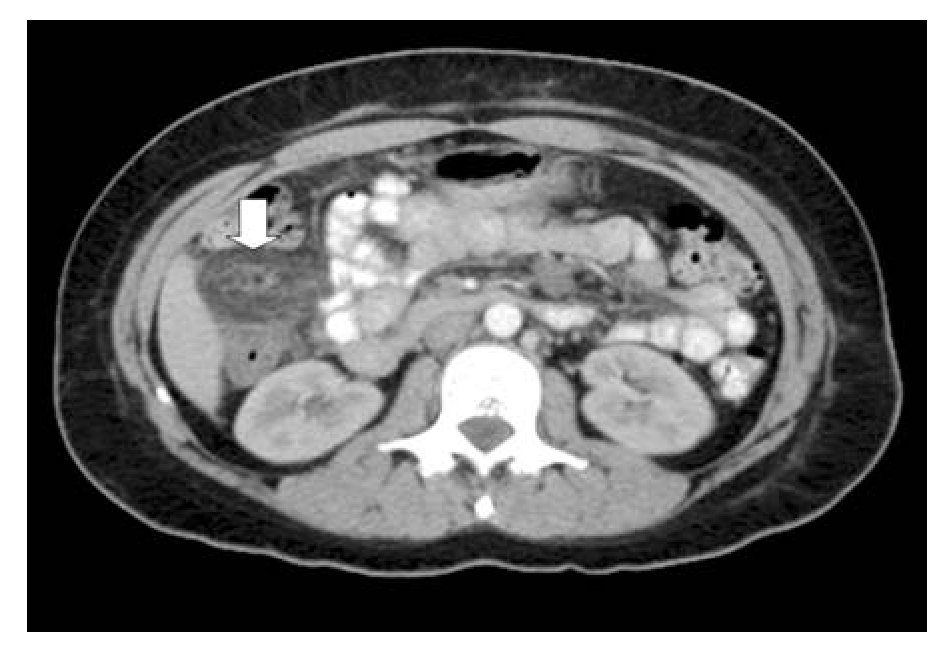
A 36-year-old female physician arrived to the office with acute onset of abdominal pain of four hours of evolution localized on right flank. She was working at the intensive care unit when symptoms began. During the physical examination the patient had tachycardia (100 bpm) and the abdomen showed signs compatible with peritonitis on right flank. The white blood cell count was 12,000/mm3 with left deviation. The rest of laboratory exams were normal. Under the suspicion of acute cholecystitis, an abdominal ultrasound was performed. The study ruled out this diagnosis. Subsequently the patient developed nausea and vomiting and an abdominal CT was performed. Findings were consistent with an inflammatory process located in the fat surrounding the ascending colon suggestive of acute epiploic appendagitis (Figure 2). The patient was started in NSAID and symptoms disappeared three days after the medication was started. She didn't require hospitalization.
¿ Figure 2. Abdominal CT showing a circular mass, inflammatory changes in surrounding fat, thickening of colonic wall and displacement of peripheral structures.
Case 3
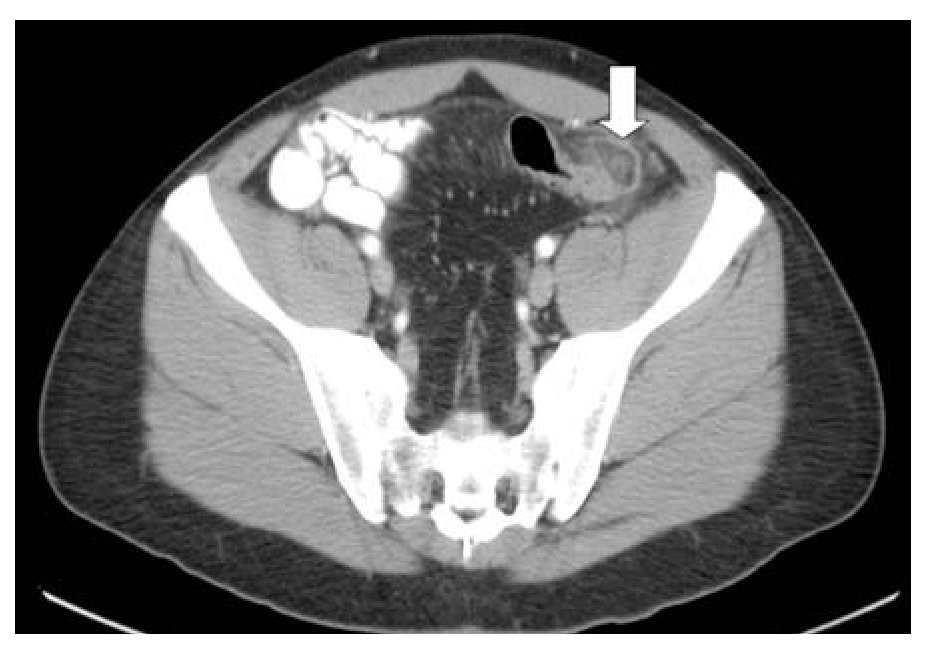
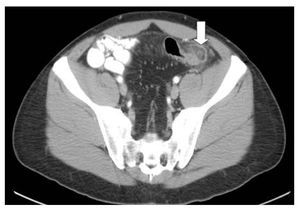
A 34-year-old previously healthy male came to the office complaining of acute abdominal pain of six hours of evolution. The pain was rated 6/10 in intensity, constant, pressure-like, located at left lower quadrant of the abdomen. No other symptoms were associated. During the physical examination his vital signs were normal. The abdomen was tender and rebound was located at left lower quadrant. The white blood cell count was 8600/mm3. A potential diagnosis of acute diverticulitis was made and the patient underwent an abdominal CT scan. The findings were compatible with acute epiploic appendangitis located at the sigmoid colon (Figure 3). The diagnosis of acute diverticulitis was ruled out, and treatment was started with oral NSAIDs with resolution of symptoms 72 hours later.
¿ Figure 3. Abdominal CT showing an ovoid mass, inflammatory changes and displacement of sigmoid colon.
In all patients described above, the NSAIDs included ketorolac (10 mg each six hours) and eterocoxib (60 mg each 12 hours) during one week.
¿ Discussion
Primary epiploic appendagitis is considered to be a rare, inflammatory intraabdominal process that is attributable to either torsion or spontaneous venous thrombosis of an epiploic appendage with subsequent ischemic infarction and inflammation.1-3 The frequency of this entity is estimated at 1.3% and its incidence in 8.8 cases/million habitants.1 This is a condition that, before CT was available, was most commonly diagnosed during surgery.2 Epiploic appendages are fat pouches that arise from the serosal surface of the colon from the cecum to the rectosimoid junction, to which they are attached by a vascular stalk. Composed of adipose tissue and blood vessels, the appendages typically have a length of 0.5-5 cm.1,3 Suggested functions of the epiploic appendages include potential bacteriostatic properties, a role in colonic absorption, and a flexible cushion to protect the blood supply when the colon is collapsed.4 The largest appendages are found in the descending colon and cecum, which are the most common locations for torsion to occur. Epiploic appendages are enlarged in obese patients, which increase their risk for torsion.5 The three patients reported had a body mass index > 25.
Primary acute epiploic appendagitis is usually a result of torsion, with ischemic changes in the epiploic appendix, but it also can be caused by thrombosis, without any evidence of torsion. Secondary epiploic appendagitis is caused by inflammation of the adjacent organs (eg, diverticulitis, appendicitis, and cholecystitis). The cause of primary epiploic appendagitis is unknown, but torsion has been associated with obesity, hernia, and unaccustomed exercise. In the three patients reported the only risk factor associated was obesity. Inflammation of the epiploic appendages is self-limited in the majority of patients. Rarely, acute epiploic appendagitis may result in adhesion, bowel obstruction, intussusception, intraperitoneal loose body, peritonitis, and/or abscess formation.2,3 This condition is more common during the 4th and 5th decades of life, predominantly in men. Acute epiploic appendagitis is misdiagnosed in the majority of patients.2 Clinically, acute epiploic appendagitis manifest with acute onset of pain in the left lower quadrant and there is absence of other notable complaints or clinical findings.1,2 Most patients have a normal white blood cell count and temperature.2 Upon clinical examination, there are no signs or symptoms that allow a definite differentiation of other common abdominal processes.1 There's a report of a male elderly patient with chronic vague abdominal pain without evidence of acute onset of symptoms.6 According to their location, they can mimic acute appendicitis, diverticulitis, or cholecystitis.1-8 Two of our patients simulated an acute diverticulitis and the other one simulated an acute appendicitis. It´s very important to rule out this diagnosis in order to avoid an unnecessary surgical procedure, especially when clinical examination is compatible with left lower quadrant peritonitis as occurred in two patients in our series. When the clinical picture simulates an acute diverticulitis a colonoscopy is required once the acute episode is solved to rule out the presence of colonic diverticular disease.
Normal epiploic appendages are not visible on ultrasound-unless the colon is surrounded by extraluminal fluid.5 The ultrasound findings of acute appendangitis include a solid, hyperechoic, noncompressible, ovoid mass at the area of maximum tenderness.3,5 The mass is often surrounded by a thin hypoechoic rim, believed to represent thickening of the serosa of the appendage and the adjacent parietal peritoneum.5 In 70% of the patients, a mass effect on the adjacent bowel and a mass fixed to the anterior abdominal is present.3
Color Doppler sign is typically absent within the echogenic mass.5 Typically, the epiploic appendages are visible in CT images only when they are inflamed and/or surrounded by fluid.2 In most cases, primary epiploic appendagitis has virtually pathognomonic CT findings, appearing as a pericolonic, oval-shaped lesion with fat attenuation, thickened visceral peritoneal lining, periappendageal fat stranding, as well as a mass effect, focal wall thickening of the adjacent colon.1-3 At times, a central high-attenuation focus, thought to represent a thrombosed vessel, is present.9 Although the clinical symptoms are solved in two weeks for most patients, the CT findings could be perpetuated until six months.2 In our patients, abdominal CT was specific to diagnose acute epiploic appendagitis. The MRI appearance is an oval-shaped lesion located anterior or anterolateral to the colon with a central area that follows the signal intensity of fat on T-1 and T-2 weighted images. The inflamed visceral peritoneum appears as a low signal intensity rim surrounding the fat-density appendage on T-1 and T-2 weighted images that are enhanced after the administration of gadolinium. A hypointense central dot can be demonstrated on both T-1 and T-2 weighted images.8
When acute epiploic appendagitis is diagnosed on the basis of CT findings, unnecessary surgery for this self-limiting, benign disorder can be avoided,1 and patients are treated conservatively with oral-antiinflammatory medications.2 In case the patient symptoms fail to improve with medical management, laparoscopy is indicated.4 The three patients reported were treated conservatively and symptoms disappeared. In a recent report,10 only one patient was treated conservatively, while other nine patients were treated by surgery. We believe with firm basis that medical treatment in these patients must to be the treatment of choice when the diagnosis is made with the imaging techniques.
Follow up with these patients showed a decrease in size with fat attenuation, but sometimes to a nugget with soft-tissue attenuation that likely reflected scar-tissue deposition. These lesions also changed in shape and contour, usually from a well-defined, smooth oval shape to a structure with a shape that is irregular, oval, or round.1
In conclusion, although this is a rare condition, it is imperative to rule out acute epiploic appendagitis as the cause of acute abdomen, especially in patients in which there is not a "classic presentation" of appendicitis or diverticulitis or when clinical findings are bizarre and unspecific to avoid surgery.
Correspondence: Dr. Miguel Ángel Sánchez-Pérez.
Carlos Graef Fernández N°154-515, Colonia Tlaxala, CP 05300, México City.
Telephone/Fax: (5255) 1664 7164.
E-mail: wfrguitarma@hotmail.com