Cancer is the result of the interaction of genetic and environmental factors. It has recently been related to viral infections, one of which is human papillomavirus. The aim of the present study was to describe the frequency of human papillomavirus infection in patients with digestive system cancers.
Materials and methodsA prospective, multicenter, observational study was conducted on patients with gastrointestinal cancer at 2public healthcare institutes in Veracruz. Two tumor samples were taken, one for histologic study and the other for DNA determination of human papillomavirus and its genotypes. Anthropometric variables, risk factors, sexual habits, tumor location, and histologic type of the cancer were analyzed. Absolute and relative frequencies were determined using the SPSS version 24.0 program.
ResultsFifty-three patients were studied. They had gastrointestinal cancer located in: the colon (62.26%), stomach (18.87%), esophagus (7.55%), rectum (7.55%), and small bowel (3.77%). Human papillomavirus was identified in 11.32% of the patients, 66.7% of which corresponded to squamous cell carcinoma and 33.3% to adenocarcinoma. Only genotype 18 was identified. Mean patient age was 61.8±15.2 years, 56.60% of the patients were men, and 43.40% were women. A total of 15.8% of the patients had a family history of cancer and 31.6% had a personal history of the disease, 38.6% were tobacco smokers, and 61.4% consumed alcohol. Regarding sex, 5.3% of the patients said they were homosexual, 3.5% were bisexual, 29.8% engaged in oral sex, and 24.6% in anal sex.
ConclusionsOur study showed that human papillomavirus infection was a risk factor for the development of gastrointestinal cancer, especially of squamous cell origin.
El cáncer es el resultado de la interacción de factores genéticos y ambientales, recientemente relacionados con infecciones virales, entre ellos, el virus del papiloma humano. El objetivo fue conocer la frecuencia de infección por el virus del papiloma humano en las neoplasias del aparato digestivo.
Material y métodosEstudio prospectivo, multicéntrico y observacional en pacientes con cáncer del aparato digestivo en 2instituciones del sector salud de Veracruz. Se realizó toma de 2muestras del tumor: una para realizar estudio histológico y otra para determinación del ADN del virus del papiloma humano y sus genotipos. Se analizaron: variables antropométricas, factores de riesgo, hábitos sexuales, localización y variedad histológica de la neoplasia. Se determinaron frecuencias absolutas y relativas utilizando el programa SPSS versión 24.0.
ResultadosSe estudió a 53 pacientes con cáncer de aparato digestivo localizado en el colon (62.26%), estómago (18.87%), esófago (7.55%), recto (7.55%) e intestino delgado (3.77%). En el 11.32% de ellos se identificó la presencia de virus del papiloma humano, de los cuales el 66.7% correspondió a carcinoma epidermoide y el 33.3% a adenocarcinoma. Únicamente se identificó el genotipo 18. La edad promedio del grupo fue 61.8±15.2 años. El 56.60% correspondió al género masculino y el 43.40% al femenino. El 15.8% refirieron antecedentes oncológicos familiares y el 31.6%, personales. El 38.6% mencionaron tabaquismo y el 61.4%, alcoholismo. El 5.3% declararon ser homosexuales y el 3.5%, bisexuales. El 29.8% manifestaron relaciones orales y el 24.6%, anales.
ConclusionesNuestro estudio muestra que la infección de virus del papiloma humano es un factor de riesgo para el desarrollo de neoplasias del aparato digestivo, sobre todo de origen epidermoide.
Cancer is the result of the interaction of genetic and environmental factors that lead to cell degeneration, causing precancerous lesions and ending in malignant neoplasias. An increase has been observed in the incidence of neoplasias directly or indirectly related to viral agents. They include the hepatitis B virus and the hepatitis C virus, as well as the human papillomavirus (HPV), representing approximately 20% of cancer deaths, worldwide.1–3
Currently, HPV infection is the most common across the world. Different unsafe sexual practices, beginning an active sex life at an early age, and numerous sexual partners are among the risk factors explaining its increased incidence. The prevalence of HPV infection has been reported to be augmented in smokers, as well as associated with non-genital cancer.2,4
More than 130 types of HPV have been identified that are classified as high-risk or low-risk, depending on their malignancy potential during the course of persistent infection. High-risk HPVs are those that are strongly associated with premalignant and malignant lesions and they include types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 73, and 82. Types 16 and 18 have the greatest worldwide prevalence. The low-risk HPVs are those associated with anogenital warts (benign, hyperproliferative lesions with a very limited tendency toward malignant progression) and they are types 6, 11, 40, 42, 43, 44, 53, 54, 61, 72, and 81.5,6
HPV infection in the United States is estimated to be responsible for 90% of anal cancers, 65% of vaginal cancers, 50% of vulvar cancers, 35% of penile cancers, and 45-90% of oropharyngeal cancers.7,8 Other reports relate HPV with squamous cell carcinoma (SCC) located in the head and neck that present in the oral cavity, nasopharynx, oropharynx, larynx, and hypopharynx.9,10 In 1983, Syrjanen et al. suggested the possibility of HPV having an etiologic role in SCC upon the immunohistochemical detection of HPV structural proteins in 6 cases of squamous cell oral carcinoma.11 HPV has been found in 23 to 35% of all SCC biopsies over the world. The majority of HPV-positive cancers arising in the oropharynx have been detected in the tongue and amygdalae, representing 45 to 90% of cases. HPV types 16 and 18 are the genotypes that have been associated in the majority of cases of oral cavity and oropharyngeal cancers, similar to that occurring in cervical cancer, although types 31, 33, 35, 45, 51, 52, 58, 59, and 68 have also been found.12
The main risk factors for esophageal cancer that have been identified are chronic gastroesophageal reflux and its most severe manifestation, Barrett's esophagus. Alcohol consumption and tobacco smoking have also been associated. However, it is possible that HPV infection in the stratified epithelium and the intestinal metaplasia has a proliferative, anti-apoptotic effect that intensifies the inflammatory response and triggers the neoplastic transformation of the esophageal mucosa.13–15
Other segments of the digestive tract covered by glandular epithelium have apparently not been so widely studied, and the reported cases associated with HPV are exceptional.11–13
The aim of the present study was to establish the frequency of HPV in relation to the different malignant neoplasias affecting the gastrointestinal tract.
Materials and methodsA prospective, multicenter, comparative, observational, and descriptive study was conducted on patients with cancer of the gastrointestinal tract seen at public health institutes in the city of Veracruz (the Unidad Médica de Alta Especialidad de la Secretaría de Salud, U.M.A.E, Centro Médico Nacional No 14 “Adolfo Ruiz Cortines” of the Instituto Mexicano del Seguro Social, and the Instituto de Investigaciones Médico-Biológicas of the Universidad Veracruzana), within the time frame of October 2013 and March 2016.
After obtaining informed consent from the patients, 2 samples were taken from the tumor site. One sample was used for the histopathologic study with hematoxylin-eosin and special stains and the other for HPV molecular determination. The latter was carried out using 100 ng of DNA, amplifying a fragment of the L1 region (amplicon: 450 pb) of the viral genome with the MY09-MY11 oligonucleotides (0.4μM) through the polymerase chain reaction (PCR) technique. The constitutive ß-Globin gene (amplicon: 248 pb), with the GH20-PC04 oligonucleotides (0.4μM), was amplified as the DNA integrity control. The negative samples were re-amplified using 0.2μM of the GP5-GP6 internal oligonucleotides (amplicon: 150 pb) from 2μl of the MY09-MY11 PCR product to corroborate the absence of HPV. In addition, a fragment of the E6/E7 regions was amplified, which served as a template for the detection of the HPV 16 and 18 genotypes through nested PCR. The amplicons were analyzed through electrophoresis, using agarose gel at 2%, stained with 0.5μg/ml of ethidium bromide.
The anthropometric variables (age, sex), risk factors (family history of cancer, personal history of cancer, smoking, and consumption of alcohol and carcinogenic agents), sexual habits and conduct, lesion location, and histopathologic study result were analyzed in each case.
The study followed the General Health Law Norms and the Helsinki Declaration and was approved by the ethics committee of the School of Medicine of the Universidad Veracruzana.
For the statistical analysis, absolute and relative frequencies were used to describe the nominal variables and mean and standard deviation were used to determine their distribution. The SPSS version 24.0 (SPSS, Inc, Chicago, IL, USA) software was employed.
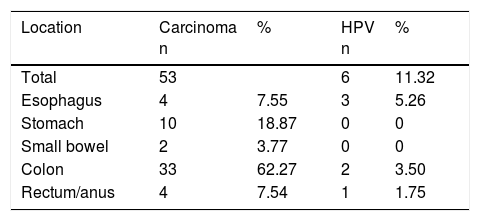
ResultsFifty-three patients diagnosed with gastrointestinal cancer were studied. Four cases (7.55%) were located in the esophagus, 10 (18.87%) in the stomach, 2 (3.77%) in the small bowel, 33 (62.27%) in the colon, and 4 (7.54%) in the anus/rectum. Of those cases, HPV was detected in 6 (11.32%) cases: 4 cases (66.67%) in the stratified epithelium (3 in the esophagus, 1 in the anorectal region) and 2 cases (33.33%) in the glandular epithelium of the colon. Likewise, in a control group of 55 cases carried out simultaneously in subjects with no digestive tract neoplasia, HPV was identified in 2 cases in the colonic mucosa, for a prevalence of 3.64%. HPV DNA studies corresponded to genotype 18 in all the cases of neoplasia and in the colonic mucosa of normal subjects. Genotype 16 was not identified in any of the cases (Table 1).
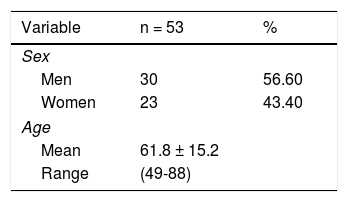
The mean age of the group was 61.8 ± 15.2 years (range: 49-88). There was a predominance of men at 56.6% of the patients, over women at 43.4% (Table 2).
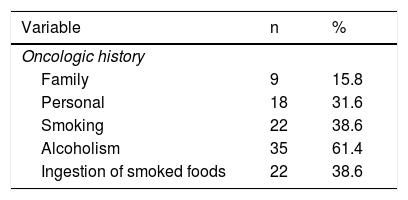
Among the risk factors in the group, 22 patients (38.6%) smoked tobacco and ingested smoked foods, 35 cases (61.4%) consumed large quantities of alcohol, 9 patients (15.8%) had a family history of cancer, and 28 cases (31.6%) had a personal history of cancer (Table 3).
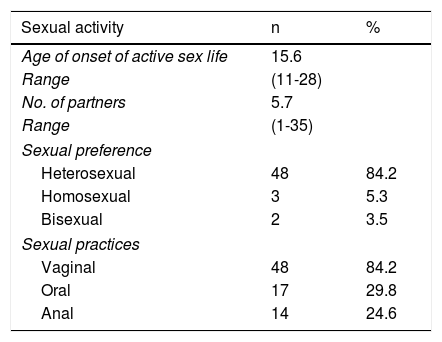
Active sex life of the patients began at a mean 15.6 years (range: 11-28) and the mean number of sexual partners was 5.7 (range: 1-35). Sexual preference was heterosexual in 84.2% of the cases, homosexual in 5.3%, and bisexual in 3.5%. A total of 29.8% patients stated they had engaged in oral sex and 24.6% in anal sex (Table 4).
Characteristics of patient sexual preference and sexual practice.
| Sexual activity | n | % |
|---|---|---|
| Age of onset of active sex life | 15.6 | |
| Range | (11-28) | |
| No. of partners | 5.7 | |
| Range | (1-35) | |
| Sexual preference | ||
| Heterosexual | 48 | 84.2 |
| Homosexual | 3 | 5.3 |
| Bisexual | 2 | 3.5 |
| Sexual practices | ||
| Vaginal | 48 | 84.2 |
| Oral | 17 | 29.8 |
| Anal | 14 | 24.6 |
According to the 2012 International Association of Cancer Registries’ GLOBOCAN project, malignant neoplasias of the gastrointestinal tract hold a high place worldwide, together with bronchogenic cancer and prostate cancer in men and breast cancer and cervical cancer in women.14 Mexico is no exception. According to the INEGI, cancer is the third cause of death, only after cardiovascular diseases and diabetes mellitus. In 2015, 13.5% of the total of deaths occurred from malignant tumors. A total of 147,985 new cases and 91,248 deaths were registered in patients between 45 and 65 years of age. There was a predominance in women (55.72%) and tumors affecting the gastrointestinal tract were in third place in both sexes. According to estimates, annual incidence and death-by-cancer will have increased by 49.8% in Mexico in 2025.15
Malignant tumor etiology is multifactorial and has included different environmental factors, such as diet, exposure to toxins, ingestion of carcinogenic agents, infectious diseases, and inflammatory states, especially in genetically predisposed individuals. A growing number of cancers directly or indirectly related to viral infections has been observed in recent years that are the final result of alterations in the signaling pathways and in the control of cell growth. HPV study has received special interest worldwide, given that it is one of the most frequent sexually transmitted diseases on an international scale that is known to be related to genital cancer. It is a double-chain DNA virus with approximately 8,000 base pairs associated with histones. It has no covering, it is 50-55 nanometers in diameter, and has an icosahedral capsid composed of 72 capsomeres, and depends on a cell host for its replication. The viral genome possesses codifying regions of proteins, among which are the early-expression or early-region genes (E1 to E8 depending on the viral type) that are necessary for viral replication and two late-expression genes (L1 y L2) that are in charge of encoding the structural proteins and the early-region gene is responsible for malignant transformation.16,17
HPV preferably established itself in the stratified epithelium of the skin and anorectal tract and has recently been considered a risk factor for malignant neoplasia of the digestive tract with epithelial mucosa. The transition zone of the anal canal is anatomically and embryologically similar to that of the uterine neck, which is why the neck is thought to be more susceptible to the oncogenic effects of HPV. The prevalence of HPV is 71% in invasive anal cancer and 78% in SCC, with HPV type 16 being found more frequently (85%), followed by type 18 (7%) and other types that include 33, 31, and 45. Risk factors are a previous history of HPV-related cancers, high-risk sexual habits, and an immunosuppressive state. Human immunodeficiency virus (HIV) stands out among the immunosuppressive states and numerous genotypes have been found in those patients, such as 53, 58, 61, and 70.18,19
HPV has also been identified in SCCs of the head and neck, particularly in the oral cavity and esophagus, with HPV association at 20 to 29%. The histologic similarities between the oral squamous epithelium and esophageal squamous epithelium are thought to resemble the anorectal tract conditions, and genotypes 16 and 18 have been more frequently identified at both sites in different studies.20,21
In a meta-analysis of 37 studies that included 2,630 cases of adenocarcinoma of the colon, Baandrup et al. recently found a HPV prevalence of 11.2%, with variations in different geographic regions. The highest prevalence was in South America, Asia, and the Middle East. They also found a prevalence of adenomatous polyps of 5.1% and of 1.6% in healthy controls. The oncogenic effect in the colonic mucosa has not yet been determined.22
We found a HPV frequency of 11.32% in the study population, confirming the data published in different case series. Tumor location in our patients corresponded to segments covered with stratified epithelium in 66.67% of the cases, with a preference for the esophagus and the anorectal region. However, 33.33% of the tumors were found in the glandular epithelium of the colon. There were 2 cases of location in the colon in the healthy controls from 55 samples taken, signifying a prevalence of 3.64%. The genotype detected was type 18, contrasting with the information published for our region that shows the predominant genotype to be type 16.
The anthropometric characteristics of the study population corresponded to those of patients with malignant neoplasias. Mean patient age was 61.8 ± 15.2 years (range 49-88) and there was a predominance of men. The risk factors identified were tobacco smoking and the ingestion of smoked foods in 38.6% of the patients, alcohol consumption in 61.4%, a family history of cancer in 15.8%, and a personal history of cancer in 31.6%. Those figures are similar to results published in different studies.
Sexual conduct has been considered a primordial factor in the transmission of HPV infection. In the present study, onset of an active sex life at 15 years of age was similar to the mean reported in our geographic region, but 84.2% of the patients were polygamous and had a mean of 5.7 sexual partners. A total of 5.3% of the patients were homosexual and 3.5% were bisexual. A high number of patients engaged in oral sex (29.8%) and anal sex (24.6%), both of which are closely related to acquiring the infection.
In conclusion, different articles have demonstrated the association between human papillomavirus infection and gastrointestinal neoplasias and our study results confirm that relation, especially with respect to the squamous cell variety. However, there is no clear hypothesis that explains the relation of HPV to cancers arising in the glandular epithelium. The sexual conduct and sexual preference of the individuals identified in our study play a fundamental role in the chain of disease transmission. We believe a larger number of cases is necessary to confirm the data in our preliminary report.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureThis project was financed by the participating institutions.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Roesch-Dietlen F, Cano-Contreras AD, Sánchez-Maza YJ, Espinosa-González JM, Vázquez-Prieto MÁ, Valdés-de la O EJ, et al. Frecuencia de infección por virus del papiloma humano en pacientes con cáncer del aparato digestivo. Revista de Gastroenterología de México. 2018;83:253–258.