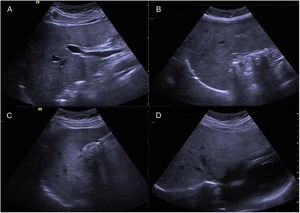
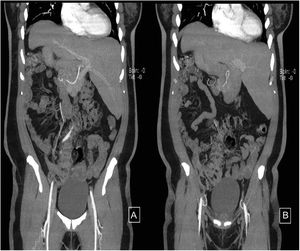
A 44-year-old woman began her illness with colicky epigastric pain that radiated to the right scapula, accompanied by nausea and vomiting. Her leukocyte count was 17,000 and bilirubin values were normal. She sought medical attention at the emergency room of a nonlocal hospital. A laparoscopic cholecystectomy was performed but there were intraoperative difficulties for identifying anatomic structures. The procedure was interrupted and a cholecystostomy tube was placed. She was referred to the Hospital General de México, where new radiologic studies and endoscopic retrograde cholangiopancreatography (ERCP) were carried out. A catheter was identified in the gallbladder, the intrahepatic bile duct was not dilated, and the common bile duct was regular, with a 4 mm diameter. Ultrasound imaging (Fig. 1A–D) and cholangiography through the cholecystostomy tube (Fig. 2A–D) showed a cystic gallbladder with stones, an unaltered intrahepatic bile duct located on the left, no evidence of biliary filling defects, and adequate passage of the contrast medium into the duodenum. The diagnosis of situs inversus was suspected and cholangioresonance imaging (Fig. 3A and B) was carried out, confirming the diagnosis. The study reported gallstones, the presence of a catheter in the gallbladder, and abdominal situs inversus totalis. Laparoscopic cholecystectomy was performed with no complications.
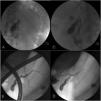
Endoscopic retrograde cholangiopancreatography (ERCP).
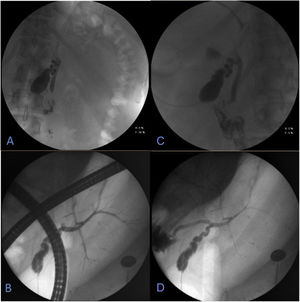
Cholangiography carried out through the “T” tube, with water-soluble contrast medium. A and B) Entrance of contrast medium with opacification of the gallbladder, in a central anatomic position, slightly to the left of the midline. C and D) Cystic gallbladder containing stones and intrahepatic bile duct located on the left, with no alterations, no signs of biliary filling defects, and with adequate passage of the contrast medium into the duodenum.
The authors declare that informed consent was obtained for performing the surgical intervention as therapeutic resolution.
The authors declare that no experiments on humans or animals were carried out for this clinical image.
The authors declare that this article contains no personal information that could identify the patient.
Financial disclosureNo specific grants were received from public sector agencies, the business sector, or non-profit organizations in relation to this clinical image.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Montalvo-Javé EE, Arroyo-Paredes PS, Corona-Torres MJ et al. Colecistectomía laparoscópica en paciente con situs inversus totalis. Rev Gastroenterol Méx. 2022;87:486–488.