Functional gastrointestinal disorders (FGIDs) are common digestive conditions characterized by chronic or recurrent symptoms in the absence of a clearly recognized gastrointestinal etiology. The biopsychosocial model, the most accepted concept explaining chronic pain conditions, proposes that the interplay of multiple factors such as genetic susceptibility, early life experiences, sociocultural issues, and coping mechanisms affect children at different stages of their lives leading to the development of different pain phenotypes and pain behaviors. Early life events including gastrointestinal inflammation, trauma, and stress may result in maladaptive responses that could lead to the development of chronic pain conditions such as FGIDs.
AimsIn this review, we discuss novel findings from studies regarding the long-term effect of early life events and their relationship with childhood chronic abdominal pain and FGIDs.
MethodsA bibliographic search of the PubMed database was conducted for articles published over the last 20 years using the keywords: “Functional gastrointestinal disorders”, “chronic abdominal pain”, “chronic pain”, “gastrointestinal inflammation”, and “early life events”. Forty-three articles were chosen for review.
ResultsBased on the current evidence, events that take place early in life predispose children to the development of chronic abdominal pain and FGIDs. Conditions that have been studied include cow's milk protein hypersensitivity, pyloric stenosis, gastrointestinal infections, and Henoch–Schonlein purpura, among others.
ConclusionsEarly events may play an important role in the complex pathogenesis of functional gastrointestinal conditions. Timely intervention may have a critical impact on the prevention of this group of chronic incapacitating conditions.
Los trastornos funcionales gastrointestinales (FGID) son condiciones que se caracterizan por la presencia de síntomas crónicos o recurrentes en ausencia de una etiología orgánica. El modelo biopsicosocial utilizado como marco conceptual de las condiciones de dolor crónico propone que la interacción de diferentes factores, como la susceptibilidad genética, los eventos en edad temprana, los factores socioculturales y los mecanismos de adaptación al dolor, afectan a los niños en diferentes estadios de sus vidas y eventualmente resultan en el desarrollo de síndromes de dolor crónico. La inflamación gastrointestinal, el traumatismo y estrés en la edad temprana pueden resultar en una adaptación inadecuada que llevaría al desarrollo de condiciones de dolor crónico tales como los FGID.
ObjetivosEn este artículo de revisión se analizan nuevas evidencias de estudios que examinan eventos en edad temprana y sus efectos a largo plazo, así como su relación con el desarrollo de dolor abdominal crónico y FGID.
Materiales y métodosBúsqueda bibliográfica en la base de datos PubMed en los últimos 20 años usando los términos: «functional gastrointestinal disorders», «chronic abdominal pain», «chronic pain», «gastrointestinal inflammation» and «early life events».
ResultadosLos eventos en la edad temprana predisponen al niño al desarrollo de dolor abdominal crónico y FGID. Entre los desórdenes estudiados tenemos: hipersensibilidad a la proteína de la leche, estenosis pilórica, infecciones gastrointestinales y púrpura de Henoch–Schonlein, entre otros.
ConclusionesLos eventos en la edad temprana cumplen un papel importante en la compleja patogénesis de los FGID. Una intervención oportuna puede ser de un impacto crítico en la prevención de este grupo de condiciones.
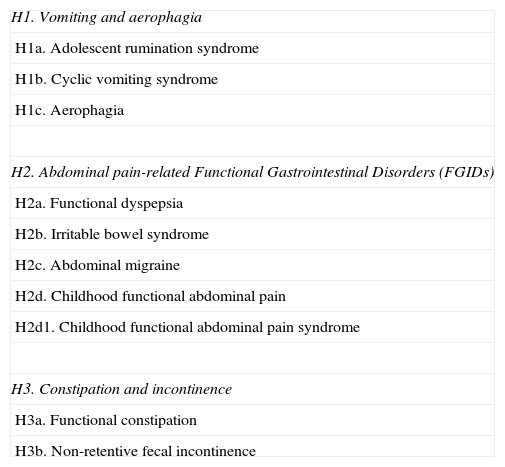
Functional gastrointestinal disorders (FGIDs) are characterized by the presence of chronic or recurrent digestive symptoms without an underlying identifiable structural or biochemical abnormality.1,2 As such, there are no biological markers to diagnose FGIDs. The diagnosis of FGIDs is based exclusively on the symptoms reported by the child and parents. According to the Rome III criteria,3 the subgroup of FGIDs associated with abdominal pain (abdominal pain-associated FGIDs) is subdivided into four disorders: Irritable Bowel Syndrome (IBS), Functional Dyspepsia, Abdominal Migraine, and Childhood Functional Abdominal Pain (this includes the subgroup of Childhood Functional Abdominal Pain syndrome in children with loss of daily functioning or other somatic complaints) (Table 1). A large proportion of children with complaints of chronic abdominal pain of non-organic origin cannot be diagnosed with a FGID if the Rome criteria are strictly applied. It is unclear whether there is a difference in pathophysiology or impact on quality of life between children who do not meet one or more items of the Rome criteria and children who meet all of them.
Rome III classification of functional disorders in children and adolescents.
| H1. Vomiting and aerophagia |
| H1a. Adolescent rumination syndrome |
| H1b. Cyclic vomiting syndrome |
| H1c. Aerophagia |
| H2. Abdominal pain-related Functional Gastrointestinal Disorders (FGIDs) |
| H2a. Functional dyspepsia |
| H2b. Irritable bowel syndrome |
| H2c. Abdominal migraine |
| H2d. Childhood functional abdominal pain |
| H2d1. Childhood functional abdominal pain syndrome |
| H3. Constipation and incontinence |
| H3a. Functional constipation |
| H3b. Non-retentive fecal incontinence |
Adapted from Rasquin et al.3.
Chronic abdominal pain and abdominal pain-associated FGIDs are common in children. Large community-based studies conducted in geographically and socio-culturally diverse areas found a similar prevalence of abdominal pain and FGIDs in children. Thirty-eight percent of American school-age children4 and 35% of Colombian children5 report abdominal pain weekly. A school-based study found FGIDs in 27% of Colombian children. A cross-sectional survey conducted in a semi-urban school in Sri-Lanka found FGIDs in 28.8% of the children6. Eleven percent of 1200 Colombian schoolchildren and 12.5% of 2163 randomly selected Sri-Lankan adolescents were diagnosed with an abdominal pain-associated FGID;7 IBS was the most common abdominal pain-associated FGID in both studies (Colombia 4.2%, Sri-Lanka 4.9%).8
ImpactThe socioeconomic burden associated with chronic abdominal pain and abdominal pain-associated FGIDs is substantial.9,10 Children and adolescents with abdominal pain and abdominal pain-associated FGIDs frequently experience poor quality of life and disability.11,12 School-aged children with abdominal pain have higher anxiety and depression scores and worse quality of life than their peers.13 Twenty-three percent of children with abdominal pain miss school in a six-month period, and 10% of their parents miss work to care for their sick children.4 Most school-aged children with abdominal pain never seek medical attention for their symptoms.14 The percentage of children who seek medical attention is consistent across studies in areas with different access to medical care and sociocultural background. An American study conducted in a large city (Chicago) and a study conducted in a semirural city in Colombia showed that in both cases only 2–3% of the children who reported abdominal pain sought medical attention. The low ratio of consultation suggests that many children suffer from abdominal pain without receiving professional attention. In those children consulting for abdominal pain, the healthcare costs associated with medical care are considerable. A study conducted in Uruguay showed that the direct healthcare costs associated with a single pediatric consultation for abdominal pain accounted for 4% of the per capita health care spending in one year.15 Costs involved with the care of a child with abdominal pain in the US are also extremely high. The average cost to care for a child with abdominal pain in a tertiary care center in the US exceeds $6000 USD.9 One third of pediatric patients undergo esophagogastroduodenoscopy that rarely changes the patient's management. Despite the presence of common symptoms such as abdominal pain, bloating, distention, diarrhea, and constipation in patients with celiac disease and IBS, celiac disease is rarely found in children presenting with isolated abdominal pain, and celiac disease is infrequent in children with IBS.9 The value of reassuring parents by demonstrating a negative endoscopy is open to question. Children who were told they had a negative endoscopy had the same prognosis as those who were not subjected to endoscopy.16 The cumulative lifetime healthcare costs associated with FGIDs are even more substantial. Almost a third of all the adults that consult for FGIDs began experiencing gastrointestinal symptoms in childhood.17,18 Long-term follow-up studies have shown that adolescents and young adults with a past history of FGIDs are likely to report other somatic complaints including chronic abdominal pain and headache several years after the initial presentation.19,20 Direct and indirect costs related to the care of IBS and other somatic complaints frequently present in adults are enormous. The high personal, familiar, and societal burden associated with FGIDs has raised great interest in unveiling the pathogenesis and pathophysiological mechanisms of FGIDs. The biopsychosocial model, the most accepted construct explaining chronic pain conditions21 recognizes the interaction between genetic susceptibility and early life experiences, social and environmental influences, psychological and physiological processes, social and environmental influences, and individual coping mechanisms in the development of FGIDs.22 Several animal and human studies suggest that events occurring early in life may constitute an additional and potentially important contributing factor to the development of FGIDs.23 A better understanding of the various early life events that may contribute to the development of FGIDs could offer a unique opportunity for early intervention to prevent the development of FGIDs and decrease the number of children with FGIDs who continue suffering into adulthood.
FGIDs are more common among members of the same family.24–28 A parental history of IBS is an independent predictor of the development of IBS in the offspring.29 Children with a maternal history of IBS have a higher frequency of gastrointestinal and non-gastrointestinal symptoms, disability days, and clinical visits compared with those that do not have a similar history.30 Several studies have tried to uncover possible genetic associations that could explain FGIDs. Some of the studies found that distinct gene polymorphisms implicated in 5-HT metabolism were more frequently present in patients with IBS.31 Cytokine gene polymorphisms were also found to be associated with irritable bowel syndrome.32 However, other genetic studies had disappointing results. Guanine nucleotide binding protein (G-protein) beta polypeptide 3 (GNB3) C825T polymorphisms that were presumed to be associated with some FGIDs were found to be equally present in cases and controls.33 Most of the experts believe that the genetic contribution to the development of FGIDs is likely to be modest. None of the genetic findings can solely explain the pathophysiology of FGIDs. Twin and family studies support the coexistence of genetic and environmental contributing factors in the pathogenesis of IBS. Monozygotic twins are more likely to develop FGIDs than dizygotic twins.29 However, the same study showed that having a mother and a father with IBS were independent predictors of IBS, indicating that social learning and parental response to illness had an equal or greater influence than heredity to the development of FGIDs. Chronic abdominal pain is more common in families with higher rates of reported illnesses and anxiety.34,35 Parental anxiety and preoccupation with physical health may reinforce the child's own concerns about physiological or minor body sensations.30 Studies have demonstrated that some biological factors could also be associated with a greater risk for developing FGIDs. Restricted fetal growth has a significant influence on the development of IBS later in life, with weight below 1500g influencing age of onset.26 In conclusion, abdominal pain and abdominal pain-related FGIDs are a global health problem that is present across ethnicities, nationalities, and geographic locations and is associated with significant health care expenditure. The pathogenesis of and the individual contributions of the various factors to the development of FGIDs remain unclear despite the increasing body of research focused on elucidating these mechanisms.
In this review, we first examine the available evidence on the effects of exposure to pain during the neonatal period. We then discuss novel findings from studies concerning the long-term effect of early life events including cow's milk protein hypersensitivity, pyloric stenosis, and other common pediatric conditions occurring later in childhood, such as gastrointestinal infections and immune conditions that predispose children to chronic abdominal pain and FGIDs (Tables 2–4).
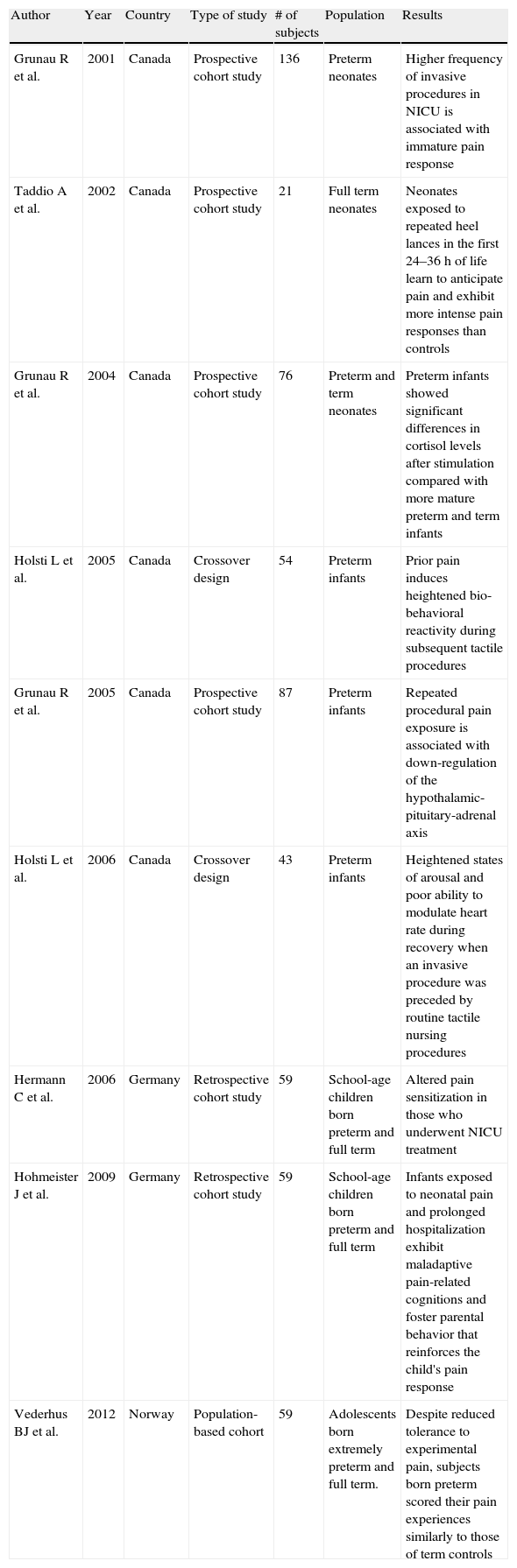
Pain exposure during the neonatal period. Summary of studies in human subjects.
| Author | Year | Country | Type of study | # of subjects | Population | Results |
| Grunau R et al. | 2001 | Canada | Prospective cohort study | 136 | Preterm neonates | Higher frequency of invasive procedures in NICU is associated with immature pain response |
| Taddio A et al. | 2002 | Canada | Prospective cohort study | 21 | Full term neonates | Neonates exposed to repeated heel lances in the first 24–36h of life learn to anticipate pain and exhibit more intense pain responses than controls |
| Grunau R et al. | 2004 | Canada | Prospective cohort study | 76 | Preterm and term neonates | Preterm infants showed significant differences in cortisol levels after stimulation compared with more mature preterm and term infants |
| Holsti L et al. | 2005 | Canada | Crossover design | 54 | Preterm infants | Prior pain induces heightened bio-behavioral reactivity during subsequent tactile procedures |
| Grunau R et al. | 2005 | Canada | Prospective cohort study | 87 | Preterm infants | Repeated procedural pain exposure is associated with down-regulation of the hypothalamic-pituitary-adrenal axis |
| Holsti L et al. | 2006 | Canada | Crossover design | 43 | Preterm infants | Heightened states of arousal and poor ability to modulate heart rate during recovery when an invasive procedure was preceded by routine tactile nursing procedures |
| Hermann C et al. | 2006 | Germany | Retrospective cohort study | 59 | School-age children born preterm and full term | Altered pain sensitization in those who underwent NICU treatment |
| Hohmeister J et al. | 2009 | Germany | Retrospective cohort study | 59 | School-age children born preterm and full term | Infants exposed to neonatal pain and prolonged hospitalization exhibit maladaptive pain-related cognitions and foster parental behavior that reinforces the child's pain response |
| Vederhus BJ et al. | 2012 | Norway | Population-based cohort | 59 | Adolescents born extremely preterm and full term. | Despite reduced tolerance to experimental pain, subjects born preterm scored their pain experiences similarly to those of term controls |
NICU: neonatal intensive care unit.
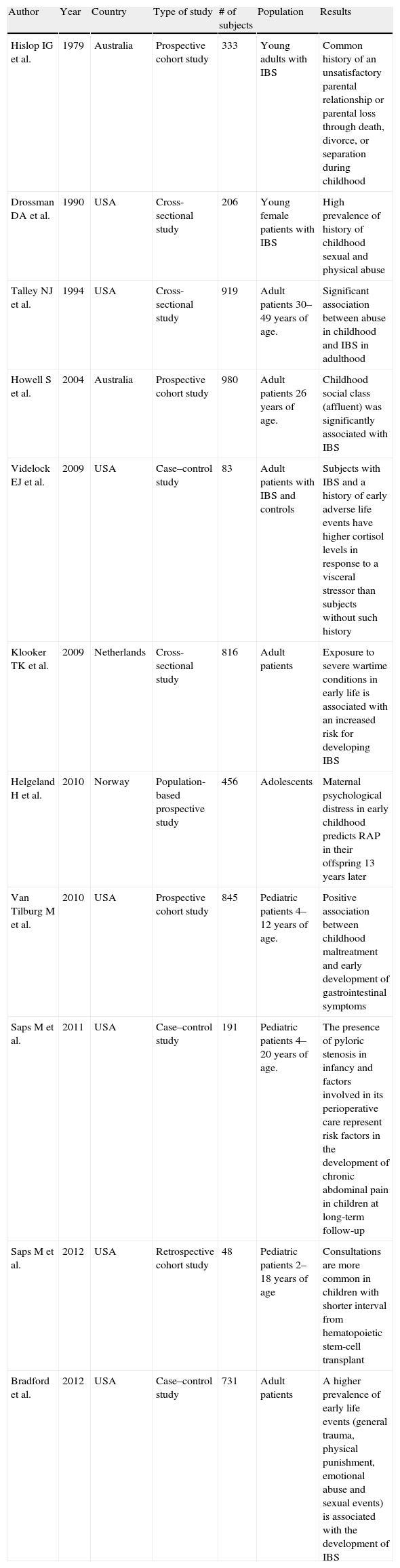
Stress and early trauma. Summary of studies in human subjects.
| Author | Year | Country | Type of study | # of subjects | Population | Results |
| Hislop IG et al. | 1979 | Australia | Prospective cohort study | 333 | Young adults with IBS | Common history of an unsatisfactory parental relationship or parental loss through death, divorce, or separation during childhood |
| Drossman DA et al. | 1990 | USA | Cross-sectional study | 206 | Young female patients with IBS | High prevalence of history of childhood sexual and physical abuse |
| Talley NJ et al. | 1994 | USA | Cross-sectional study | 919 | Adult patients 30–49 years of age. | Significant association between abuse in childhood and IBS in adulthood |
| Howell S et al. | 2004 | Australia | Prospective cohort study | 980 | Adult patients 26 years of age. | Childhood social class (affluent) was significantly associated with IBS |
| Videlock EJ et al. | 2009 | USA | Case–control study | 83 | Adult patients with IBS and controls | Subjects with IBS and a history of early adverse life events have higher cortisol levels in response to a visceral stressor than subjects without such history |
| Klooker TK et al. | 2009 | Netherlands | Cross-sectional study | 816 | Adult patients | Exposure to severe wartime conditions in early life is associated with an increased risk for developing IBS |
| Helgeland H et al. | 2010 | Norway | Population-based prospective study | 456 | Adolescents | Maternal psychological distress in early childhood predicts RAP in their offspring 13 years later |
| Van Tilburg M et al. | 2010 | USA | Prospective cohort study | 845 | Pediatric patients 4–12 years of age. | Positive association between childhood maltreatment and early development of gastrointestinal symptoms |
| Saps M et al. | 2011 | USA | Case–control study | 191 | Pediatric patients 4–20 years of age. | The presence of pyloric stenosis in infancy and factors involved in its perioperative care represent risk factors in the development of chronic abdominal pain in children at long-term follow-up |
| Saps M et al. | 2012 | USA | Retrospective cohort study | 48 | Pediatric patients 2–18 years of age | Consultations are more common in children with shorter interval from hematopoietic stem-cell transplant |
| Bradford et al. | 2012 | USA | Case–control study | 731 | Adult patients | A higher prevalence of early life events (general trauma, physical punishment, emotional abuse and sexual events) is associated with the development of IBS |
IBS: irritable bowel syndrome; RAP: recurrent abdominal pain.
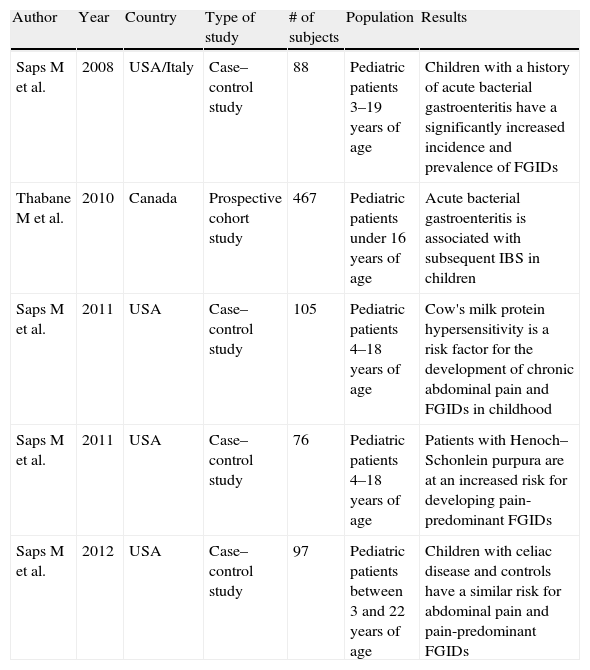
GI inflammation. Summary of studies in human subjects.
| Author | Year | Country | Type of study | # of subjects | Population | Results |
| Saps M et al. | 2008 | USA/Italy | Case–control study | 88 | Pediatric patients 3–19 years of age | Children with a history of acute bacterial gastroenteritis have a significantly increased incidence and prevalence of FGIDs |
| Thabane M et al. | 2010 | Canada | Prospective cohort study | 467 | Pediatric patients under 16 years of age | Acute bacterial gastroenteritis is associated with subsequent IBS in children |
| Saps M et al. | 2011 | USA | Case–control study | 105 | Pediatric patients 4–18 years of age | Cow's milk protein hypersensitivity is a risk factor for the development of chronic abdominal pain and FGIDs in childhood |
| Saps M et al. | 2011 | USA | Case–control study | 76 | Pediatric patients 4–18 years of age | Patients with Henoch–Schonlein purpura are at an increased risk for developing pain-predominant FGIDs |
| Saps M et al. | 2012 | USA | Case–control study | 97 | Pediatric patients between 3 and 22 years of age | Children with celiac disease and controls have a similar risk for abdominal pain and pain-predominant FGIDs |
FGIDs: functional gastrointestinal disorders; IBS: irritable bowel syndrome.
A bibliographic search of the PubMed database was conducted for articles published over the last 20 years using the keywords: “Functional gastrointestinal disorders”, “chronic abdominal pain”, “chronic pain”, and “early life events”. Forty-three articles were chosen for the literature review.
Effects of exposure to pain during the neonatal periodClinical and laboratory investigations in neonatal pain have shown that exposure to an early insult – physical and/or psychological – results in maladaptive CNS responses that in turn can lead to the development of chronic pain disorders. Studies conducted in neonatal rat pups showed that exposure to repetitive pain led to altered maturation of the pain system and decreased pain thresholds.36 Preterm neonates that are exposed to acute painful stimuli experience prolonged periods of hyperalgesia.37,38 Premature babies who had a higher frequency of invasive procedures in the Neonatal Intensive Care Unit (NICU) are less mature in their pain response.39 In preterm infants, prior pain induces an increased bio-behavioral reactivity during subsequent tactile procedures.40 Repeated procedural pain exposure is associated with down-regulation of the hypothalamic-pituitary-adrenal axis as measured by cortisol levels.41 Preterm infants who were born at an extremely low gestational age showed significant differences in cortisol levels after stimulation, compared with more mature preterm and term infants.42 Heightened states of arousal and poor response to invasive procedures have also been described in earlier born preterm infants.43
Newborns exposed to repeated heel lances in the first 24–36h of life learn to anticipate pain and exhibit more intense pain responses during venipuncture than controls.44 Similar changes have been reported in long-term follow-up studies of ex-preterm neonates who had prolonged stays in the NICU. Altered pain sensitization was also found in school-age children who had undergone NICU treatment.45 Severe inflammatory pain and painful repetitive injections during the first week of life leads to key changes in the developing brain of the neonatal rat.46 The neonatal period is a time of high neural plasticity and insults that occur during this period may alter the development of the Central Nervous System (CNS) and influence future pain responses. However, the mechanisms underlying the long-term adaptations to pain are complex and have yet to be completely elucidated.45,47,48 Early life noxious stimuli also affect the gastrointestinal tract. Noxious stimuli in early stages may lead to the development of long-term gastrointestinal hyperalgesia through various putative mechanisms including sensitization of primary sensory or spinal neurons, altered stress response, and/or impaired descending inhibitory control.49 Animal studies have linked gastrointestinal injury to the development of long-term hyperalgesia by demonstrating that neonatal gastrointestinal noxious stimulation can induce long-lasting changes in pain behavior. Neonatal rats infused with iodoacetamide by oral gavage developed chronic gastric hypersensitivity and gastric motor dysfunction as adults in the absence of detectable gastric pathology.50 Neonatal rats subjected to repeated orogastric suctioning develop chronic somatic and visceral hyperalgesia during adulthood.51 Chemically induced mild, transient colitis results in persistent visceral hyperalgesia and referred pain in rats.52 Evidence from animal studies suggests that chemically induced colitis and repeated colorectal distention in neonatal mice leads to chronic visceral hypersensitivity associated with peripheral and central sensitization as adults. The same phenomenon is not present if the noxious stimulus is applied in adulthood.53,54
Early life psychological stress may also act as a contributing factor toward sensitization to visceral pain. The model of maternal separation allows for the investigation of potential mechanisms involved in stress-related disorders.55,56 Neonatal maternal separation predisposes rats to develop features that mimic IBS, such as visceral hyperalgesia, increased colonic motility, and reduced somatic analgesia when exposed to an acute psychological stressor.57 Male rat pups that were separated from their mothers have a higher number of bowel movements and higher plasma corticosterone levels in response to stress when compared with controls.58 Stressed pups exhibit increased visceral sensation, changes in fecal microbiota, and a heightened systemic immune response after an in vitro lipopolysaccharide challenge. Using the same model of early psychological stress associated with maternal separation, a group of investigators assessed colorectal balloon distention and its relation to abdominal withdrawal reflex as a surrogate marker of visceral pain.59 The investigators found a significantly higher abdominal withdrawal reflex score in response to colorectal balloon distention in the maternal separation group. The expression of 5-HT, 5-HT3 receptors, and 5-HT transporter in brain and spine tissue was also significantly increased in the maternal separation group, compared with controls. Pain threshold was also significantly lower in the maternal separation group. Only the maternal separation group had a significant increase in 5-HT content in the colon. There is evidence that neonatal maternal separation sensitizes the cingulate cortex and upregulates the activity of the ascending pathway at the spinal level, as well as the thalamo-cortico-amygdala pathway, in response to colorectal distention.60 The authors postulate that the sensitization of these pathways may be responsible for the development of visceral hypersensitivity in IBS. An increased expression of corticotrophin releasing factor (CRF) and CRF type 1 receptor (CRF-R1) was found in the thalamus of neonatal rats exposed to maternal separation.61 Together these results suggest that in line with the biopsychosocial model, animals exposed to early life psychological stress develop brain–gut axis dysfunction.
Early gastrointestinal inflammation, trauma, and stressFor ethical and logistical reasons, most studies on the effect of early life events in gastrointestinal health have been conducted on animals. Lack of human models has limited the progress of research in this area. Gastrointestinal inflammation and physical trauma to the gastrointestinal tract, the most commonly used models in animals, cannot be reproduced in humans for obvious reasons. Recently, our group proposed human models to study the long-term effect of early gastrointestinal inflammation, trauma, and stress. In the first study of our series, we demonstrated that cow's milk protein hypersensitivity – a common transient gastrointestinal inflammatory condition of infancy – was a risk factor for the development of chronic abdominal pain and FGIDs later in childhood.62 This case–control study included 52 subjects between 4 and 18 years of age who were diagnosed with cow's milk protein hypersensitivity within the first year of life. Fifty-three healthy siblings of the same age were selected as controls. Twenty-three of the 52 study subjects (44.2%) reported GI symptoms that included abdominal pain, constipation, or diarrhea compared with 11 of the 53 controls (20.75%) (OR 3.03, p=0.01). Ten of the 52 subjects (19.2%) met the Rome III criteria for diagnosis of FGIDs (7 IBS, 2 functional dyspepsia, 1 functional abdominal pain), whereas none in the control group did. A second study by our group has shown that a history of pyloric stenosis in infancy is associated with the development of chronic abdominal pain in children at long-term follow-up.63 One hundred cases and 91 controls participated in the study with a mean time to follow-up of 7.22±1.64 years. Chronic abdominal pain was significantly more common in cases (20/100, 20%) versus controls (5/91, 5.8%) (OR 4.3, CI [1.54–11.99] [p=0.0045]). Seven out of 20 subjects (35%) met the Rome III criteria for diagnosis of an abdominal pain-associated FGID (3 IBS, 2 functional dyspepsia, 2 functional abdominal pain), whereas only 1 patient in the control group did (1 IBS) (OR 6.77, CI [0.82–56.17] [p=0.043]). This study suggested for the first time that the presence of pyloric stenosis in infancy or factors involved in its perioperative care, such as the use of antibiotics, nasogastric suction, pain related to the surgical incision, and personal and family stressors associated with the surgery, represent risk factors in the development of childhood chronic abdominal pain later in life. An additional benefit derived from this study was the identification of a novel model to study early life events in humans. A limitation of the study was the inability to isolate the single factor or identify the multiple factors explaining the increased risk of pain associated-FGIDs found in this group of children. In light of the biopsychosocial model, several aspects require further study. For example, the relationship between the age at which a patient receives a noxious stimulus and develops the risk for long-term gastrointestinal effects is unclear. The time period of early life events in humans is still undefined. The severity, type, and timing of the noxious stimuli most likely vary from subject to subject. In yet unpublished data, our group has found that surgery in older children also results in an increased risk for developing FGIDs. Pediatric and adult studies have shown that inflammatory conditions that present later in life can also lead to long-term chronic abdominal pain and FGIDs. Studies have found a significant increase in cases of FGIDs following bacterial infections in children outside of the infant period. A study on 44 children with a previous history of acute bacterial gastroenteritis who were contacted at least 6 months after the index episode, showed a significant increase in incidence and prevalence of FGIDs, compared with healthy controls of similar age and sex. Thirty-six percent of exposed patients and 11% of control subjects reported abdominal pain (p<0.01). Fifty-six percent reported onset of pain following the episode of acute gastroenteritis.64 A recent epidemiologic study conducted in children who experienced acute gastroenteritis as a result of an outbreak of bacterial contamination in the municipal water in Ontario, Canada, confirmed these findings.65 The study included 467 subjects, with 305 subjects who had a history of acute bacterial gastroenteritis and 162 unexposed controls. The cumulative incidence of IBS was significantly increased among exposed subjects vs. controls (10.5% vs. 2.5%; OR 4.6, 95% CI [1.6, 13.3]) and risk factors for the development of IBS were similar to those identified among adults.66–68 Non-infectious sources of inflammation have also been linked to the development of FGIDs in older children. A follow-up study of children diagnosed with Henoch–Schonlein purpura (HSP) who were contacted several months to years after the acute episode, has shown that HSP predisposes children to the development of FGIDs.69 Possible ongoing inflammation and persistence of symptoms from the time of diagnosis were excluded by review of records, laboratory, and parental interview. Sixty percent of children with a history of HSP and 2.6% of controls reported abdominal pain at follow-up. Children in the HSP group were diagnosed with various FGIDs (IBS in 11%, FAPS in 8%, and FAP in 2.8%). Celiac disease is another model of intestinal inflammation that allows for the investigation of the long-term effects of inflammatory changes in visceral pain. In order to assess whether celiac disease was a risk factor for long-term abdominal pain and FGIDs, our group conducted a case-control study involving 49 cases and 48 controls.70 Twelve children in the celiac disease group (24.5%) and 7 children in the control group (14.6%) had abdominal pain at the time of the study (p=0.3). Nine children in the celiac disease group (18.3%) and 4 children in the control group (8.3%) met the Rome criteria for an associated FGID (p=0.23). We found that children with celiac disease and controls have a similar risk for developing abdominal pain and abdominal pain-associated FGIDs. However, larger prospective studies should confirm these findings and investigate whether healthy siblings of celiac disease children have a higher prevalence of FGIDs. Consultation for abdominal pain is frequent in children who had hematopoietic stem-cell transplant. Our group found that consultations are more common in children with a shorter interval from hematopoietic stem-cell transplant. The results of the study suggest that post-hematopoietic stem-cell transplant follows the course of other inflammatory gastrointestinal conditions.71
Psychological stressors have also been shown to predispose to FGIDs in children. Maternal psychological distress during the child's early years is a risk factor for the development of recurrent abdominal pain during adolescence.72 A history of psychological, physical, or sexual abuse in childhood is a strong predictor of the development of gastrointestinal symptoms later in life.73–75 IBS patients have a higher prevalence of general trauma, physical punishment, emotional abuse, and sexual events than age and sex matched controls.76 This has been confirmed by physiologic studies that have shown that subjects with IBS and a history of early adverse life events have higher cortisol levels in response to a visceral stressor than subjects without a history of early adverse life events.77 Early-life exposure to severe wartime conditions was found to be associated with an increased prevalence of IBS.78 Adults who were less than 2 years of age during a war-related famine have a higher prevalence of IBS than the general population. Possible mechanisms involved include exposure to a stressful environment, severe malnutrition, or increased prevalence of infectious diseases. A history of an unsatisfactory parental relationship or parental loss through death, divorce, or separation during childhood was also found in 31–61% of IBS adult patients.79 Finally, the influence of the childhood socioeconomic environment on the development of adult IBS was studied using information from a New Zealand birth cohort study.80 The authors found that an affluent childhood setting was an independent risk factor for adult IBS.
ConclusionsEarly life events appear to be significant risk factors for the development of an abnormal response to pain later in life. Evidence from experimental and clinical studies suggests that early childhood is a critical time period in which psychological or physical trauma can induce visceral hyperalgesia. Early life events may play an important role in the complex pathogenesis of functional gastrointestinal conditions. Taken together, these findings are of great significance given that some of these events are potentially modifiable. Timely intervention may have a critical impact in the prevention of this group of chronic incapacitating conditions. These findings support the biopsychosocial model as a valid theoretical construct in FGIDs. Future studies are required to further evaluate the relative contribution of each of these factors to the pathogenesis of childhood FGIDs.
Conflict of interestThe authors declare that there is no conflict of interest.
Financial disclosureNo financial support was received in relation to this article.