Sclerosing mesenteritis makes up part of a spectrum of rare idiopathic conditions characterized by chronic inflammation of the mesentery and fibrosis.1 It was first described in 1924.2 Clinical presentation varies from an asymptomatic abdominal mass to acute systemic syndromes manifested as fever, weight loss, general malaise, bowel obstruction, or intestinal ischemia.
Tomography is a sensitive diagnostic tool, but surgical biopsy is usually necessary for making the diagnosis and ruling out other pathologies. Few patients require surgical treatment, which is generally directed at secondary complications such as bowel obstruction. The epidemiology of sclerosing mesenteritis is unknown. A prevalence of 0.6% has been described from more than 7,000 abdominal computed axial tomography scans.3 The disease is regarded as rare in the pediatric age and only 17 cases have been reported up to the present date.4 Even though there are reports on children under 3 years of age, the majority of patients are in the fifth to seventh decades of life.1
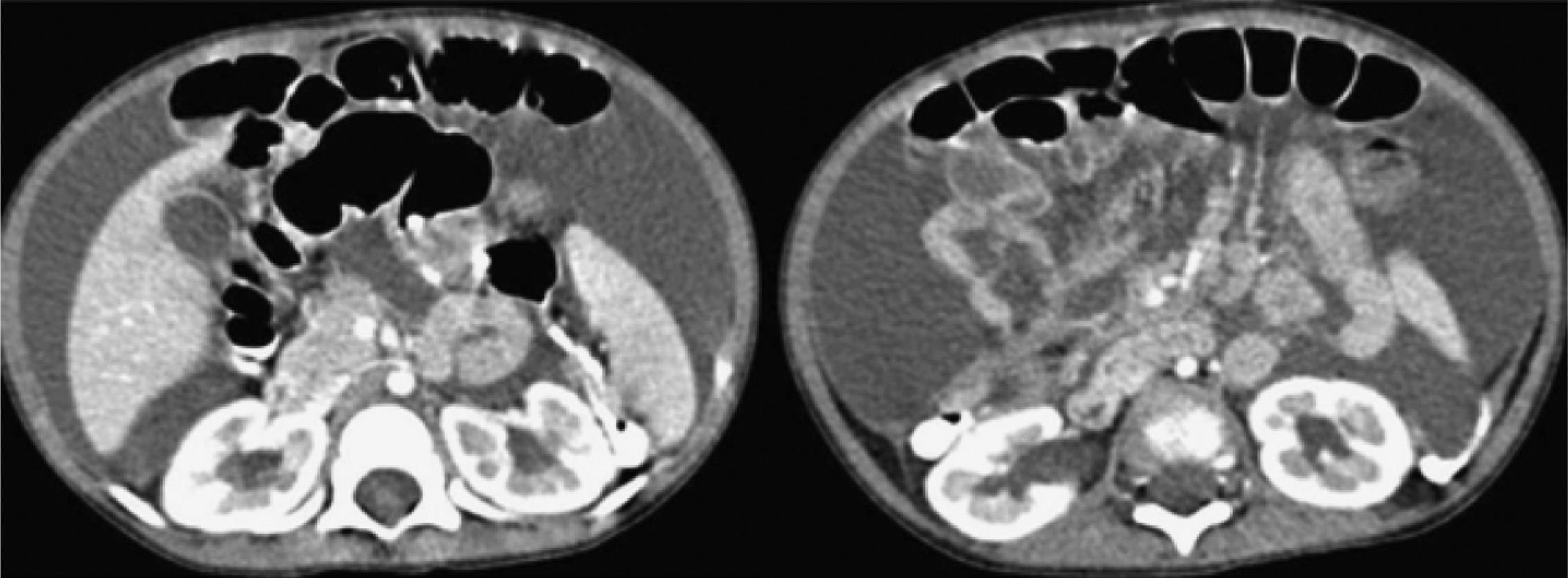
We present the case herein of a 25-month-old male child with a 15-day progression of symptoms that began with abdominal bloating, soft stools, and pain, for which he was hospitalized in order to be tested. An abdominal computerized tomography scan was taken (Fig. 1) that showed important ascites. Paracentesis with fluid analysis was done to look for tuberculosis, but only one positive criterion was found: tuberculin 10mm (the rest were negative), for which latent tuberculosis was diagnosed.
Abdominal tomography scan: A great quantity of ascites of undetermined cause; the liver, pancreas, and kidneys have a normal aspect and size; there is no primary tumor or metastasis and no adenomegaly or masses. The vascular structures have normal caliber and there are no lesions in the digestive tract.
Given that there were no other paraclinical findings to explain the ascitic process, the patient underwent surgery that revealed abundant clear peritoneal fluid, marked distension of the intestinal segments, and whitish patches on the peritoneum from diaphragmatic recesses. Upper gastrointestinal endoscopy and total video colonoscopy were performed that showed grade III esophagitis, antral gastritis, mild duodenitis, and nodular colitis. Biopsies demonstrated micro-abscesses at the distal duodenal level and special stains were negative.
Two weeks after surgery and with no clear diagnosis, the patient's symptoms of abdominal bloating and pain recurred. A control abdominal ultrasound was done that showed evidence again of free fluid in the cavity. A second surgery was decided upon and diagnostic laparoscopy was performed in which samples of the entire thickness of the intestine were taken; this had not been possible in the first surgery because the distension of the segments had not allowed for adequate visualization. Surgery revealed critical stricture of the ileum with severe hardening in almost its entirety. Samples were taken for histopathology and the macroscopic results were: the serous membrane of the distal ileum presented with thickened fibrous areas like a «breastplate», compressing it.
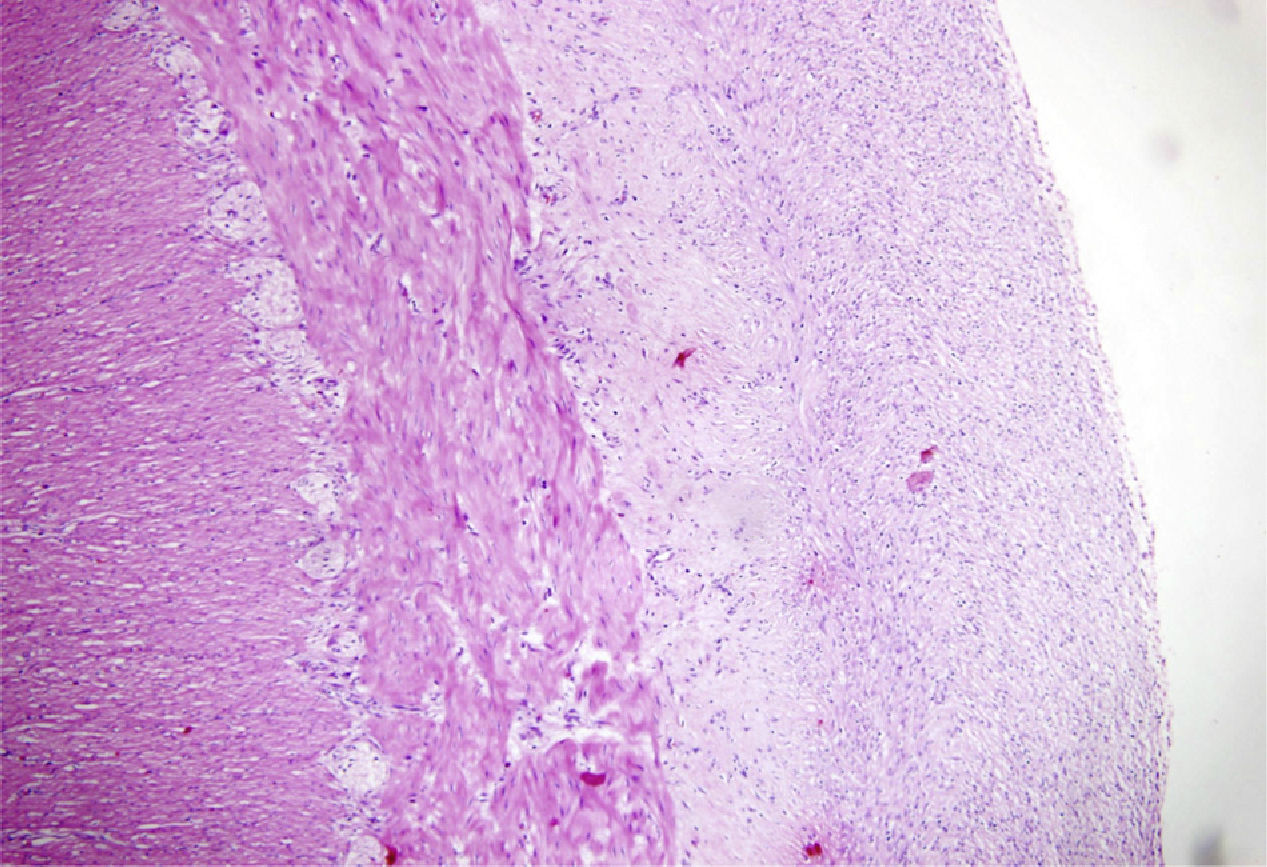
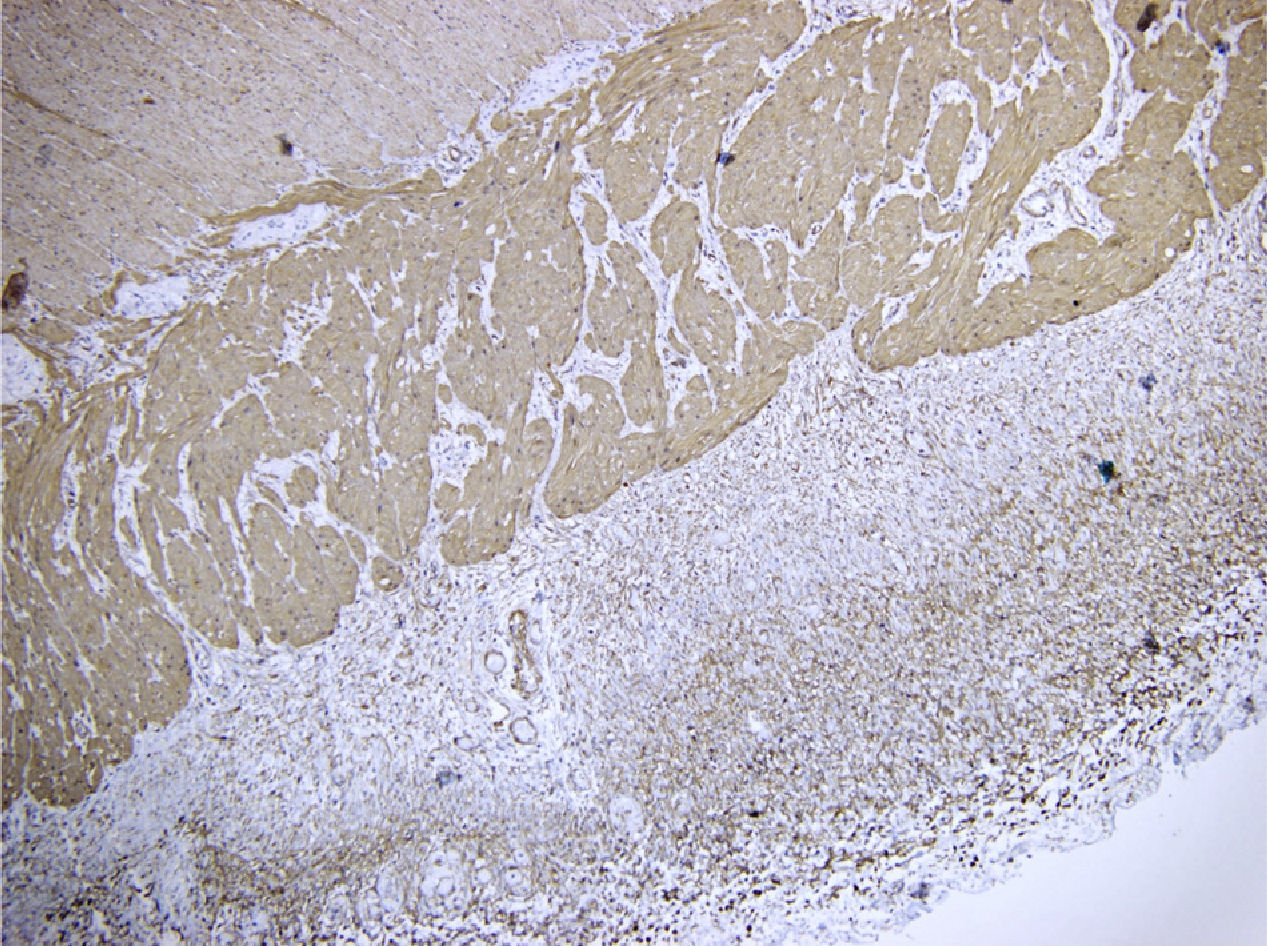
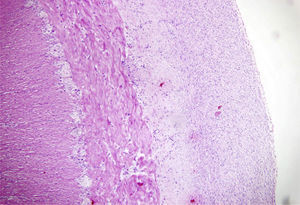
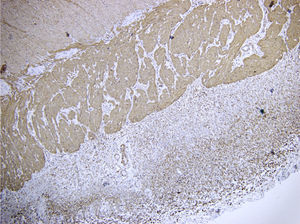
Microscopically: the mucosa, submucosa, and muscle were normal; the serous membrane had a thickened fibrous band that entirely covered the distal ileum resulting in complete stricture and compression. Diagnosis in the distal ileum was idiopathic sclerosing mesenteritis (Figs. 2 and 3).
Systemic steroid therapy was begun, along with isoniazid for 9 months for treating the latent tuberculosis infection. Due to the severity of the clinical symptoms, cyclophosphamide was added. Once treatment was started, the patient progressed adequately, he tolerated oral intake, there were no febrile peaks, and the ascites and distension were resolved.
Given the atypical nature of the clinical symptoms and the immediate improvement, it was decided to continue the steroids for 6 complete weeks, without prolonging cyclophosphamide administration.
It has been suggested in the literature that sclerosing mesenteritis is a rare entity in children and adolescents due to the lower quantity of mesenteric fat,5 and even though the precise etiology is still unexplained, mechanisms including previous abdominal trauma or surgery, autoimmunity, infection, and ischemia have been proposed.6 A reasonable hypothesis is that this subgroup of patients has abnormal responses in the cicatrization and repair of connective tissue. This inflammatory and fibrotic process can affect the integrity of the gastrointestinal lumen and the mesenteric vessels through a mass effect, causing a variety of gastrointestinal and systemic manifestations that include abdominal pain, nausea and vomiting, diarrhea, weight loss, and fever. Therefore a high degree of suspicion is necessary for making the diagnosis.2
Diagnosis is established through histologic evaluation; plain x-ray is non-specific. Ultrasound imaging can aid in better visualizing the mesenteric fat. Computerized tomography scan is the most sensitive image for detection. Calcifications are present in approximately 20% of the lesions as a result of fat necrosis or vascular obstruction.7,8
Pathologic confirmation should be obtained in all cases, as was the case with our patient. It was the basis for establishing the definitive diagnosis.
There is no standard therapy and treatment should be individualized. In the large majority of cases, complete surgical resection is impossible due to the associated vascular involvement and disease extension.
A number of pharmaceutical agents have been used in an attempt to stabilize the disease. Glucocorticoids, azathioprine, methotrexate, colchicine, cyclophosphamide, and/or radiotherapy have been proposed as therapeutic options.1,9,10 The patients with a greater inflammatory component, with fever, weight loss, and general malaise appear to be the most receptive to glucocorticoids, alone or in combination. In the case of our patient, the use of the steroid and cyclophosphamide had favorable results in disease improvement and modulation.
Financial disclosureNo financial support was received in relation to this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Parra-Buitrago A, Valencia-Zuluaga N, Rivera-Echeverry J, Contreras-Ramírez M, Vélez-Hoyos A. Mesenteritis esclerosante idiopática en la edad pediátrica: presentación de un caso clínico. 2013;78:255–257.