Bouveret's syndrome is a rare type of gallstone ileus that consists of duodenal obstruction secondary to the passage of a stone through a cholecystoduodenal fistula and presents in elderly patients. A clinical case is described.
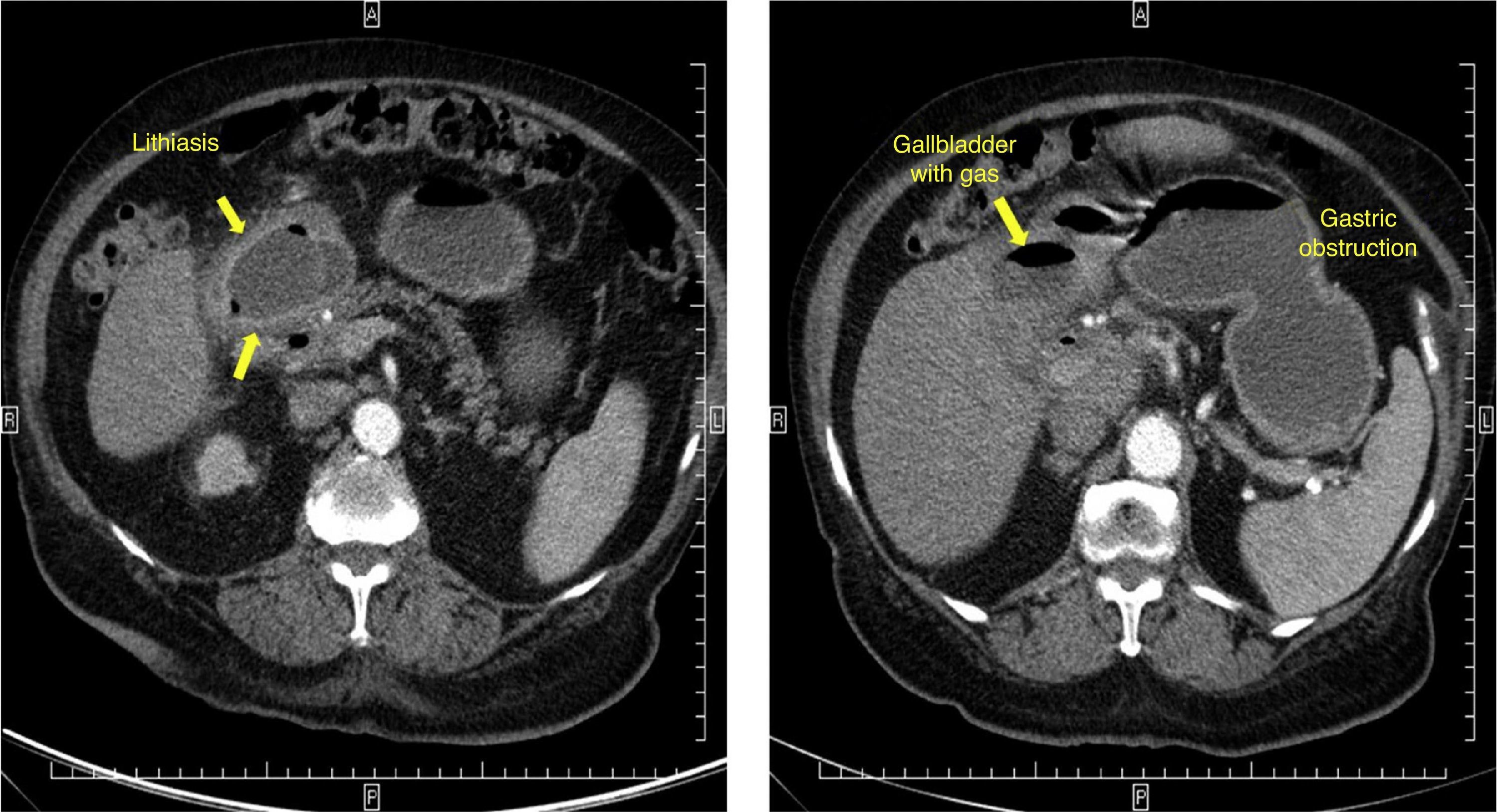
An 86-year-old man sought medical attention for epigastric pain and vomiting with food remains for several days associated with general malaise and dehydration. Physical examination revealed mild epigastric pain with tympanism. Laboratory work-up reported hemoglobin 16.3g/dL, urea 133mg/dl, creatinine 3.20mg/dl, lactate 2.14 mmol/L, and CRP 189.6mg/L. A plain abdominal x-ray showed gastric dilation. Upper endoscopy revealed a dilated stomach with abundant fluid. A large stone was found over the pylorus and duodenum that impeded the passage of the endoscope. An attempt to fragment the stone was unsuccessful. A CT scan also identified the presence of a stone, along with gas in the gallbladder. A pyloroduodenotomy with stone extraction and transverse duodenorrhaphy with the Heineke-Mikulicz technique were performed, but not a cholecystectomy. There were no postoperative complications and the patient was released from the hospital (fig. 1).
Bilioenteric fistula is present in 2-3% of the cases of cholelithiasis.1 This communication allows the stone to enter the intestine causing a bowel obstruction known as gallstone ileus. The majority of the fistulas are cholecystoduodenal, followed by cholecystocolic and cholecystogastric fistulas. Nevertheless, the stones are small and eliminated without causing obstruction. Only 6% of fistula-associated stones cause obstruction. The most frequent occlusion site is the small bowel. When the stone is lodged at the level of the duodenum, obstructing the gastric outlet, it is called Bouveret's syndrome, and it represents only 1-3% of the cases of gallstone ileus.2,3 The syndrome was named after the French physician, Leon Bouveret, who published 2 cases of the pathology in 1896.4
Bouveret's syndrome is more frequent in elderly women and it presents with nausea, vomiting, and epigastric pain. There can be gastrointestinal bleeding in severe cases. The most frequent complication is hydroelectrolytic imbalance.1,5 Diagnosis is delayed, given that patients do not have a history of cholelithiasis and the symptoms are non-specific. It can be confused with other causes of gastroduodenal obstruction, and so differential diagnosis must be made with bezoar, foreign body impaction, gastric volvulus, tumor, peptic stricture, superior mesenteric artery syndrome, etc. Plain abdominal x-ray can sometimes identify the Rigler triad (intestinal obstruction or gastric dilation, pneumobilia, and ectopic stone visualization).1,3 Endoscopy is diagnostic in 70% of the cases.4 Endoscopic stone extraction can be attempted, but it may not be possible if the stone is larger than 2.5cm. Surgery is the treatment of choice. There are 2 alternatives: one-stage surgery (with enterotomy, stone extraction, and cholecystectomy with fistula repair) or simple enterotomy and stone extraction. The combined surgery has been associated with higher postoperative mortality rates (20-30%), compared with cases of duodenotomy alone (6-12%).4 Gallstone ileus recurrence (less than 5%) or biliary symptom persistence (10%) are low.1,3
In conclusion, Bouveret's syndrome is rare and therefore diagnosis is by exclusion. The ideal treatment is endoscopic, but if that fails, then surgery is necessary.
Financial disclosureNo financial support was received in relation to this study/article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Ruiz de la Hermosa A, Ortega-Domene P, Zarzosa-Hernández G, Seoane-González JB. Síndrome de Bouveret, una causa infrecuente de obstrucción duodenal. Revista de Gastroenterología de México. 2016;81:55–56.